Key Takeaways
The best clinical notes software in 2026 unifies SOAP documentation, AI scribing, and HIPAA-aligned storage with the rest of your practice workflow
Per-clinician pricing from SimplePractice, TherapyNotes, and Elation Health escalates fast for group practices with three or more providers
AI ambient scribes like Heidi Health and Upheal save 10-15 minutes per encounter but rarely replace a full EHR on their own
Pabau is the broadest option in this list, combining customizable clinical notes, AI medical scribing, telehealth, and a branded patient portal under one platform
Clinical documentation now consumes more than a third of a typical provider’s working hours, and the wrong software multiplies that burden. According to a 2024 JAMA Network Open analysis, US clinicians spend an average of 1.77 hours on the electronic health record for every hour of direct patient contact, with after-hours “pajama time” charting widely cited as a leading driver of clinician burnout. For private practice owners, the question is no longer whether to digitize notes. It is which clinical notes software actually saves time without sacrificing accuracy, compliance, or billing readiness.
This guide evaluates the best clinical notes software in 2026 across seven platforms, covering AI ambient scribing, SOAP and DAP templates, HIPAA compliance, telehealth integration, e-prescribing, and how documentation fits into the broader operational workflow. Whether you are a solo therapist hunting for a focused AI scribe or a multi-provider clinic looking for a single platform that handles documentation alongside scheduling and billing, this is a structured, criteria-based comparison. For related reading on AI SOAP notes or AI in clinical documentation, see our specialist guides.
Top 7 clinical notes software platforms compared at a glance
Seven platforms evaluated across clinical documentation features, AI capabilities, telehealth, pricing, and best-fit practice profile. Pabau is listed first as the broadest all-in-one option; the remaining six are ordered by US market presence and specialty fit.
Pabau: Best clinical notes software for multi-service clinics
Pabau is a complete practice management and clinical notes platform built for clinics that need more than a documentation-only tool. Most clinical notes software locks providers into a single specialty template library or forces them to bolt on scheduling, billing, and patient communication from separate vendors. Pabau covers documentation, AI scribing, calendar, payments, telehealth, and patient engagement in one platform.
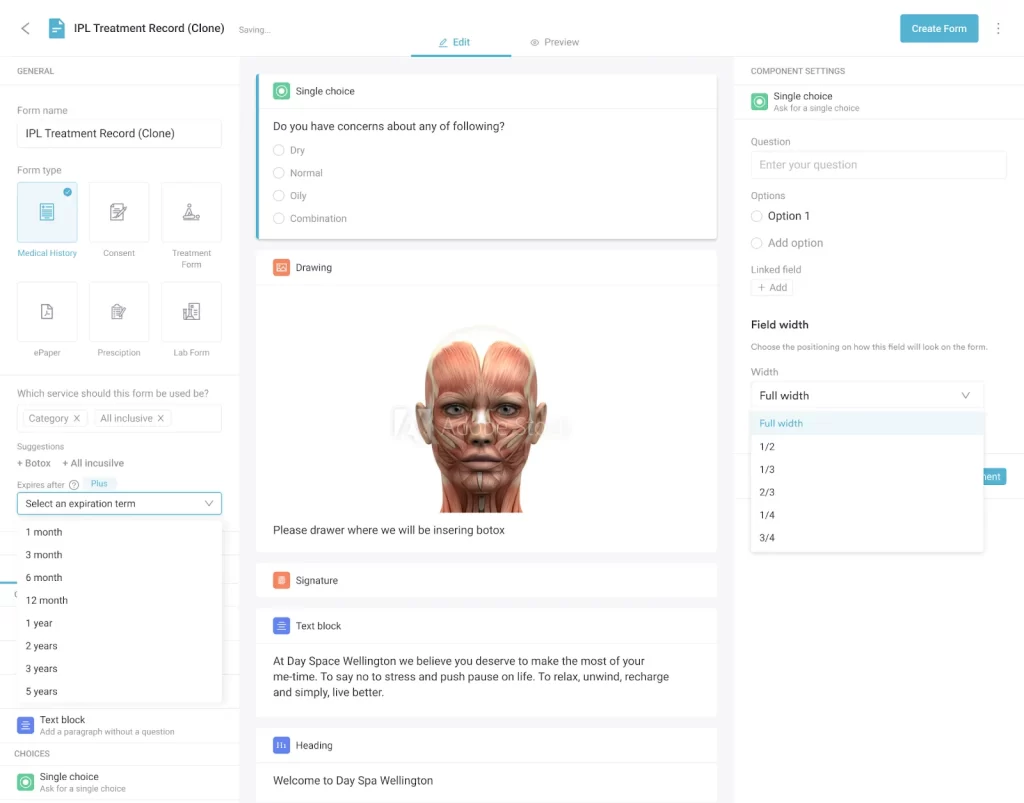
The platform supports the full patient journey: branded online booking, automated appointment reminders, HIPAA-aligned digital intake forms, video consultations, fully customizable treatment note templates, invoicing, and post-care follow-up automations. Practices running multiple providers benefit from multi-location calendars and granular permission controls, so clinicians see only the records relevant to their cases while administrators retain the full operational view. The clinical notes engine itself supports SOAP charting, DAP, BIRP, and custom layouts with image annotation, body charting, and structured data fields that feed straight into reporting.
Key features
- Customizable note templates: Build SOAP, DAP, BIRP, intake assessments, treatment plans, or bespoke clinical formats without development work
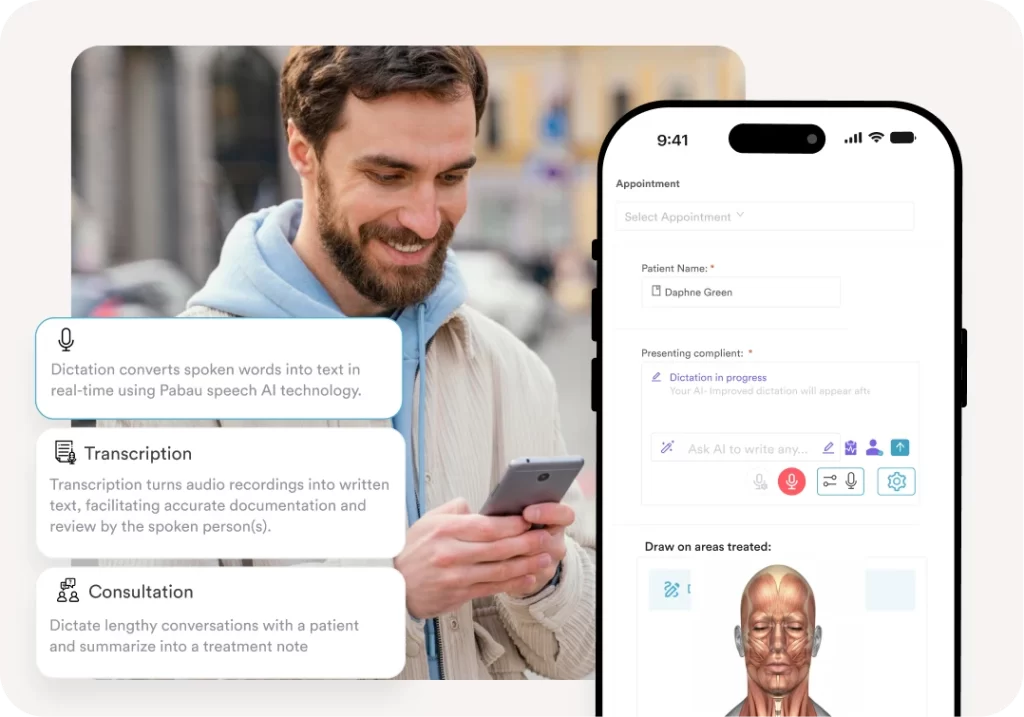
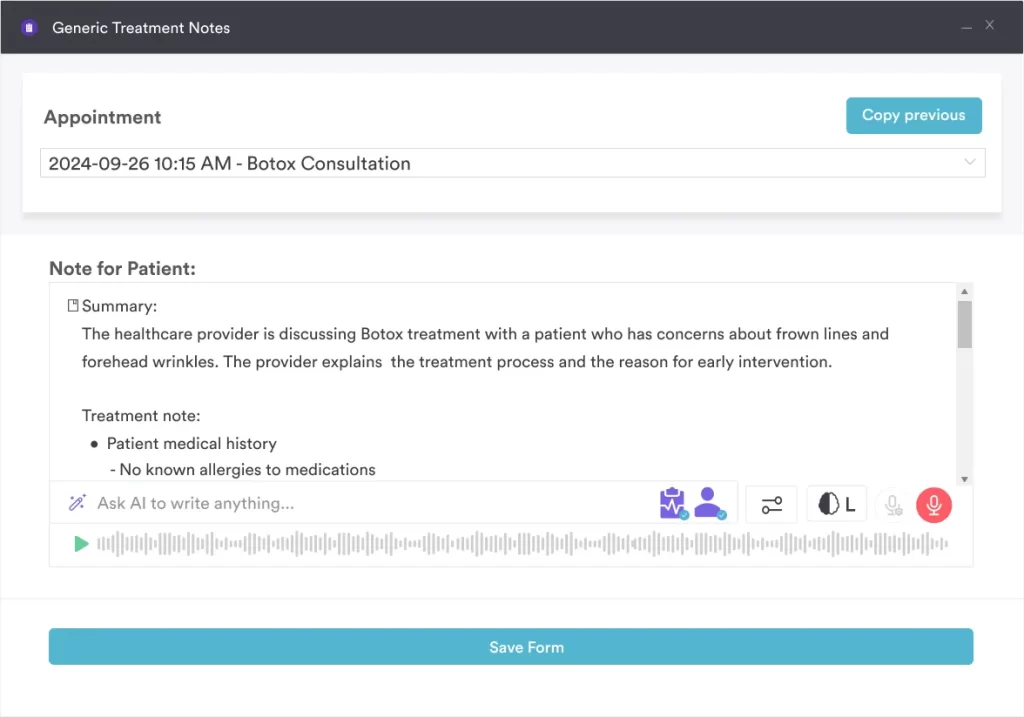
- Pabau Scribe (AI medical scribe): Ambient AI documentation that drafts clinical notes from the consultation conversation in real time
- Integrated telehealth: HIPAA-compliant video with pre and post-session forms, charting, and billing built into the call workflow
- Body charting and image annotation: Mark up clinical photography, anatomical diagrams, and injection sites directly inside the note
- Digital intake and consent forms: Sent automatically before appointments with e-signature capture and structured field mapping into the chart
- Patient portal with branding: Patients book, complete intake, sign consents, and access records under the practice’s own brand
- Automation engine: Recall reminders, follow-up sequences, post-treatment care instructions, and win-back campaigns configured without code
- Reporting and analytics: Track documentation completion, no-show rates, revenue by service, and clinician productivity from a single dashboard
Pricing
Where Pabau shines
- Operational breadth: The only platform in this comparison that covers documentation, AI scribing, scheduling, billing, marketing automation, and patient retention in one system
- Template flexibility: Customize note formats for any specialty without waiting on the vendor to build a template library for your modality
- Predictable pricing at scale: Practice-level pricing avoids the per-clinician cost spikes that hit SimplePractice, TherapyNotes, and Elation users at three or more providers
- Branded patient experience: Patients interact with your clinic’s name and logo, not a third-party software brand, across booking, forms, telehealth, and the portal
- Built-in AI scribe: Pabau Scribe is included in higher plans rather than sold as a separate $30-$40 monthly add-on
Where Pabau falls short
- Onboarding investment: The platform’s breadth means initial setup takes longer than single-purpose tools like Heidi Health or Upheal
- US insurance billing depth: ERA and EOB processing is less mature than TherapyNotes for high-volume insurance practices
- Mobile experience: Some users report the mobile app does not yet cover every workflow available on desktop
Customer reviews
According to Capterra reviewers, Pabau holds a 4.7 out of 5 rating from more than 600 verified reviews. Reviewers consistently highlight the all-in-one workflow, customizable clinical templates, and responsive support. “The customizable forms and clinical notes have saved my team hours every week and made audits painless,” one multi-location reviewer noted. The most frequently cited limitation is the initial setup curve compared with simpler, single-purpose tools.
Who Pabau is best for
- Multi-disciplinary practices combining medical, aesthetic, therapy, or allied health services under one roof
- Group practices with three or more providers where per-clinician pricing from competitors becomes expensive
- Clinics that want automated workflows for recalls, follow-ups, and patient retention layered on top of clinical documentation
- Practices that need a fully branded patient portal rather than generic third-party software
See how Pabau handles your clinical documentation workflow
Pabau combines customizable clinical notes, AI scribing, telehealth, automated reminders, and a branded patient portal in one platform. Book a personalized walkthrough for your clinic.

SimplePractice: Best for solo and small-group behavioral health
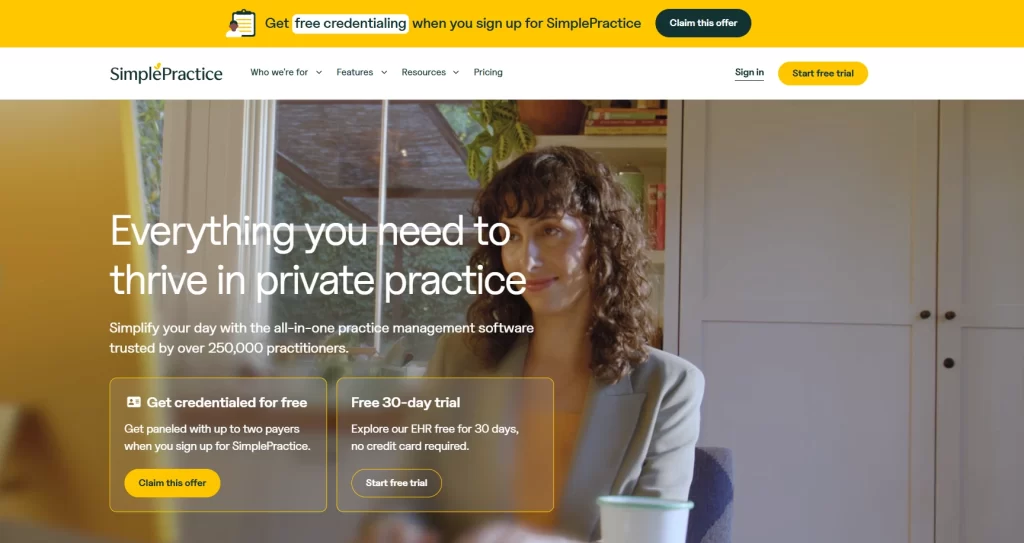
SimplePractice is the most widely used clinical notes software among US behavioral health professionals, with the vendor reporting more than 250,000 practitioners on the platform. Its reputation rests on usability: the interface is clean, the client self-scheduling widget works reliably, and the patient portal consistently scores well with both clinicians and patients. Solo therapists evaluating their first electronic chart frequently start here, and many stay long-term.
Key features
- Progress note templates: Pre-built SOAP, DAP, intake assessments, and treatment plans designed for behavioral health
- AI Notes add-on: Ambient transcription generates a structured draft for clinician review
- Integrated telehealth: HIPAA-compliant video with concurrent charting in the same interface
- Patient portal: Self-scheduling, intake forms, billing, and secure messaging
- Mobile charting: Native iOS and Android apps for documentation on the go
Pricing
Where SimplePractice shines
- Onboarding speed: Most solo clinicians are fully operational within a week, with minimal training friction
- Patient experience: The patient portal is consistently rated as one of the easiest for patients to navigate
- Telehealth integration: Built-in video is reliable and tightly tied to the chart, not a separate app
Where SimplePractice falls short
- Pricing increases: Reviewers frequently flag steep year-over-year price hikes once practices are dependent on the platform
- Insurance and claims depth: Multi-payer claims management is thinner than TherapyNotes for insurance-heavy practices
- Customization limits: Note templates are flexible within behavioral health but harder to adapt for non-mental-health specialties
Customer reviews
SimplePractice holds a 4.6 out of 5 rating from more than 2,800 verified reviews on Capterra. Positive themes center on ease of use, telehealth quality, and the patient portal. Negative themes cluster around customer support response times and recurring price increases, particularly for solo subscribers.
Who SimplePractice is best for
- Solo therapists, counselors, and small-group behavioral health practices
- Private-pay-heavy practices that do not need deep multi-payer claims processing
- Clinicians who prioritize patient experience and minimal onboarding time
TherapyNotes: Best clinical documentation software for psychotherapy
TherapyNotes is the documentation-first counterpoint to SimplePractice. Where SimplePractice optimizes for breadth and ease of use, TherapyNotes optimizes for clinical depth and billing accuracy. Its note templates are designed around psychotherapy and psychiatry workflows, and treatment plans link directly to progress notes for continuity. For practices that bill insurance heavily, the integrated claims and ERA processing is among the strongest in the category.
Key features
- Specialty templates: Psychotherapy intake, progress notes, treatment plans, and psychiatric assessments built around behavioral health workflows
- Treatment plan linkage: Goals and interventions in the treatment plan auto-populate progress notes for documentation continuity
- Insurance billing: Integrated claims submission, ERA posting, and remittance management for multi-payer practices
- E-prescribing: EPCS-ready prescribing for psychiatric medications
- TherapyFuel AI scribe: Optional ambient AI documentation as a paid add-on, around $40/month
- Integrated telehealth: HIPAA-compliant video with charting in the same window
Pricing
Where TherapyNotes shines
- Documentation quality: Templates are designed to satisfy payer audits and clinical supervision requirements
- Insurance billing: ERA, EOB, and claims scrubbing rival much more expensive enterprise platforms
- Customer support: Consistently rated near the top of the category for support response and quality
Where TherapyNotes falls short
- Single-specialty focus: Built for psychotherapy and psychiatry; not a fit for multi-disciplinary practices
- No public API: Integrations with outside systems are limited compared with cloud-native competitors
- AI scribe is a paid add-on: AI documentation is not bundled into the base plan
Customer reviews
TherapyNotes holds a 4.7 out of 5 rating from more than 950 verified reviews on Capterra. Reviewers consistently highlight documentation depth, billing accuracy, and customer support. The most common limitation cited is feature velocity: new capabilities arrive slowly compared with newer entrants like Upheal or Heidi.
Who TherapyNotes is best for
- Insurance-heavy psychotherapy and psychiatry group practices
- Clinicians who treat documentation quality and audit-readiness as non-negotiable
- Practices that need EPCS-ready e-prescribing alongside therapy notes
Heidi Health: Best AI clinical notes scribe
Heidi Health is a specialist AI ambient scribe rather than a full EHR. Clinicians open the app at the start of a consultation, and Heidi listens, transcribes, and drafts a structured note using a template the clinician selects. The output drops into whatever EHR the practice already uses. This pure-scribe positioning makes Heidi a natural fit for clinicians who like their current chart but want to cut documentation time without switching everything.

Key features
- Ambient transcription: Captures in-person and telehealth consultations, including multi-speaker scenarios
- Template library: Pre-built and custom templates for SOAP, consult letters, referrals, and specialty-specific notes
- Multilingual support: Transcription and note drafting across multiple languages
- Ask Heidi: Prompt-based queries against the consultation transcript for differential diagnoses, summaries, or follow-up planning
- Dictation mode: Hands-free note creation for clinicians who prefer post-encounter dictation
Pricing
Where Heidi Health shines
- Transcription accuracy: Strong performance even in noisy clinical environments with multiple speakers
- Template flexibility: Clinicians can build custom templates without engineering support
- Stack-on deployment: Works alongside any existing EHR rather than replacing it
Where Heidi Health falls short
- Hallucination risk on long encounters: Reviewers report occasional fabricated details in complex or extended consultations, requiring careful clinician review
- Not a complete EHR: No scheduling, billing, charting beyond notes, or patient portal
- Price step from free to paid: The jump from $0 to $150 per user per month is steep for part-time clinicians
Customer reviews
Heidi has a limited Capterra footprint and currently leans on Trustpilot reviews, where it sits around 3.8 out of 5 from roughly 465 reviews. Positive themes are time savings on documentation and template flexibility. Negative themes cluster around occasional transcription errors and price relative to AI-only competitors.
Pro Tip
AI scribes save 10-15 minutes per encounter on average, but only if the clinician trusts the output enough to skip line-by-line editing. Before committing to a paid plan, run a structured two-week trial: track how often you accept the AI draft as-is versus rewriting it. If you are rewriting more than 30 percent of notes, the platform is not yet ready for your clinical context and the time savings will not materialize.
Who Heidi Health is best for
- Clinicians who like their current EHR but want to cut documentation time
- Specialty practices needing custom note templates without vendor development support
- Multilingual clinical settings where transcription needs to handle non-English consultations
Practice Fusion: Best budget clinical notes software for primary care
Practice Fusion, now part of Veradigm, has been a familiar name in ambulatory cloud EHR since its earlier ad-supported free model. The platform has since shifted to paid tiers but remains one of the more accessible cloud EHRs for small primary-care and specialty clinics. Its strengths are the ambulatory feature set, the broad lab and pharmacy network, and a low barrier to entry compared with enterprise EHRs.
Key features
- Customizable SOAP charting: Templates configurable per specialty and provider preference
- E-prescribing: EPCS-ready prescribing with drug interaction and allergy checks
- Lab and imaging integration: Broad ordering network across major lab vendors
- ICD-10 and CPT coding: Coding tools built into the chart for billing accuracy
- Patient portal: Self-scheduling, secure messaging, and records access
Pricing
Where Practice Fusion shines
- Lab and pharmacy network: One of the broadest ordering integrations in the ambulatory cloud EHR category
- Cloud-native: No local install or server requirements; works on any modern browser
- Familiar workflow: Long-running product with documentation and training materials widely available
Where Practice Fusion falls short
- Customer support: Slow and inconsistent response times are widely cited in recent reviews
- Dated interface: UI feels older than newer cloud-native competitors
- Limited AI features: No bundled AI scribe; clinicians must layer a separate AI scribe on top
Customer reviews
Practice Fusion holds a 4.3 out of 5 rating from more than 700 verified reviews on Capterra. Positive themes are price, lab integrations, and cloud convenience. Negative themes cluster heavily around customer support response times and UI dating.
Who Practice Fusion is best for
- Independent primary-care clinics on a tight technology budget
- Small specialty practices needing strong e-prescribing without an enterprise EHR contract
- Clinicians who plan to layer a separate AI scribe on top of an existing chart
Upheal: Best AI-first clinical notes for therapists
Upheal is built for therapists who want AI to do the heavy lifting on documentation. Sessions can be recorded in person, over Upheal’s own video module, or imported from telehealth platforms. The AI produces SOAP, DAP, EMDR, or custom progress notes, plus treatment plans and session analytics, with the clinician reviewing and signing off rather than typing from scratch.
Key features
- AI progress notes: SOAP, DAP, EMDR, and other therapy-specific formats generated from session audio
- Session recording and transcription: In-person, telehealth, or uploaded audio
- Treatment plan generation: AI drafts treatment plans from initial assessments
- Session analytics: Speech patterns, sentiment, and topic frequency for clinical supervision
- HIPAA-compliant storage: Encrypted at rest and in transit, with PHIPA support for Canadian practices
Pricing
Where Upheal shines
- Therapy-specific note formats: Out-of-the-box SOAP, DAP, and EMDR templates without configuration
- Usage-based pricing: Pay-per-session pricing keeps costs predictable for part-time or variable caseloads
- Session analytics: Speech-pattern and sentiment data offer supervision insights that competitors do not provide
Where Upheal falls short
- Speaker attribution errors: Occasional misattribution between therapist and client in noisy recordings
- Not a full EHR: No scheduling, claims billing, or patient portal
- Phone-session recording on iPhone: Reviewers report inconsistent capture on iOS for phone-only sessions
Customer reviews
Upheal’s Capterra listing has a limited review footprint, but Trustpilot ratings cluster between 4.7 and 5.0 across recent feedback. Reviewers consistently call out time savings and the quality of therapy-specific note formats. Negative themes are minor: speaker attribution edge cases and iOS phone-call recording.
Who Upheal is best for
- Solo therapists who want AI documentation without committing to a full AI EHR
- Part-time clinicians who benefit from pay-per-session pricing
- Group supervisors interested in session-level analytics for training
Elation Health: Best for direct primary care and value-based practices
Elation Health is a clinical-first EHR designed around primary care rather than retrofitted from a billing platform. Its longitudinal patient view, problem-oriented charting, and care-gap reminders make it a frequent pick for direct primary care (DPC) practices and value-based care arrangements. The note interface is clean, with the patient’s full history visible alongside the active note rather than buried under tabs.
Key features
- Longitudinal patient view: Full clinical history visible alongside the active note
- Problem-oriented charting: Notes structured around active problems rather than visit-by-visit
- E-prescribing with EPCS: Controlled-substance prescribing built in
- Lab and imaging integration: Direct ordering and result inbox
- Note Assist AI: AI-assisted documentation drafting
- Care-gap reminders: Quality measure tracking for value-based contracts
Pricing
Elation Health does not publish pricing on its website. Third-party review aggregators place Direct Care plans around $275 per provider per month (annual) and insurance-billing plans in the $333-$399 per provider per month range. Confirm directly with Elation before signing.
Where Elation Health shines
- Clinical-first design: Built for clinicians who want the chart to feel like a chart, not a billing system
- Direct primary care workflows: Strong fit for membership-based and DPC practices
- Longitudinal view: Patient history is genuinely visible during the encounter
Where Elation Health falls short
- Billing learning curve: The billing module has a steeper onboarding than the clinical side
- Higher price point: One of the more expensive options in this list per provider
- Limited multi-specialty fit: Optimized for primary care; less suited to aesthetic, therapy, or allied health
Customer reviews
Elation Health has a small Capterra footprint relative to its market presence. Third-party aggregator ratings sit around 4.4 out of 5 from a modest sample. Reviewers praise the clinical interface and longitudinal view; the most common criticism is the billing module’s learning curve.
Who Elation Health is best for
- Direct primary care, concierge medicine, and membership-based practices
- Independent primary care groups in value-based or risk-bearing arrangements
- Clinicians who want a problem-oriented chart rather than visit-oriented charting
How to choose clinical notes software for your clinic
No single platform wins for every practice. The right clinical notes software depends on specialty, payer mix, practice size, and whether documentation is a standalone need or part of a broader operational stack. Six criteria separate a productive long-term platform from a costly mistake, and weighing them against your specific situation is more useful than chasing the highest-rated option on a single review site.
Where most evaluations go wrong: teams demo each platform in isolation and grade it on note-taking alone, then discover six months later that the scheduling, billing, or patient communication around the note is what actually consumes their time. Documentation accounts for roughly 30 to 40 percent of administrative workload in a typical private practice. The other 60 to 70 percent comes from coordination tasks that live outside the note. If your shortlist mixes notes-only tools with full-stack platforms, score them on the full EMR feature set, not just the documentation interface.
Practices combining therapy with aesthetics, physiotherapy, or allied health services hit this wall earliest because no single-specialty tool maps cleanly onto a multi-service operation. Pabau remains the only platform in this comparison with customizable clinical notes, AI scribing, telehealth, digital intake forms, and a branded patient portal under one roof, which is why it leads this list for multi-service clinics rather than single-modality solos.
Expert picks
Continue your research
Comparing AI scribes against full EHRs? AI SOAP notes explains how AI-generated documentation compares with manual SOAP charting across accuracy, time savings, and clinical risk.
Looking at AI documentation specifically for medical practice? Clinical notes AI covers how ambient scribes integrate into existing clinical workflows and where they fall short.
Running a mental health or therapy practice? Best EHR for therapists compares the seven leading platforms for solo and group behavioral health practices.
Evaluating HIPAA-compliant telehealth alongside your notes? HIPAA-compliant telehealth covers what to verify with any video platform before signing a Business Associate Agreement.
Conclusion
Choosing the best clinical notes software in 2026 is less about picking the highest-rated platform and more about matching documentation capability to practice reality. Behavioral health solos will struggle to beat SimplePractice on ease of use. Insurance-heavy psychotherapy groups will find TherapyNotes hard to dislodge on billing depth. Clinicians who like their existing chart but want AI on top should look at Heidi Health or Upheal. Direct primary care practices align well with Elation Health’s clinical-first design.
For multi-service clinics, group practices, and any operation where documentation is one part of a broader workflow, Pabau remains the most complete option in this comparison. Customizable notes, built-in AI scribing, integrated telehealth, a branded patient portal, automated recall workflows, and multi-provider scheduling sit under one platform without per-clinician cost escalation at scale. Book a demo to see how Pabau handles your specific documentation and operational workflow.
Frequently Asked Questions
For solo behavioral health practices, SimplePractice is the most widely used option due to its ease of use and patient portal quality. For insurance-heavy psychotherapy groups, TherapyNotes offers stronger documentation and billing workflows. For multi-service or multi-provider clinics, Pabau provides the broadest operational platform combining clinical notes, AI scribing, scheduling, billing, and patient communication. The best choice depends on specialty, practice size, and whether documentation is your only need or part of a wider operational stack.
Prioritize a signed HIPAA Business Associate Agreement, customizable note templates that fit your modality, AI scribing or fast structured charting, integrated telehealth with concurrent documentation, audit-ready records with full version history, role-based access controls, and predictable pricing that does not balloon as you add providers. Verify each feature works in a structured demo using your real clinical workflow, not the vendor’s scripted scenario.
Pricing varies significantly by category. AI-only scribes like Upheal start free with paid plans from $1 per session capped around $69 per month, while Heidi Health Pro runs $150 per user per month. Therapy-focused EHRs like SimplePractice and TherapyNotes start around $49-$69 per provider per month. Primary care EHRs like Practice Fusion start around $149 per provider per month. Pabau starts from $65 per month at the practice level rather than per clinician, which is often better value for groups with three or more providers. Always verify current pricing directly with vendors.
AI clinical notes can be HIPAA compliant when the vendor signs a Business Associate Agreement, encrypts data at rest and in transit, maintains audit logs, supports access controls, and trains staff on minimum-necessary use. Compliance is a vendor configuration question, not an inherent property of AI. Before adopting any AI scribe, request the BAA, confirm data is not used to train external models without explicit consent, and verify how long recordings are retained. The HHS Office for Civil Rights treats vendors handling PHI as Business Associates regardless of whether AI is involved.
An AI scribe is a documentation-only tool that listens to a consultation and drafts a structured note. It does not handle scheduling, billing, patient communication, or chart history. Clinical notes software in the broader sense is the full electronic chart, often part of an EHR or practice management platform, that stores, retrieves, and secures the patient record over time. Many practices use both: the EHR is the system of record, and the AI scribe drafts notes that get reviewed and saved into it. Pabau combines both layers in one platform; Heidi Health and Upheal are scribe-only and require an EHR underneath.
Free clinical notes software exists but rarely supports a fully compliant private practice on its own. Free tiers from Heidi Health or Upheal cover individual AI scribing with limits, and Practice Fusion historically offered a free ad-supported EHR before moving to paid tiers. For most private practices, the realistic minimum is a paid plan that includes a signed Business Associate Agreement, audit logs, role-based access controls, and structured backups. Free tools work for trialing AI documentation but are usually not adequate as a long-term system of record.










