Key Takeaways
Highly activated patients (PAM Level 4) have approximately 43% lower rates of 30-day post-discharge hospital utilization than the lowest activation patients (PAM Level 1), per Boston Medical Center research published in JGIM (Mitchell et al., 2014; incident rate ratio 1.75, 95% CI 1.18-2.60).
The global patient engagement solutions market is projected to reach USD 194.18 billion by 2034, growing at a 21.38% CAGR, signalling major industry investment.
Practices that deploy automated recall, digital intake, and two-way messaging see measurable reductions in no-show rates and stronger patient retention.
Pabau’s client portal, automated workflows, and recall tools give clinics a direct operational lever for improving engagement metrics across every patient touchpoint.
Most practices think patient engagement is a patient problem. The data says it is an operational one. When a clinic lacks automated reminders, digital intake, or a structured recall system, patients disengage because friction accumulates at every touchpoint. Understanding current patient engagement statistics is less about benchmarking satisfaction scores and more about identifying exactly where that friction lives. This guide covers the key data points, what they mean for everyday clinic operations, and how to improve patient engagement with the systems already available to you.
Key Patient Engagement Statistics Every Clinic Should Know
The headline figures on patient engagement statistics point consistently in one direction: clinics that invest in structured engagement infrastructure outperform those that rely on ad-hoc communication. The numbers below come from government health agencies, peer-reviewed research, and market analysis firms. They span hospital systems and smaller practices alike, though the operational lessons apply across the board.
- Approximately 43% lower rates of 30-day post-discharge hospital utilization among highly activated patients (PAM Level 4) compared to the lowest activation patients (PAM Level 1), per the Boston Medical Center study published in the Journal of General Internal Medicine (Mitchell et al., 2014; incident rate ratio 1.75, 95% CI 1.18-2.60; PMID: 24091935), as cited in the CDC Health Literacy Research Summary, June 2024.
- USD 194.18 billion projected global market size for patient engagement solutions by 2034, growing at a 21.38% compound annual growth rate (Fortune Business Insights, 2026).
- 70% of US non-federal acute care hospitals enabled patient access through FHIR-based apps in 2024, up from 57% in 2021, with standards-based API access growing 23% over the same period (ONC Health IT Data Brief, November 2025).
- mHealth app market projected to reach $86.37 billion by 2030, growing at a 14.9% CAGR (Grand View Research, 2024).
These figures represent substantial capital flowing into patient engagement infrastructure. For clinic owners evaluating whether to invest in digital tools, the market trajectory removes much of the uncertainty. The question is not whether engagement technology matters. It is which tools deliver measurable results at the practice level.
The ONC data is particularly telling. Growth across US hospitals in Health IT-enabled engagement capabilities between 2021 and 2024 reflects a shift from engagement as a nice-to-have to engagement as an operational standard, driven in part by value-based care (VBC) requirements tied to CMS reimbursement frameworks. Practices participating in VBC arrangements that lack engagement infrastructure face a compounding disadvantage: lower quality scores, weaker patient retention, and reduced reimbursement eligibility.
What the Data Shows About Digital Tools and Patient Portals
Digital engagement channels now drive the majority of measurable patient interaction outside the consulting room. Patient portal software sits at the centre of this shift, but the data reveals important nuance about adoption patterns and where portals actually move the needle.
Portal adoption continues to grow, but access alone does not equal engagement. Research from the ONC shows that US hospitals rapidly expanded their FHIR-enabled app capabilities between 2021 and 2024, giving patients the technical ability to access health information through third-party applications. However, the gap between access provision and active patient use remains a persistent challenge across both hospital and private practice settings.
Two signals from the data stand out for smaller practices:
- Appointment reminders via SMS or email consistently rank as the highest-ROI engagement touchpoint for reducing no-show rates, often more impactful than portal access alone.
- Two-way patient messaging drives stronger treatment plan adherence than one-way notifications, because patients can ask questions before an appointment rather than cancelling due to uncertainty.
The practical implication: practices that deploy automated, multi-channel communication alongside portal access see better engagement outcomes than those that launch a portal and assume patients will use it. A portal is infrastructure. What drives usage is the workflow built around it. Clinics should also capture patient feedback systematically to understand which channels their specific patient base actually responds to, because preferences vary significantly across age groups and care settings.
Online reputation now functions as a discovery channel in its own right. Yext research found that businesses with 4-5 star ratings rank approximately 9% higher in Google’s local pack than 2-3 star competitors, meaning star ratings directly affect whether prospective patients see a clinic at all when searching locally. Patient reviews, before-and-after photos, and social proof signals shape evaluation before a booking is ever made. Clinics that can reduce no-show rates and improve attendance through better pre-appointment communication will also naturally generate more satisfied patients who are likely to leave positive reviews, compounding the visibility advantage over time.
See How Pabau Handles Patient Engagement End to End
Pabau's automated workflows, client portal, and recall tools give clinics a measurable lever for improving engagement at every touchpoint. Book a demo to see it in action.

How Patient Activation Levels Shape Clinical Outcomes
The Patient Activation Measure (PAM) is one of the most rigorously validated tools for quantifying engagement. Developed as a standardised assessment, the PAM scores patients on a scale of 0 to 100 across four activation levels, reflecting a progression from passive acceptance of care to proactive self-management. The CDC’s Health Literacy research summary cites a 2015 study showing that PAM scores predicted both health outcomes and healthcare costs over time, not just at a single point.
Understanding the four activation levels gives clinics a framework for segmenting their patient base by engagement risk:
| PAM Level | Patient Behaviour Profile | Engagement Risk | Clinic Response |
|---|---|---|---|
| Level 1 | Passive; relies entirely on provider for decisions | Highest | Structured outreach, simplified instructions |
| Level 2 | Aware but lacks confidence to act on knowledge | High | Educational content, goal-setting support |
| Level 3 | Beginning to take action but inconsistent | Moderate | Recall automation, progress check-ins |
| Level 4 | Proactive; maintains healthy behaviours under stress | Low | Maintenance touchpoints, loyalty programmes |
For private clinics and aesthetics practices, the PAM framework translates directly into recall strategy. Patients at Level 1 and 2 need more structured outreach to attend follow-up appointments. Patients at Level 3 and 4 respond better to value-led communications, such as treatment outcome updates or loyalty rewards. A single-message approach to all patients wastes clinic capacity and leaves the highest-risk patients underserved.
Measuring patient satisfaction alongside PAM-style segmentation gives clinics two complementary data streams: one for predicting behaviour (PAM) and one for assessing perception (satisfaction scores). Neither alone tells the full story. Together, they identify whether a patient is both willing and satisfied enough to return.
Pro Tip
Audit your recall list quarterly and segment patients by appointment history. Patients who have missed two or more appointments without rebooking are your highest-disengagement risk group. Flag these contacts for a dedicated re-engagement sequence using two-way messaging rather than standard broadcast reminders.
Where Smaller and Private Clinics Fit Into the Engagement Picture
Most published patient engagement statistics draw from hospital systems and large multi-location practices. The data for smaller clinics, aesthetics practices, wellness centres, and private GP surgeries is sparse by comparison. This gap matters because the engagement dynamics are genuinely different.
In cash-pay and elective care settings, engagement is primarily a retention and revenue problem rather than a clinical outcomes problem. A medical spa that loses a third of its Botox clients between treatments is not facing a health crisis. It is facing a revenue gap that compounds over 12 months. Patient engagement statistics from hospital settings do not directly map to this context, but the underlying principles do:
- No-show rates in private clinics typically range from 10-30%, with practices lacking automated reminders sitting at the higher end. Each no-show in a 60-minute appointment slot represents direct lost revenue.
- Recall compliance for aesthetic treatments (Botox, fillers, laser) depends almost entirely on proactive outreach. Unlike GP appointments driven by symptoms, elective treatments require the practice to initiate the next booking.
- Patient lifetime value in aesthetics and wellness settings correlates strongly with engagement frequency. Clients who receive pre-care, post-care, and follow-up communications between appointments spend more and refer more.
The patient experience management gap between large and small practices is partly a technology gap. Hospital systems have IT departments, dedicated engagement platforms, and CMS-mandated digital capabilities. Smaller clinics need tools that deliver similar results without enterprise-level overhead. This is where integrated practice management platforms that combine scheduling, recall, digital forms, and messaging in one system offer a structural advantage over fragmented point solutions.
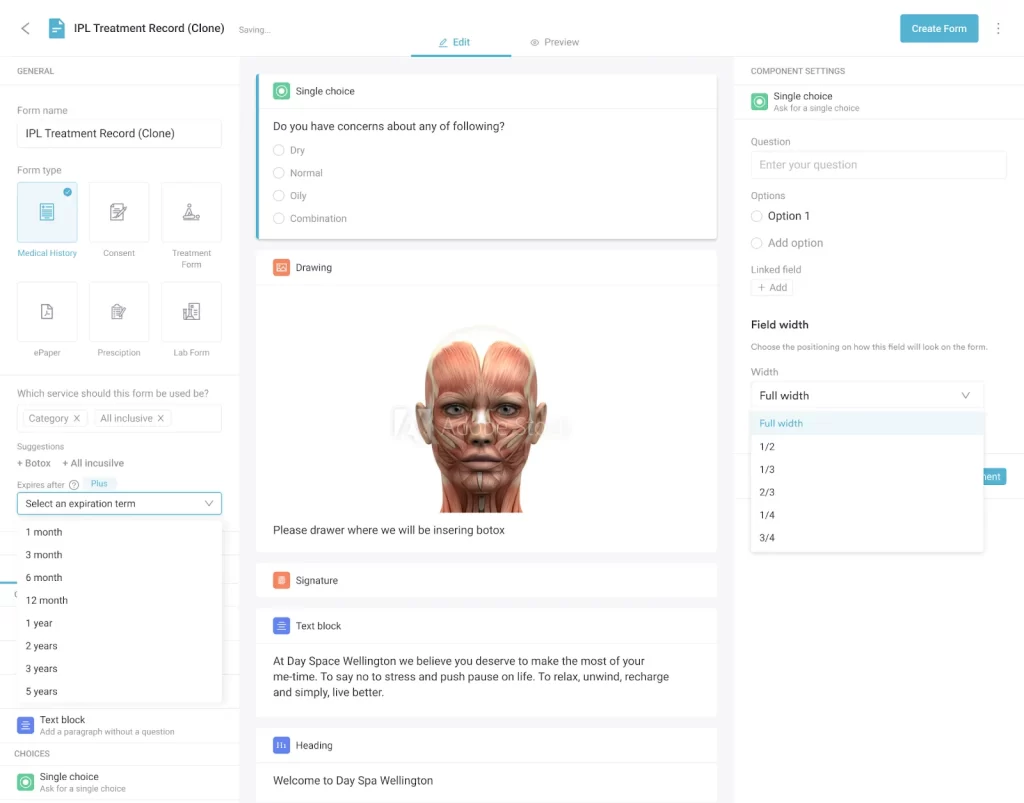
The client portal specifically addresses a common gap in smaller practices: patients leaving an appointment without a clear pathway for pre-care instructions, post-treatment guidance, or rebooking. A portal that delivers these touchpoints automatically, without requiring admin intervention, scales engagement without scaling headcount. The benefits of patient portals for smaller practices are less about data interoperability (a hospital priority) and more about reducing the communication burden on clinical staff.
Turning the Data Into Clinic Improvements
Engagement data is only useful when it connects to an operational decision. The following framework maps specific patient engagement statistics to the clinic workflows most likely to move those numbers.
- Track your no-show rate monthly. This is the most actionable engagement metric for most clinics. A no-show rate above 15% almost always indicates a gap in pre-appointment communication. Deploy automated workflows that send confirmation at booking, a reminder 48 hours before, and a same-day reminder for high-value appointments.
- Segment by engagement frequency. Identify patients who have not booked in 90+ days and run a targeted recall campaign. Use email and SMS campaigns rather than generic newsletters. Personalised subject lines referencing the patient’s last treatment type consistently outperform generic “We miss you” messages.
- Measure post-treatment return rate. For elective treatments, calculate the percentage of patients who return for a second appointment within 90 days. This is your most reliable retention indicator. If this figure drops below 40%, audit your post-treatment communication sequence for timing and relevance.
- Use digital intake forms to capture baseline data. Structured intake data gives you the raw material for personalisation. A patient who flags interest in anti-ageing treatments during intake should receive follow-up content relevant to that interest, not a generic newsletter about every service you offer.
- Survey patients after every appointment. Short post-appointment surveys with a Net Promoter Score question and one open-text field generate actionable feedback without survey fatigue. Track scores over time by practitioner and treatment type to identify specific engagement weak points.
Each of these steps produces its own engagement metric. Together, they build a feedback loop that connects patient behaviour to operational decisions rather than relying on annual satisfaction surveys that arrive too late to drive meaningful change. Pair this with robust patient scheduling and appointment management systems that give patients flexible booking options, and the structural conditions for high engagement are in place before the patient even walks through the door.
Continue your research
Want to understand what engaged patients actually experience? AI and Patient Experience covers how AI-driven tools are reshaping patient interactions and what clinics can implement today.
Looking for tools to act on your engagement data? Patient Care Management outlines the systems and workflows that translate engagement goals into clinical results.
Need to benchmark your practice performance? Med Spa KPI Guide provides a structured framework for tracking the metrics that matter most to clinic owners and practice managers.
Conclusion
The friction between patients and practices is measurable, addressable, and expensive to ignore. Patient engagement statistics consistently show that the gap between low-activation and high-activation patients maps almost directly to the presence or absence of structured outreach, digital tools, and personalised communication workflows.
Pabau’s automated recall, two-way messaging, client portal, and digital intake capabilities give practices the infrastructure to close that gap without adding administrative headcount. Whether you are tracking no-show rates, recall compliance, or post-treatment return rates, the operational levers are available. Book a demo to see how Pabau structures patient engagement across every touchpoint in your clinic’s workflow.
Frequently Asked Questions
Private clinics typically track four metrics: no-show rate (appointments missed without cancellation), post-treatment return rate (percentage of patients who rebook within 90 days), recall compliance (percentage of patients who respond to outreach), and patient satisfaction score. These are more actionable than hospital-centric measures like 30-day readmission rates, because they directly reflect the financial health of a cash-pay or elective care practice.
Digital-first engagement is the dominant trend, with practices shifting from phone-based scheduling and paper intake to automated workflows, mobile booking, and AI-assisted documentation. The growth of FHIR-enabled patient data access, the expansion of the mHealth app market toward an estimated $86 billion by 2030, and the adoption of remote patient monitoring tools are all accelerating the expectation that clinics meet patients through digital channels rather than expecting patients to call during business hours.
The Patient Activation Measure (PAM) is a validated assessment tool that scores patients 0 to 100 across four levels of engagement, from passive (relying entirely on provider guidance) to proactive (managing health independently and advocating for themselves). A 2015 study cited by the CDC found that PAM scores predicted healthcare costs and outcomes over time, making it a useful tool for identifying patients most at risk of disengaging from treatment plans before a clinical event occurs.
Research published in PMC and summarised by the CDC shows that highly activated patients have meaningfully lower readmission rates, stronger medication adherence, and better management of chronic conditions than low-activation patients. The effect is strongest in chronic disease management contexts, but engagement quality also influences outcomes in elective and aesthetic settings through treatment plan adherence, post-care compliance, and timely rebooking for maintenance treatments.
Automated appointment reminders (SMS and email) consistently show the highest return on investment for smaller clinics, reducing no-shows without requiring staff time. Two-way messaging for pre-appointment questions and digital intake forms that capture patient preferences at first contact come next. Patient portals add value when paired with proactive outreach workflows rather than deployed as standalone tools patients are expected to discover independently.










