Key Takeaways
What is patient engagement: the active involvement of patients in understanding, managing, and making decisions about their own care.
Higher patient activation directly correlates with better health outcomes, according to the CDC.
Disengaged patients are significantly more likely to miss appointments and less likely to follow treatment plans, increasing clinical risk and administrative cost.
Pabau’s automated recall, digital forms, and client portal address the core engagement gaps in independent clinic workflows.
Most clinics lose patients not because their clinical care is poor, but because the experience around it is fragmented. Appointments are confirmed by phone. Intake forms arrive on paper. Post-treatment instructions get forgotten. Patients drift away not from dissatisfaction, but from disconnection. Understanding what is patient engagement and building systems around it is how clinics close that gap.
This guide is written for clinic owners, practice managers, and clinicians running independent or small group practices. It covers the definition of patient engagement, why it affects retention and outcomes, which strategies drive measurable results, and how digital tools support each touchpoint in the patient journey.
What Is Patient Engagement in Healthcare?
Patient engagement describes the degree to which patients actively participate in their own healthcare. It combines a patient’s knowledge, skills, and willingness to manage their condition with the interventions a practice uses to support that participation, as defined by Healthcare IT News. Engaged patients understand their diagnoses, communicate with their providers, attend follow-up appointments, and act on treatment advice between visits.
This is distinct from patient satisfaction, which measures how patients feel about a specific encounter. Engagement is behavioural and ongoing. A patient can be satisfied with a consultation yet still fail to return for a recommended follow-up, forget their aftercare instructions, or never complete the intake process properly. Those are engagement failures, not satisfaction failures.
The FDA’s Center for Devices and Radiological Health frames patient engagement as “intentional, meaningful interactions that provide opportunities for mutual learning and effective collaboration.” For clinic operators, that definition has a practical implication: engagement is something you actively build, not something patients bring with them.
Why What Is Patient Engagement Matters for Clinic Operators
Engagement has a direct line to clinic revenue. Patients who are actively involved in their care return more often, refer more frequently, and are more likely to follow through on treatment packages or membership programmes. Disengaged patients, by contrast, cancel last-minute, request refunds, and generate higher administrative overhead through repeated rescheduling and chasing.
The CDC’s health literacy research confirms that patients with higher activation levels, meaning those with the knowledge, skills, and confidence to participate in their care, have measurably better health outcomes. For chronic condition management, aesthetic treatment plans, and wellness programmes, that outcome difference translates directly to client retention and word-of-mouth growth. Good patient care management starts with understanding where engagement breaks down.
| Engagement Level | Clinical Behaviour | Business Impact |
|---|---|---|
| High | Attends follow-ups, follows care plan, communicates proactively | Higher LTV, more referrals, fewer no-shows |
| Medium | Attends some appointments, inconsistent aftercare compliance | Moderate retention, periodic dropout risk |
| Low | Misses appointments, ignores follow-up, poor treatment adherence | Revenue leakage, higher admin cost, worse outcomes |
Clinics managing chronic conditions, multi-session aesthetic treatments, or membership models feel this most acutely. A dermatology practice running a 6-session laser programme needs consistent patient participation at every stage. An aesthetic clinic with a quarterly Botox client base depends on retention, not just acquisition. Engagement is the operational mechanism that makes either model sustainable.
Patient Activation vs Patient Engagement: What’s the Difference?
These two terms are often used interchangeably, but they describe different things. Patient activation refers to a patient’s internal readiness: their confidence, knowledge, and perceived ability to manage their own health. Patient engagement refers to the actual behaviours that result from that readiness, shaped by both the patient and the practice environment.
Think of activation as a precondition and engagement as the outcome. A patient may have high activation but still disengage if the clinic’s communication processes are poor. Equally, a low-activation patient can be supported into higher engagement through well-designed touchpoints: a clear pre-appointment email, a structured intake form, a follow-up message with specific post-treatment guidance.
For clinic operators, this distinction matters because it shifts responsibility. Activation is largely the patient’s starting point. Engagement is partly yours. Supporting patient compliance with care plans requires designing systems that guide patients, not just hoping they show up motivated. This is where practice management tools become genuinely useful.
Pro Tip
Audit your last 30 appointment cancellations. Separate them into categories: no communication before cancelling, late cancellations, and silent no-shows. The pattern tells you exactly where your engagement system is breaking down and which touchpoints to fix first.
Patient Engagement Strategies That Work in Independent Clinics
Most patient engagement literature targets hospital systems with dedicated patient experience teams. Independent clinics operate differently: smaller teams, fewer resources, and patients who expect a more personal relationship. The strategies that work here are those that automate the low-value touchpoints so the high-value clinical interactions can carry more weight.
1. Streamline Appointment Scheduling and Reminders
Friction at booking is the first engagement failure point. If scheduling requires a phone call during clinic hours, you are filtering out an entire segment of patients who would otherwise book. Online booking removes that barrier. Automated reminders, sent 48 and 24 hours before an appointment, reduce no-shows and give patients enough time to reschedule rather than simply not showing up. Effective appointment scheduling is foundational to everything else in the engagement chain.
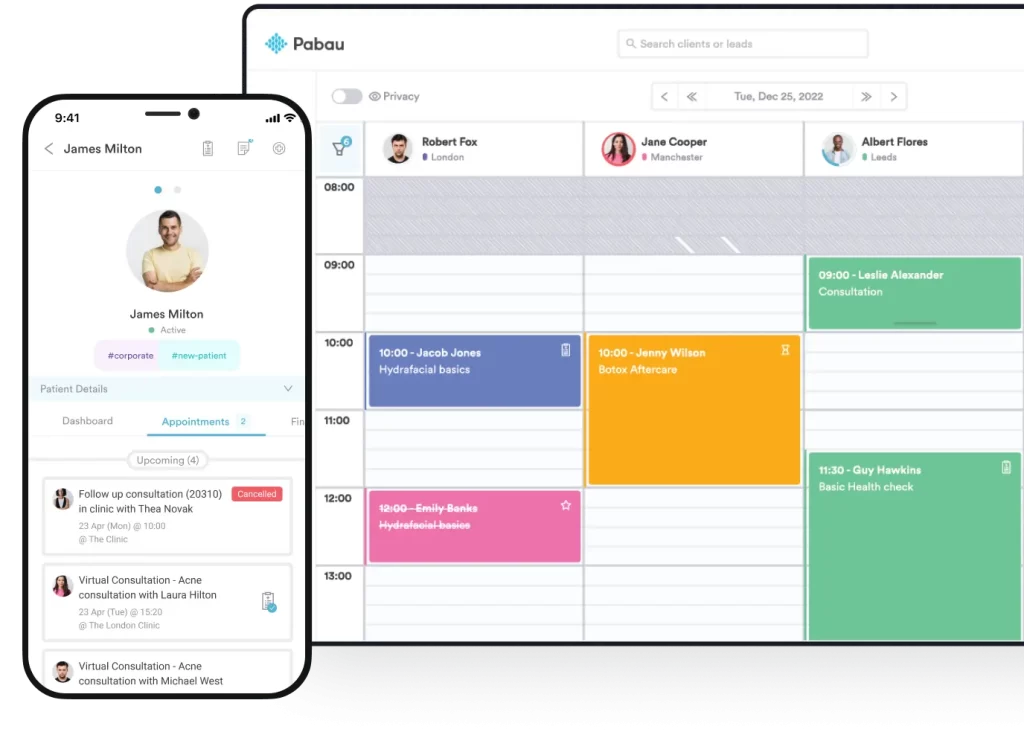
2. Use Digital Intake Forms to Set Expectations Early
Pre-appointment intake is an engagement touchpoint, not just an administrative necessity. When patients complete digital intake forms before they arrive, they have already mentally prepared for the consultation. They have read through their health history, considered their goals, and started thinking about questions to ask. That cognitive preparation increases the quality of the clinical interaction and improves treatment adherence afterwards. Paper forms handed over at reception achieve the opposite: they signal that the clinic’s process is reactive and create a rushed, bureaucratic first impression.
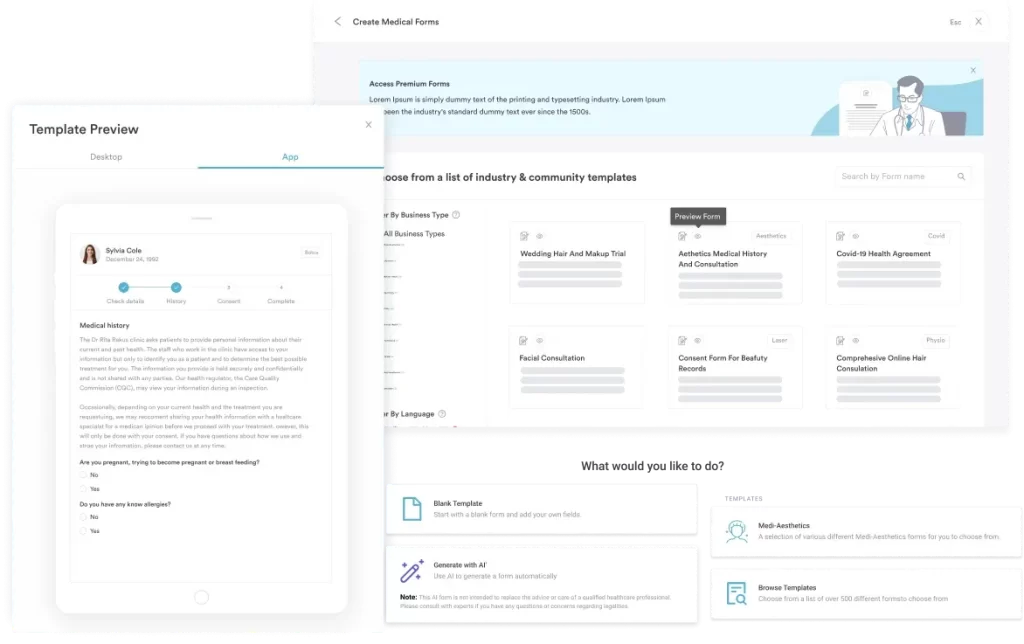
3. Automate Pre- and Post-Care Communication
Post-treatment instructions are where engagement commonly collapses. Patients leave an appointment, receive verbal aftercare guidance they half-remember, and then call back with questions or ignore the guidance entirely. Automated post-care messaging, sent within hours of treatment, reinforces what was said in the room and reduces both patient anxiety and follow-up call volume. Pair this with automated recalls for repeat treatments, and you create a communication loop that keeps patients on schedule without manual intervention. Pabau’s automated workflows handle pre- and post-care sequences, recall scheduling, and appointment reminders in a single system.
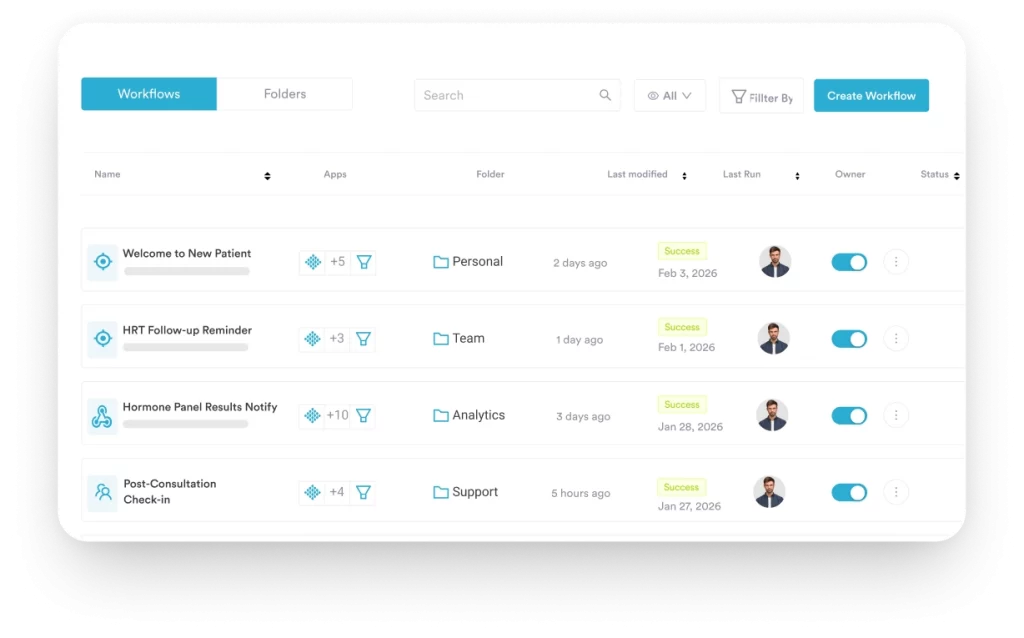
4. Give Patients Access to Their Records
Patient portals increase engagement by giving patients access to their records, invoices, and treatment history outside of appointments. When patients can review their own clinical notes, track their treatment progress, and communicate directly with the clinic through a secure channel, they are more invested in their care. According to ONC data briefs on individuals’ access to electronic health information, approximately 6 in 10 individuals nationwide have been offered and accessed their online medical record, a figure that continues to climb as patient portal adoption grows across both hospital and ambulatory settings. Pabau’s client portal gives patients this access without additional software overhead. The benefits of patient portals extend beyond convenience: they shift patients from passive recipients to active participants in their care.
5. Collect and Act on Patient Feedback
Sending a satisfaction survey after every appointment is table stakes. What matters is what you do with the responses. Clinics that systematically capture patient feedback and route low scores to a follow-up process retain far more at-risk patients than those who survey but never respond. A score of 3 out of 5 with no follow-up communicates that the clinic does not care. A score of 3 out of 5 followed by a personal message from the practice manager communicates the opposite.
See how Pabau supports patient engagement across every touchpoint
From automated recall workflows and digital intake forms to client portals and post-care messaging, Pabau connects every part of the patient journey in one platform built for independent clinics.

What Is Patient Engagement in Digital Healthcare Settings?
Digital patient engagement refers to using technology to replicate and extend the touchpoints that previously required manual effort. This includes online booking, automated reminders, digital consent forms, patient portals, telehealth consultations, and SMS or email campaigns. Each tool targets a specific friction point in the patient journey.
For independent clinics, the practical value of digital engagement is not sophistication but consistency. A solo practitioner cannot personally follow up with every patient who misses a recall. An automated email and SMS campaign triggered by a lapse in appointments can. The technology does not replace the clinical relationship; it protects it by ensuring patients are not simply forgotten between visits.
The intersection of AI and patient experience is also shifting what is possible. AI-assisted clinical notes reduce the documentation burden on practitioners, freeing more time for genuine patient interaction during appointments. When a clinician is not simultaneously writing notes and listening, patient communication quality improves. That improvement is itself an engagement driver.
- Online booking: Removes scheduling friction, increases first-contact conversion
- Automated reminders: Reduce no-shows, give patients time to reschedule proactively
- Digital forms: Prepare patients before appointments, improve intake quality
- Patient portals: Give patients access to records, communications, and invoices
- Post-care messaging: Reinforce treatment instructions, reduce follow-up call volume
- Recall automation: Bring patients back for repeat treatments on the right schedule
- Feedback collection: Identify at-risk patients before they churn silently
How to Measure Patient Engagement in Your Clinic
Engagement is not a feeling. It is measurable. Most practice management systems capture the data you need; the challenge is knowing which metrics to track and what good looks like.
Appointment Attendance Rate
What it is: The percentage of booked appointments that are attended without rescheduling or no-showing.
Why it matters: Clinics with strong engagement systems typically see attendance rates above 85%. A rate below 75% signals a systemic communication problem, not just individual patient unreliability.
Recall Conversion Rate
What it is: The proportion of patients who are recalled for a follow-up or repeat treatment and actually book.
Why it matters: For treatment-based practices, this metric determines lifetime patient value. A Botox client who returns every 3-4 months is worth 3-4x more annually than one who returns once. Low recall conversion typically means the recall message is poorly timed, generic, or being sent through a channel the patient ignores.
Treatment Plan Completion Rate
What it is: For multi-session treatments, the percentage of patients who complete the full recommended course rather than dropping off mid-plan.
Why it matters: Dropout mid-plan is both a clinical risk and a financial one. Patients who do not complete laser resurfacing courses or physiotherapy programmes often see suboptimal results and attribute that to the clinic rather than their own non-completion. Completion rate is one of the strongest proxies for overall engagement health in a practice.
Tracking these metrics consistently requires a system that connects scheduling, communications, and clinical records. That is where measuring patient satisfaction alongside operational metrics gives clinics a complete picture. The best way to improve patient engagement long-term is to identify exactly where in the patient journey the numbers drop off and intervene at that specific point.
Continue your research
Want a practical framework for tracking how patients interact with your clinic? Improve Patient Engagement covers the tactical steps clinics can take to increase participation at every stage of the care journey.
Looking for tools that support patient onboarding and retention? Patient Care Management explains how coordinated care workflows reduce dropout and improve clinical continuity.
Need to understand the role of digital records access in patient engagement? Benefits of Patient Portals outlines how secure portal access shifts patients from passive recipients to active participants.
Ready to see how data-driven satisfaction tracking supports engagement? Measuring Patient Satisfaction details which metrics matter most and how to act on them systematically.
Conclusion
Patient engagement is the operational gap between good clinical care and a clinic that actually retains its patients. Most practices have the clinical expertise. The breakdown happens in the touchpoints around it: the reminder that was never sent, the intake form filled out in the waiting room, the recall that slipped through with no follow-up.
Pabau’s automated recall system, digital intake forms, and client portal address precisely these gaps, giving independent clinics the same engagement infrastructure that larger health systems build with dedicated teams. If patient retention is a priority in your practice, book a demo to see how Pabau’s patient experience management tools work in practice.
Frequently Asked Questions
Patient engagement in healthcare is the active participation of patients in understanding, managing, and making decisions about their own care. It matters because engaged patients have better clinical outcomes, attend more appointments, follow care plans more consistently, and generate higher lifetime value for clinics. The CDC has confirmed the link between patient activation and measurable health outcome improvements.
Patient experience is a patient’s perception of a specific interaction with a clinic: how they felt during the appointment, whether staff were friendly, whether the environment was comfortable. Patient engagement is behavioural and ongoing: whether the patient returns, follows their care plan, completes their treatment programme, and communicates proactively. You can have a great patient experience score and still have low engagement.
Examples include completing pre-appointment intake forms digitally, responding to SMS appointment reminders, accessing treatment records through a patient portal, following post-care instructions sent automatically after treatment, booking their own recall appointments online, and completing post-visit satisfaction surveys. Each of these is a measurable engagement touchpoint that a clinic can track and optimise.
Focus on automating the communication touchpoints that currently rely on manual effort: appointment reminders, post-care instructions, and recall messaging. Replace paper intake with digital forms patients complete before arriving. Give patients access to their own records through a portal. Collect feedback systematically and follow up on low scores. These four changes address the most common engagement drop-off points without requiring additional staff.
Patient activation refers to a patient’s internal readiness: the knowledge, confidence, and skills they have to manage their own health. Engagement is what actually happens in practice. A highly activated patient who encounters a poor clinic communication process may still disengage. Clinics cannot fully control activation, but they can build systems that support engagement regardless of a patient’s starting activation level.










