Key Takeaways
Patient experience covers every interaction a patient has with a healthcare provider, from booking to billing to follow-up.
It differs from patient satisfaction: experience measures what actually happened; satisfaction measures whether expectations were met.
Poor patient experience is linked to lower treatment adherence, higher readmission rates, and reduced practice revenue.
Pabau’s automated workflows, digital forms, and recall tools help clinics systematically improve experience at every touchpoint.
Clinics losing patients to competitors rarely lose them over clinical outcomes. They lose them over wait times, confusing intake paperwork, unanswered calls, and follow-ups that never arrive. What is patient experience in healthcare? It is the full accumulation of those moments, and how a practice manages them determines whether patients return, refer others, and comply with treatment plans. This guide covers what patient experience means, how it differs from satisfaction, how to measure it in a clinic setting, and what practical steps drive meaningful improvement.
What Is Patient Experience in Healthcare?
According to the Agency for Healthcare Research and Quality (AHRQ), patient experience encompasses the range of interactions that patients have with the healthcare system, including care from health plans, doctors, nurses, and staff in hospitals, physician practices, and other healthcare facilities. The Beryl Institute, the leading independent body advancing this field, defines it as “the sum of all interactions, shaped by an organisation’s culture, that influence patient perceptions across the continuum of care.”
That second definition is operationally useful for clinic owners. It surfaces two things most definitions miss: culture shapes experience before any single interaction happens, and the continuum matters as much as any individual moment.
- Pre-visit: ease of booking, appointment confirmation messages, intake form completion
- During visit: wait times, staff communication, clinical environment, clarity of explanation
- Post-visit: aftercare instructions, billing clarity, follow-up communications, recall scheduling
For private practices and aesthetic or wellness clinics, this framework matters especially. Hospital-focused definitions often reduce patient experience to inpatient stay metrics. In outpatient and elective settings, the pre-visit and post-visit phases carry more relative weight because patients choose freely whether to return. Investing in patient experience management starts with mapping where these interactions occur and who owns each one.
The Society of Hospital Medicine defines it as “everything we say and do that affects our patients’ thoughts, feelings and well-being.” For clinic teams, that is a useful daily operating principle: every communication, every process delay, every unexplained fee shapes what patients carry away from their visit.
The Role of Digital Intake Forms at the First Touchpoint
The intake process is often a patient’s first substantive interaction with a clinic. Paper forms in a waiting room signal disorganization. A digital form sent 48 hours before the appointment signals preparation and respect for the patient’s time. Clinics using digital intake forms routinely report shorter wait times and better-prepared consultations because clinical staff have reviewed relevant history before the patient arrives.
Patient Experience vs. Patient Satisfaction
These two terms are used interchangeably in most clinic conversations. They measure different things, and conflating them produces misleading performance data.
| Dimension | Patient Experience | Patient Satisfaction |
|---|---|---|
| What it measures | What actually happened during care interactions | Whether expectations were met |
| Example question | “Did staff explain your medication clearly?” | “Were you satisfied with your visit today?” |
| Bias risk | Lower – anchored to observable events | Higher – shaped by prior expectations |
| Actionability | High – identifies specific process gaps | Medium – tells you the outcome, not the cause |
| Survey instrument | CAHPS, HCAHPS | NPS, custom satisfaction scales |
A patient with very low expectations who receives mediocre care may report high satisfaction. A patient who expected prompt communication and had to wait three days for results may report low satisfaction despite receiving clinically excellent care. Neither response tells the clinic what actually went wrong. Measuring patient satisfaction remains useful for tracking overall sentiment, but it needs experience data alongside it to be actionable.
The CAHPS (Consumer Assessment of Healthcare Providers and Systems) framework, developed by the AHRQ, was specifically designed to standardize experience measurement. Its questions ask about concrete events: whether care was explained, whether staff were respectful, whether appointments started on time. These observable benchmarks are far more useful for operational improvement than generic satisfaction scores.
Why Patient Experience Matters for Health Outcomes
Johns Hopkins Medicine states that a positive patient and family experience while in hospital often results in better overall health outcomes. Clear communication from healthcare providers helps patients and families understand how to manage their health and lowers the likelihood of hospital readmission. The causal mechanism is straightforward: patients who understand their care instructions follow them. Patients who feel heard by their clinicians report concerns earlier.
For clinic operators, the business case runs parallel to the clinical one:
- Retention: Patients who report positive experiences are more likely to return for follow-up treatments and refer family members.
- Compliance: Effective patient communication improves adherence to treatment protocols, reducing complication rates and associated liability.
- Reviews: Online review platforms amplify experience signals. A pattern of negative experiences around wait times or billing confusion accumulates publicly.
- CMS reimbursement (US): Under the Hospital Value-Based Purchasing program, HCAHPS scores affect Medicare payment adjustments. For hospital-adjacent practices, experience scores carry financial weight.
Cleveland Clinic was the first major academic medical center to appoint a Chief Experience Officer and establish a formal Office of Patient Experience, recognizing that experience management requires dedicated operational ownership, not just a survey sent at discharge. Private practices operating without dedicated resources need systems that make experience improvement structural rather than aspirational. That is where patient care management infrastructure becomes the practical substitute for headcount.
Pro Tip
Review your last 25 patient journey touchpoints. Identify which three generated the most friction (missed communications, long waits, unclear billing). Fix those three before adding new experience initiatives. Concentrated improvements outperform broad but shallow changes.
How Patient Experience Is Measured
Measurement frameworks vary by setting, country, and practice size. These are the instruments and methods most relevant to clinic operators:
HCAHPS and CAHPS Surveys
The HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems) survey is the standardized CMS instrument for measuring patients’ perceptions of hospital experience. It covers communication with doctors and nurses, responsiveness of staff, pain management, discharge information, and overall hospital rating. CMS publishes HCAHPS results publicly, creating direct reputational and financial accountability.
CAHPS surveys extend the same methodology to outpatient, dental, surgical, and other settings. The AHRQ administers the CAHPS program and provides validated survey instruments that can be adapted for private practice use. For clinics not subject to mandatory reporting, adopting CAHPS-style questions produces more actionable data than generic five-star reviews because the questions are standardized and comparable across settings.
Net Promoter Score (NPS)
NPS asks one question: “How likely are you to recommend this clinic to a friend or colleague?” Scores range from 0-10. Promoters (9-10), Passives (7-8), and Detractors (0-6) calculate a net score. NPS is fast to deploy and benchmarkable across industries, but it captures overall sentiment rather than specific process failures. Use it as a directional indicator alongside more granular feedback mechanisms, not as a standalone measure.
Post-Visit Feedback and Review Platforms
Automated post-visit surveys sent within 24 hours of an appointment capture experience data at peak recall. Response rates drop significantly beyond 48 hours. Clinics using systematic feedback capture combined with review management tools can route positive feedback to public platforms while flagging negative responses for internal resolution before they appear as public reviews.
How to Improve Patient Experience Across Every Touchpoint
Most clinics treat the concept in the abstract. Improvement becomes concrete when mapped to specific workflow decisions. Here are five touchpoints where operational changes produce measurable gains.
1. Booking and Pre-Visit Communication
Friction at booking predicts cancellation rates. Online booking that requires patients to call during business hours loses to competitors with 24/7 self-scheduling. Appointment confirmation messages, pre-visit preparation instructions, and digital intake forms sent in advance reduce anxiety and no-shows simultaneously. Appointment scheduling workflows that include automated confirmation and reminder sequences handle this without manual staff effort.
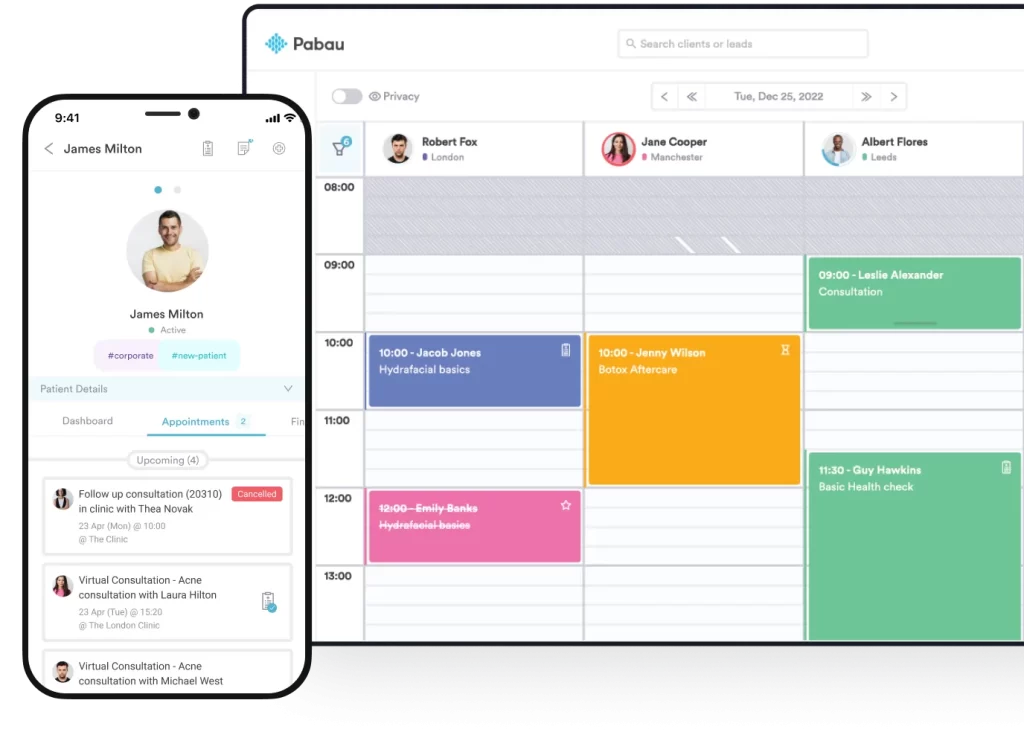
2. In-Clinic Environment and Staff Communication
Wait time perception is partly psychological. Patients who receive an explanation for delays report lower frustration than those who wait in silence for the same duration. Staff who acknowledge patients by name, explain what is happening, and check understanding after clinical explanations are the primary drivers of positive experience ratings. Training protocols matter here as much as any technology investment.
See How Pabau Manages the Full Patient Journey
From digital intake forms and automated reminders to post-visit follow-up and review capture, Pabau handles every patient experience touchpoint in one platform. Book a demo to see it in action.

3. Post-Visit Follow-Up and Recall
The post-visit phase is where most clinics lose ground. A patient who receives clear aftercare instructions, a follow-up check-in message, and a timely recall reminder for their next treatment feels managed, not forgotten. Pre- and post-care communications sent automatically through practice management software ensure consistency without adding staff workload. Patients who receive systematic follow-up are measurably more likely to rebook.
4. Automating Routine Experience Touchpoints
Manual processes create inconsistency. When a staff member forgets to send a recall message or a post-visit survey, the patient’s experience degrades silently. Automated workflows replace manual decisions with triggered sequences: a confirmation fires at booking, a reminder fires 48 hours before, aftercare fires same-day, a satisfaction survey fires 24 hours post-visit. Each automation reduces both workload and the variance that erodes experience quality.
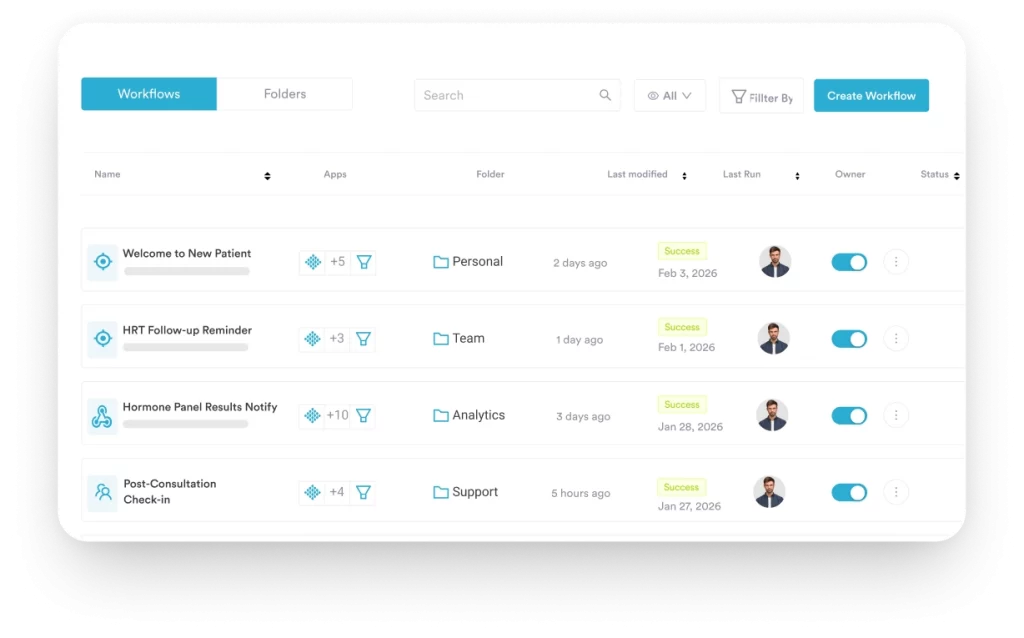
Patient engagement strategies built on automation work because consistency is itself an experience signal. A patient who receives exactly the right communication at exactly the right time perceives their provider as organized, attentive, and professional, regardless of whether a human or a system sent the message.
5. Billing Transparency
Surprise billing is among the most reliable drivers of negative experience reviews. Patients who receive a clear fee explanation before treatment, an itemized invoice, and flexible payment options report higher experience scores even when the actual cost is higher than they hoped. Billing transparency is a communication problem, not just a finance problem.
Consider what AI tools for patient experience can do at the billing stage: automated pre-treatment cost summaries, digital consent forms that include fee acknowledgments, and post-visit invoice delivery remove the uncertainty that generates complaints.
Expert Picks
Want a framework for capturing patient feedback systematically? How to Capture Patient Feedback covers the tools, timing, and question frameworks that generate actionable data from clinic patients.
Looking to strengthen patient retention through better engagement? Improve Patient Engagement outlines specific communication sequences and touchpoint strategies for private clinics.
Need to understand how scheduling affects patient experience? Patient Scheduling and Appointment Management explores how booking workflows shape first impressions and no-show rates.
Conclusion
Patient experience in healthcare is not a sentiment survey. It is the operational outcome of every system, process, and communication decision a clinic makes. Practices that treat it as a structural concern rather than an occasional measure see higher retention, better treatment compliance, and stronger referral rates.
Pabau’s automated workflow tools give clinics the infrastructure to deliver consistent, high-quality experience at every touchpoint without adding headcount. To see how Pabau handles the full patient journey from booking to post-visit follow-up, book a demo.
Frequently Asked Questions
Patient experience measures what actually happened during care interactions – whether a nurse explained medication clearly, whether wait times were communicated. Patient satisfaction measures whether those events met the patient’s prior expectations. A patient with low expectations can report high satisfaction despite receiving mediocre care, making satisfaction scores less reliable for identifying specific process failures.
Better patient experience is associated with higher treatment adherence, lower readmission rates, and stronger retention. Patients who feel heard and well-informed follow care instructions more consistently. For practices operating in competitive markets, experience quality also directly affects online reviews, referrals, and, in US hospital settings, Medicare reimbursement through HCAHPS-linked payment adjustments.
Private clinics typically use post-visit surveys (sent within 24 hours), Net Promoter Score questions, and public review platforms. CAHPS-style survey instruments from the AHRQ provide standardized, validated questions designed to capture observable events rather than general sentiment. Automated survey dispatch through practice management software increases response rates significantly compared to manual outreach.
It covers every interaction from the first booking attempt (online, phone, or referral), through pre-visit communications and intake, the clinical encounter itself, post-visit aftercare instructions, follow-up and recall messaging, and finally billing transparency. Each touchpoint either reinforces or erodes overall perception. In elective and private clinic settings, pre-visit and post-visit phases often carry more weight than the clinical encounter itself.
A positive patient experience means a patient felt informed, respected, and well-managed throughout their interaction with a practice. Concretely: their appointment started close to schedule, staff communicated clearly, they understood their treatment plan and costs before agreeing to proceed, follow-up communications arrived as expected, and they had a clear path to contact the clinic with questions. Absence of any one of these elements reduces overall experience quality.










