Key Takeaways
How to start a private therapy practice requires a valid state license, a chosen business entity (LLC or PLLC), and malpractice insurance before seeing your first client.
Insurance credentialing can take 3-6 months depending on the payer and state – start this process before you open your doors.
Most solo therapy practices spend $5,000-$15,000 in startup costs covering licensing, office setup, software, and marketing.
Pabau’s all-in-one platform handles scheduling, digital intake forms, clinical notes, billing, and telehealth in one place, eliminating the need for multiple tools when launching.
Most therapists finishing their training assume the hardest part is behind them. It isn’t. Starting a private practice involves a separate skillset that clinical training rarely covers: business registration, malpractice insurance, payer credentialing, marketing, and operational technology. According to the American Counseling Association, many clinicians launch private practices while still employed elsewhere, building caseloads gradually before making the full transition. That incremental approach reduces financial risk significantly.
This guide is written for licensed mental health professionals: LCSWs, LPCs, LMFTs, licensed psychologists, and PMHNPs who are ready to move from employment to independent practice. It covers every major workstream, from legal structure through technology selection, in the order you’ll encounter them. For a broader view of what makes private practice worthwhile, see benefits of private practice before diving into the operational steps below.
How to Start a Private Therapy Practice: Legal Foundation First
Before you schedule your first client, three legal requirements must be in place: an active license in your state, a registered business entity, and professional liability insurance. Skipping any one of these exposes you to regulatory action and personal financial liability.
Choosing Your Business Structure
Most new private practitioners choose between a sole proprietorship, an LLC, or a PLLC. Sole proprietorships require no state filing and are the simplest option, but they offer no liability protection. An LLC separates personal assets from business liabilities and is the most common choice for solo practitioners. However, not all states permit licensed therapists to form a standard LLC. Some require a PLLC (Professional Limited Liability Company), which is specifically designed for licensed professionals. Check with your state licensing board and a local attorney before filing. For a detailed look at the ongoing operational considerations of each structure, private practice management frameworks differ significantly between entity types.
| Structure | Liability Protection | State Filing Required | Best For |
|---|---|---|---|
| Sole Proprietorship | None | No | Testing the waters part-time |
| LLC | Yes (personal assets protected) | Yes | Solo practitioners in most states |
| PLLC | Yes (required for licensed professionals in some states) | Yes | States that restrict LLC formation for therapists |
Licensing and Malpractice Insurance
Your license must be in good standing and active in the state where you’re practicing. For telehealth, this often means holding licenses in every state where your clients are physically located during sessions, though interstate compacts are gradually expanding portability. Malpractice insurance (professional liability insurance) is non-negotiable. Occurrence-based policies are generally preferable to claims-made policies for long-term protection, though they cost more. Professional associations like the National Association of Social Workers (NASW) offer member-rate malpractice insurance that can reduce costs substantially for new practitioners.
Building Your Business Plan and Financial Model
A therapy practice is a business. Treating it otherwise is the most common reason new practices fail within the first two years. Your business plan doesn’t need to be 40 pages, but it does need to answer four financial questions before you open.
- What are your startup costs? Most solo practices spend $5,000-$15,000 before seeing their first client. This covers state filing fees ($50-$500), malpractice insurance ($500-$2,000/year), office rent or telehealth setup, EHR software, website, and directory listings.
- What is your break-even caseload? Divide your fixed monthly costs by your session fee. A therapist with $3,000/month in costs charging $150/session needs 20 clients per month to break even.
- Will you accept insurance? Insurance panels increase referral volume but reduce per-session revenue by 30-50% compared to private pay rates.
- What is your 90-day cash flow projection? Insurance reimbursements lag 30-90 days after claim submission. Plan for that gap.
For a structured approach to building out these financial projections, medical practice business planning frameworks apply directly to therapy practices and can save significant setup time. The IRS self-employment tax guidance is also essential reading before you finalize your financial model, as quarterly estimated tax payments will affect your cash flow projections significantly.
Pro Tip
Track startup costs from day one in a dedicated business account, separate from personal finances. This simplifies tax preparation, protects your liability shield, and gives you accurate data on your actual break-even timeline. Open a business checking account before you spend your first dollar on the practice.
Insurance Credentialing: The Step Most Therapists Underestimate
Credentialing with insurance panels is the single longest lead-time task when launching a private practice. The process typically takes 3-6 months depending on the payer and state, though community reports from practitioners suggest it can extend longer in some regions. Starting this process late is the most common operational mistake new private practitioners make.
How Credentialing Works
Each insurance company requires you to submit an application demonstrating your license, education, malpractice coverage, and clinical training. The payer verifies your credentials through a primary source verification process, then reviews whether they have capacity on their panel (some panels are closed to new providers). Once approved, you sign a participation agreement that specifies your contracted reimbursement rates.
Medicare credentialing follows its own process through CMS’s PECOS system. LCSWs and psychologists have long been eligible Medicare providers, and as of January 1, 2024, LMFTs and LPCs (designated as Mental Health Counselors by CMS) became independently eligible to enroll and bill Medicare as well, reimbursed at 75% of the psychologist rate for the same CPT codes. Each license type has specific eligibility and enrollment requirements that differ from commercial payer rules – review the CMS provider enrollment guidance for your license type before applying.
Private Pay vs. Insurance Panel Strategy
Many new therapists credential with 3-5 major payers to build volume quickly, then transition higher-income clients to private pay over time. Others start entirely private pay, using sliding-scale fees to maintain accessibility. Both strategies work. The determining factor is usually your local market: areas with lower median incomes typically require insurance acceptance to maintain a sustainable caseload, while urban markets often support private-pay-only practices. Claims management software that tracks submission status, denial rates, and reimbursement lag is worth evaluating before you credential with any payer.
Setting Up Your Technology Stack
Solo practitioners who try to run a practice on spreadsheets, email, and a separate video platform typically spend 8-12 hours per week on administrative tasks that integrated software handles in 1-2 hours. Technology decisions made at launch are hard to reverse, so choosing the right foundation matters.
What Your Practice Management Software Must Cover
At minimum, your software platform needs to handle five workflows from day one: scheduling, clinical documentation (SOAP notes), billing and superbills, client communication, and HIPAA-compliant file storage. Practices that add telehealth, intake forms, and automated reminders to that stack from day one see significantly lower no-show rates and faster client onboarding.
- Scheduling: Online booking with automated appointment reminders reduces no-shows. Clients who self-schedule are more likely to keep their appointments.
- Clinical notes: Structured SOAP note templates speed documentation and support audit defense. AI-assisted note generation is an emerging option worth evaluating.
- Billing: Superbill generation for private-pay clients and direct insurance claim submission for paneled practices. Look for built-in ERA/EOB reconciliation.
- Client portal: Secure messaging, document sharing, and appointment self-management reduce administrative back-and-forth.
- Telehealth: Integrated video that does not require a separate HIPAA BAA with a third-party vendor simplifies compliance significantly.
For a comprehensive evaluation of what to look for, EHR for private practice options vary considerably in how well they handle the billing and documentation workflow combination. Therapy practice management software that consolidates these into one platform eliminates the integration complexity and BAA management that comes with multi-vendor stacks.
Pabau’s platform covers all five of these workflows natively: scheduling with online booking, structured clinical notes, claims management, a client portal for secure communication and document exchange, and integrated telehealth with video consultations. For solo practitioners launching without an IT team, that consolidation matters more than any individual feature.
See How Pabau Runs Your Entire Practice
From scheduling and clinical notes to telehealth and billing, Pabau handles every workflow a solo therapy practice needs. Book a demo to see it running with your specialty in mind.

HIPAA Compliance and Data Privacy
HIPAA compliance is not optional for any US-based mental health practice. Every piece of technology that touches protected health information (PHI) – your EHR, email system, video platform, and even your scheduling tool – requires a signed Business Associate Agreement (BAA) from the vendor. A missing BAA is a HIPAA violation even if no data breach occurs.
For solo practitioners, the four highest-risk areas are unsecured messaging (never use personal Gmail or SMS for clinical communication), unencrypted file storage, telehealth platforms without a BAA, and intake forms collected via unencrypted web forms. A detailed checklist of what to verify appears in HIPAA compliance for clinic software, which covers BAA requirements and technical safeguard obligations for small practices. The HHS HIPAA guidance for healthcare professionals is the authoritative reference for understanding your obligations as a covered entity.
Client Onboarding and the First 30 Days of Practice
Your intake workflow determines the quality of first impressions and the efficiency of your documentation from session one. Practices that send intake paperwork digitally before the first appointment arrive with completed consent forms, intake histories, and insurance information already on file. That eliminates 15-20 minutes of administrative setup per new client.
What Your Intake Process Should Cover
A complete intake packet for a mental health practice typically includes: a consent to treatment form, a HIPAA notice of privacy practices, a financial policy (covering fees, cancellation policy, and insurance billing), a biopsychosocial intake questionnaire, and emergency contact and safety planning information. Using digital intake forms that sync directly to the client record eliminates transcription errors and reduces paper storage requirements entirely.
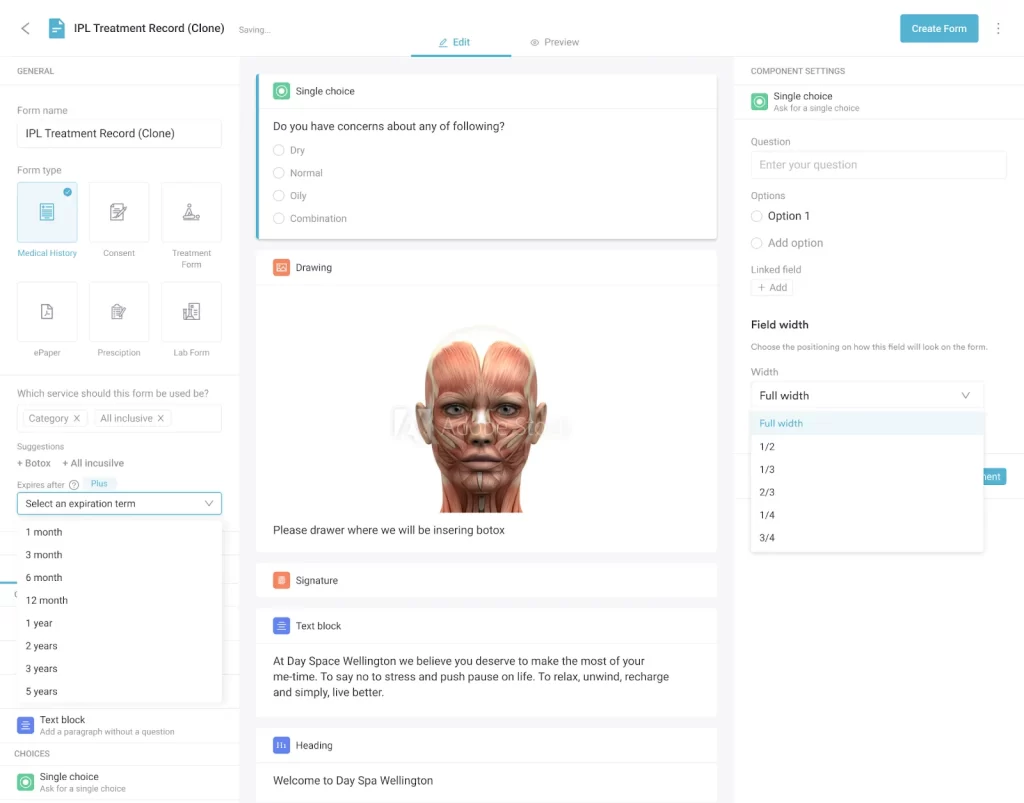
In your first 30 days, focus on three things: getting your first 5-10 clients, testing your billing workflow end-to-end, and refining your session documentation so it takes no more than 10-15 minutes per session. Everything else – marketing, referral networks, specialty positioning – can be built out over the following 90 days.
Marketing Your Practice and How to Find Your First Clients
New practitioners consistently overestimate how quickly organic marketing produces clients and underestimate how effectively a single strong referral source can fill a caseload. Your first 10-15 clients will almost certainly come from direct referrals, directory listings, or former colleagues rather than from social media or Google search.
Where to Start
- Therapist directories: Psychology Today, Therapy Den, and Zencare are the highest-traffic options. Psychology Today’s listing cost and trial availability vary by region – verify current pricing directly before listing.
- Referral relationships: Psychiatrists, PCPs, and employee assistance programs (EAPs) generate reliable, recurring referrals. One strong referral relationship can provide 3-5 new clients per month consistently.
- Professional networks: Your state association, previous supervisors, and clinical training sites are underutilized referral sources. Most new practitioners don’t ask systematically.
- Niche positioning: Therapists who specialize in a specific population (perinatal mental health, first responders, LGBTQ+ affirmative therapy) typically fill their caseloads faster than generalists in competitive markets.
A practice website with a clear specialty statement, your licensure and credentials, and a direct online booking link converts directory traffic into scheduled appointments. Without it, potential clients who find your directory listing have no obvious next step. Connecting online booking directly to your scheduling software closes that gap automatically.
Pro Tip
Reach out to three psychiatrists in your area within your first month of opening. Offer a brief 15-minute call to introduce your specialization and the client populations you work best with. Psychiatrists consistently need trusted therapists for medication-plus-therapy referrals and will send clients your way when they know your clinical approach.
Managing Caseload, Avoiding Burnout, and Running a Sustainable Practice
Private practice removes the structural boundaries that employment provides: set hours, administrative support, and peer contact. Without intentional design, the administrative burden of running a solo practice compounds clinical work in ways that drive burnout faster than agency employment. New private practitioners consistently underestimate this workload in their first year.
A full-time solo practice typically means 20-25 billable sessions per week, not 40. The remaining hours go to documentation, billing follow-up, marketing, professional development, and business administration. Practitioners who try to maintain 35+ clinical hours quickly discover the documentation backlog alone creates unsustainable stress. For evidence on how administrative burden contributes to clinician burnout, burnout in healthcare research consistently identifies documentation time as the highest-impact reducible variable.
Build sustainability into your structure from the start: set a hard cap on clinical hours, protect dedicated documentation time in your schedule, and use automation to handle reminders, recalls, and billing follow-up rather than doing it manually. Starting a medical practice with the right operational infrastructure is significantly easier than retrofitting it after you’re already overwhelmed.
Continue your research
Need a clinical documentation framework for your new practice? SOAP Notes for Social Work provides a step-by-step guide to writing efficient, defensible clinical notes across therapy modalities.
Want guidance on preventing practitioner burnout as you grow? Therapist Burnout: Signs, Causes, and Prevention covers the specific risk factors for solo practitioners and practical structural interventions.
Looking for intake and consent form templates to use from day one? Group Therapy Informed Consent covers the consent elements required for compliant therapy intake documentation.
Conclusion
The biggest challenge in starting a private therapy practice isn’t clinical competence. It’s the operational infrastructure: legal setup, credentialing timelines, HIPAA compliance, billing workflows, and client acquisition all running in parallel during the same 3-6 month launch window. Practitioners who build this infrastructure systematically arrive at their first clients with sustainable systems already in place.
Pabau’s therapy practice management platform handles scheduling, digital intake forms, clinical notes, billing, client portal, and telehealth in one place, removing the multi-vendor complexity that drains administrative time in a solo practice. To see how it runs with your workflow, book a demo and walk through the platform with your specific specialty and practice structure in mind.
Frequently Asked Questions
Register your business entity (LLC or PLLC) through your state’s Secretary of State office. Filing fees range from $50 to $500 depending on the state. Your financial plan should include startup cost projections, a break-even caseload calculation based on your session fee, and a 90-day cash flow forecast that accounts for insurance reimbursement lag of 30-90 days after claim submission.
You need an active, unrestricted license in your state for your credential type: LCSW, LPC, LMFT, licensed psychologist, or PMHNP. Most licensure paths require a master’s degree or higher plus supervised clinical hours, though psychologists typically require a doctoral degree. For telehealth across state lines, check whether your states participate in an interstate licensure compact before seeing out-of-state clients.
Submit a credentialing application directly to each payer’s provider relations department, or use a credentialing service to manage multiple applications simultaneously. You’ll need your license, NPI number, malpractice insurance certificate, educational history, and clinical training documentation. Start the process 4-6 months before your intended opening date. Some panels are closed to new providers – have a private-pay rate ready as a fallback while credentialing is pending.
Telehealth-only practices typically cost $3,000-$8,000 to launch, covering licensing fees, malpractice insurance, EHR software, and directory listings. In-person practices add office rent deposits, furniture, and build-out costs that typically bring startup costs to $8,000-$20,000. Ongoing monthly overhead for a solo practice generally runs $1,500-$4,000 depending on office location, software stack, and whether you carry employees.
List on 2-3 therapist directories (Psychology Today, Therapy Den, Zencare) and contact psychiatrists, PCPs, and EAPs in your area directly within your first month. Niche specialization significantly accelerates caseload growth in competitive markets. A simple website with online booking converts directory referrals more effectively than directories alone. Most new practitioners reach a sustainable caseload of 15-20 weekly clients within 6-12 months using these channels.