Key Takeaways
Ambulatory EHR vs inpatient EHR: ambulatory systems serve outpatient clinics; inpatient systems serve hospitals with overnight stays
Ambulatory EHRs support electronic prescribing to outside pharmacies; inpatient EHRs use CPOE for in-house medication orders
Inpatient EHRs require integration across hospital departments before go-live, making implementation significantly more complex and costly
Independent and private practices almost always need ambulatory EHR software, not hospital-grade inpatient systems
Choosing the wrong EHR category can mean paying for capabilities you will never use, or missing features your practice cannot operate without. A four-provider dermatology clinic spent eight months implementing a hospital-grade EHR before discovering it could not handle their outpatient scheduling volume without custom configuration that cost more than the software itself. They switched to an ambulatory platform and were fully live in three weeks. That gap between ambulatory EHR vs inpatient EHR is not a technicality – it determines whether your software works with your clinical workflow or against it.
Ambulatory EHR vs Inpatient EHR: What Each System Is Designed to Do
The ambulatory EHR vs inpatient EHR distinction starts with care context. An ambulatory EHR is built for outpatient settings where patients arrive, receive care, and leave the same day. A general practice, dermatology clinic, physiotherapy centre, or medical spa all operate in ambulatory mode. The visit is self-contained, and the system needs to support scheduling, documentation, prescribing, and billing for that discrete encounter.
Inpatient EHRs, also called acute care EHRs, are built for hospital environments where patients are admitted, monitored continuously, and discharged after stays that typically exceed 24 hours. According to the ONC (Office of the National Coordinator for Health IT), certification criteria for these two EHR categories differ substantially because their clinical workflows are fundamentally different. An inpatient system must coordinate nursing, pharmacy, lab, radiology, and multiple physician teams in real time. An ambulatory system coordinates a much smaller set of workflows around a single provider and patient encounter.
| Dimension | Ambulatory EHR | Inpatient EHR |
|---|---|---|
| Care setting | Outpatient clinics, private practices | Hospitals, acute care facilities |
| Patient stay | Same-day visit, no overnight | Admission with overnight or multi-day stay |
| Prescribing | Electronic prescribing (eRx) to outside pharmacies | CPOE for in-house medication management |
| Implementation | Lower complexity, faster go-live | Multi-department integration required before launch |
| Start-up cost | Lower, often subscription-based | High, often seven-figure enterprise deployments |
| Primary users | Physicians, nurses, front-desk staff in small teams | Large multidisciplinary clinical teams across departments |
Core Features of an Ambulatory EHR System
Understanding what an ambulatory system actually does is the fastest way to confirm whether it fits your practice. These features are common across most modern EHR systems for private practice:
- Patient scheduling and calendar management: Appointment booking, waitlist handling, and automated reminders built around outpatient visit workflows.
- Clinical documentation: Encounter notes, SOAP notes, and treatment records scoped to a single visit rather than a continuous hospital stay.
- Electronic prescribing (eRx): Sends prescriptions directly to outside pharmacies, which inpatient systems do not need because medications are managed in-house via CPOE.
- Lab integration: Ordering tests and receiving results from external labs, not an internal hospital laboratory.
- Billing and revenue cycle management: Claim submission, insurance verification, and patient invoicing for outpatient encounters.
- Patient engagement tools: Portals, intake forms, pre- and post-care instructions, and recall messaging.
- Telehealth: Many modern ambulatory platforms include video consultation support within the same workflow.
The absence of bed management, discharge planning, and cross-department order routing is not a limitation. Those capabilities simply do not apply to outpatient care. An ambulatory EHR is designed to be lean and fast, supporting high appointment volumes across a small team without the infrastructure overhead of a hospital system.
Core Features of an Inpatient EHR System
Inpatient EHRs solve a different class of problem. A patient admitted to a hospital interacts with nursing staff, attending physicians, specialists, pharmacists, radiologists, and lab technicians, sometimes simultaneously. The EHR must give every team member an accurate, real-time picture of the patient’s status across all of those interactions.
- Admission, discharge, and transfer (ADT) management: Tracks every patient as they move through the facility, from admission through bed assignment to discharge.
- Computerized Physician Order Entry (CPOE): Physicians enter orders for medications, labs, imaging, and procedures directly into the system for execution by the relevant department.
- Medication reconciliation: Reconciles a patient’s home medications against those administered during the inpatient stay, critical for preventing adverse drug events.
- Continuous vital sign monitoring and nursing documentation: Captures data flows that do not exist in short ambulatory visits.
- Discharge summary generation: Produces structured handoff documentation for the patient’s primary care or specialist upon discharge.
- Cross-departmental data integration: Real-time data sharing between emergency, ICU, pharmacy, lab, radiology, and clinical departments.
Implementing an inpatient EHR requires integrating all of these departments before the system can go live. That is a fundamentally different project from deploying an ambulatory platform for a five-clinician practice. The complexity, cost, and timeline reflect that difference.
Certification and Regulatory Differences Between Ambulatory and Inpatient EHRs
Both ambulatory and inpatient EHR systems can be certified under the ONC Health IT Certification Program, but the criteria differ by care setting. The ONC maintains separate certification criteria for ambulatory and inpatient EHRs, reflecting the distinct clinical functions each must support. Under the 21st Century Cures Act, both categories are subject to information-blocking rules and must support HL7 FHIR-based interoperability, but the specific clinical and technical requirements diverge.
Ambulatory certification priorities: Patient access to records, electronic prescribing, clinical quality measures for outpatient populations, and care coordination between providers across separate practices.
Inpatient certification priorities: CPOE for medications and lab orders, drug-drug and drug-allergy interaction checking, medication reconciliation, and cross-department data exchange within a single facility.
CMS’s Promoting Interoperability program (formerly Meaningful Use) also has separate tracks for eligible professionals (primarily outpatient) and eligible hospitals. If your practice participates in any CMS quality programs, confirming that your EHR holds the correct certification category is essential for compliance. The ONC Certified Health IT Product List (CHPL) allows you to verify any vendor’s certification status before purchasing.
Pro Tip
Before evaluating any EHR vendor, check their ONC certification status on the CHPL database. Filter by care setting (ambulatory vs. inpatient) to confirm the product is certified for your use case. Vendors occasionally market inpatient-derived systems to outpatient practices without clearly disclosing the mismatch.
Implementation Complexity: Ambulatory EHR vs Inpatient EHR Timelines
One of the most practical differences between these two system categories is how long it takes to get from contract signing to a live, functioning system. This is an area where the ambulatory EHR vs inpatient EHR gap is especially wide.
An ambulatory EHR for an independent practice typically goes live in weeks to a few months, depending on data migration complexity and staff training requirements. A cloud-based ambulatory platform built for small-to-mid-size practices can often be operational within days for a new practice with no legacy data to migrate.
Inpatient EHR implementations are measured in months and years, not weeks. The requirement to integrate with every hospital department, conduct parallel testing across clinical and administrative teams, and validate workflows against patient safety standards makes enterprise hospital EHR deployments among the most complex software projects in healthcare. Budget overruns and timeline delays are common.
For clinic owners starting a new medical practice, this difference is consequential. Choosing a platform designed for hospital-scale implementation when you run a four-room outpatient clinic means months of configuration work before you see your first patient through the system.
Pabau is built for ambulatory care workflows
Pabau handles scheduling, clinical documentation, digital intake forms, electronic prescribing, billing, and patient engagement in one platform. Designed for independent and multi-location outpatient clinics, not hospital IT departments.

Where Practice Management Software Fits the Ambulatory EHR vs Inpatient EHR Picture
Many outpatient clinics do not realise that practice management software and EMR systems increasingly overlap in the ambulatory space. A standalone EMR handles clinical documentation. A practice management system (PMS) handles scheduling, billing, and patient communication. Modern ambulatory platforms combine both into a single integrated system.
Inpatient EHRs typically include PMS-equivalent modules because hospitals need them, but those modules are designed around hospital-specific workflows like ADT management, not outpatient scheduling logic. Attempting to use an inpatient system’s scheduling module for a clinic’s appointment book is possible in theory, but the configuration overhead and feature mismatch make it impractical for independent practices.
For private clinics, the better approach is an integrated ambulatory platform that combines clinical and administrative functionality in a single system. The best EMR software options for outpatient practices bundle scheduling, digital forms, clinical notes, billing, and patient engagement without requiring the separate module licensing typical of hospital enterprise systems.
How to Choose Between Ambulatory EHR vs Inpatient EHR for Your Practice
For the vast majority of independent and private clinic operators, this decision is straightforward. If your patients do not stay overnight, you need an ambulatory EHR. The more nuanced questions arise when practices operate in hybrid settings, share data with hospital systems, or are part of an integrated delivery network.
Work through these four criteria to confirm your system category:
- Care setting: Do any of your patients stay overnight for treatment? If no, you operate in an ambulatory setting. If yes, or if you manage a combination of inpatient and outpatient care (as some surgical centres do), you may need a system that bridges both or a separate ambulatory module from your hospital EHR vendor.
- Prescribing workflow: Do you send prescriptions to outside pharmacies? Ambulatory EHRs support eRx to retail and mail-order pharmacies. If your medication management is entirely in-house (as it would be in a hospital), CPOE is the relevant function.
- Integration requirements: Do you need real-time data sharing with a hospital’s lab, radiology, or pharmacy? Some ambulatory EHRs support HL7 FHIR-based integration with hospital systems. Others operate as closed ecosystems. If you are part of an integrated delivery network, ask prospective vendors about bi-directional hospital integration before selecting a system.
- Implementation budget and timeline: A solo practitioner or small group practice cannot absorb an enterprise EHR implementation project. If a vendor’s typical implementation timeline exceeds three months for a practice your size, that is a signal the system was designed for a different scale of organisation.
Specialty ambulatory practices have additional considerations. A dermatology clinic needs before-and-after photo management and skin mapping tools that a general ambulatory EHR may not include. A mental health practice requires structured therapy note templates, outcome measurement tools, and group session scheduling. A plastic surgery practice needs procedure planning and consent workflows. The right ambulatory platform is one that supports your specialty’s specific clinical documentation needs, not just the general outpatient workflow model.
AI and Automation in Modern Ambulatory EHR Workflows
One gap in most existing ambulatory EHR vs inpatient EHR comparisons is the role AI and automation now play in outpatient clinical workflows. This is an area where ambulatory-focused platforms have moved faster than hospital EHR vendors in recent years.
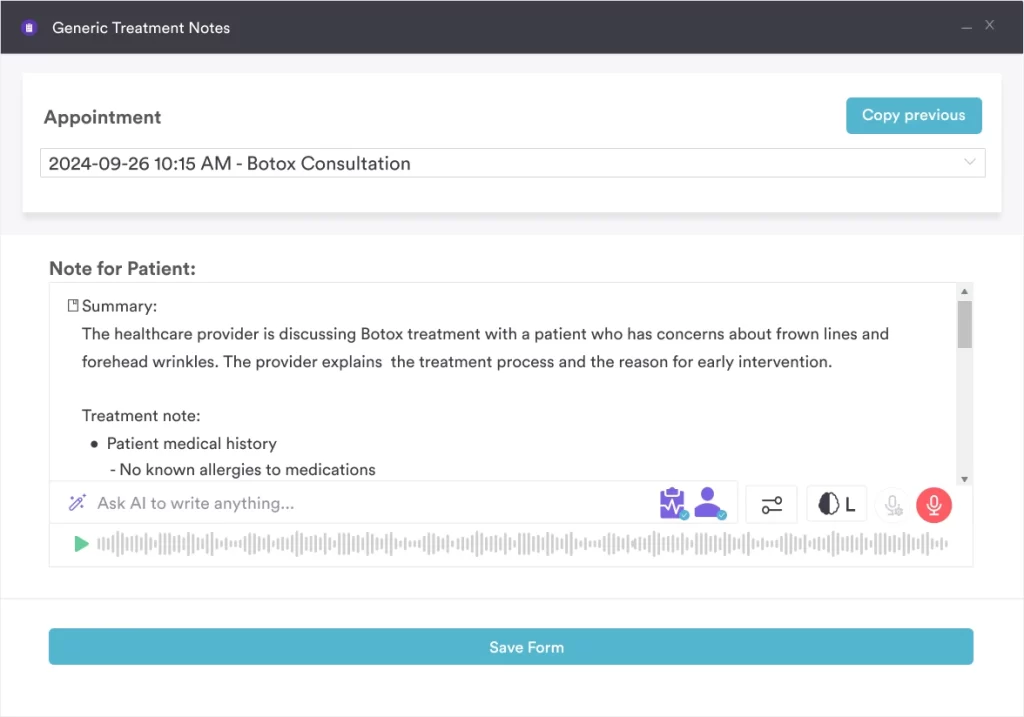
AI-powered clinical documentation tools, often called AI scribes, listen to a consultation and generate structured clinical notes automatically. For outpatient practitioners seeing 20 to 30 patients per day, documentation time is one of the largest sources of administrative burden. Research published in PMC (PubMed Central) on national ambulatory physician EHR use found that a significant proportion of EHR time occurs outside of clinic hours, indicating that documentation overhead extends well beyond the consultation itself.
Automation also reshapes the patient journey in ambulatory care. Automated recall messages, digital intake forms sent before the appointment, and post-treatment care instructions sent automatically after discharge all reduce manual administrative work without requiring hospital-grade infrastructure. Pabau’s Pabau Scribe handles clinical note generation within the ambulatory workflow, while automated workflows handle recall, follow-up messaging, and patient communications without staff intervention.
Pro Tip
When evaluating ambulatory EHR vendors, ask specifically whether AI documentation tools are included in the base subscription or charged separately. Some platforms offer AI scribe features as premium add-ons that double the effective cost. Pabau includes Pabau Scribe within the platform.
Inpatient EHR vendors have invested in AI for areas like sepsis prediction and medication safety alerts, which serve the acute care context. For an independent outpatient clinic, those capabilities are not relevant. The AI priorities in ambulatory care centre on documentation efficiency, patient retention, and workflow automation at the individual practice level.
Expert Picks
Need an EMR built specifically for your clinic type? Best EMR Software covers the top ambulatory platforms for outpatient practices across specialties.
Running a private practice and evaluating your options? Best EHR for Private Practice breaks down what independent practitioners should prioritise in an ambulatory system.
Wondering how AI documentation fits your workflow? AI Scribes: Impact on Patient Care examines how automated note generation changes day-to-day clinical documentation for outpatient providers.
Looking for EHR software that handles billing too? Practice Management System vs EMR explains when a combined platform outperforms two separate tools.
Conclusion
If your patients walk in and walk out the same day, you need an ambulatory EHR. The decision framework is straightforward: match the system to the care setting, verify the certification pathway covers your reporting requirements, and confirm the implementation timeline fits your operational capacity. Choosing a hospital-grade system for an outpatient clinic does not give you more capability – it gives you more configuration overhead, longer onboarding, and features designed for workflows you will never run.
Pabau is an ambulatory EHR and practice management platform built for outpatient clinics, from single-provider practices to multi-location groups. It combines digital intake forms, clinical documentation, automated workflows, and billing in one system designed for the pace and structure of outpatient care. To see how it handles your specific clinical workflows, book a demo and walk through the platform with a specialist.
Frequently Asked Questions
An ambulatory EHR supports outpatient visits where patients do not stay overnight. An inpatient EHR supports hospital admissions with continuous monitoring, multi-department coordination, and discharge planning. The clinical workflows, features, and certification requirements differ substantially between the two categories.
Outpatient clinics need an ambulatory EHR, not a hospital-grade inpatient system. The best ambulatory EHR for your clinic depends on specialty, practice size, and whether you need integrated billing and practice management alongside clinical documentation.
Yes. Electronic prescribing to outside pharmacies (eRx) is a core ambulatory EHR capability. Inpatient systems use Computerized Physician Order Entry (CPOE) for in-house medication management and do not typically support external pharmacy prescribing in the same way.
The ONC Health IT Certification Program maintains separate criteria for ambulatory and inpatient EHRs. Ambulatory certification emphasises patient access to records, eRx, and outpatient quality measures. Inpatient certification focuses on CPOE, medication reconciliation, and cross-department data integration. You can verify a vendor’s certification category on the ONC’s CHPL database.
Some large EHR vendors offer both ambulatory and inpatient modules. This can be advantageous for integrated delivery networks where hospital systems and affiliated physician practices want a shared data infrastructure. However, for independent outpatient practices with no hospital affiliation, a dedicated ambulatory platform is typically simpler and less expensive.










