Key Takeaways
Only 7-25% of PT patients complete their full plan of care, according to State of Rehab Therapy industry data – making dropout the single biggest revenue leak in outpatient practices.
Patient Retention Rate (PRR) is calculated as visits attended divided by visits prescribed, multiplied by 100 – track it per patient and practice-wide every month.
The first visit sets retention trajectory: patients who leave without booking a follow-up appointment are far more likely to drop out before completing their plan of care.
Pabau’s automated recall workflows, SMS reminders, and client portal reduce dropout by keeping patients engaged between visits and eliminating scheduling friction.
Fewer than one in four physical therapy patients completes their prescribed plan of care. According to the State of Rehab Therapy survey, PT clinics across the US see only 7-25% of patients attend all recommended visits – a range that has stayed stubbornly consistent for years. For a clinic running 300 active patients at any given time, that math translates to hundreds of incomplete treatment courses, poorer outcomes, and thousands of dollars in unrealised revenue every quarter.
This guide is for clinic owners, practice managers, and senior physiotherapists who already understand the clinical side but want a practical framework for measuring and improving patient retention in physical therapy. It covers how to calculate your retention rate, why patients drop out, and the specific operational strategies that move the needle.
Patient Retention in Physical Therapy: What the Numbers Actually Tell You
Patient retention in physical therapy is measured using the Patient Retention Rate (PRR): the percentage of prescribed visits a patient actually attends. The formula is straightforward.
Track PRR at both the individual patient level and the practice level. A single therapist with consistently low per-patient PRR signals a clinical or communication issue. A practice-wide drop signals a scheduling, billing, or operational problem. The distinction matters because the fix is different in each case.
One survey cited by Healthie found that patient retention can be as low as 7% in practices with more than one therapist – though the original survey source was not named, this directional data aligns with the State of Rehab Therapy findings. For physical therapy EMR users, this metric should be visible on a dashboard, not buried in a spreadsheet updated monthly.
Why Patients Drop Out of Physical Therapy
Dropout rarely happens for a single reason. It is usually a cascade: pain improves enough that motivation drops, then a scheduling conflict creates a gap, then the gap makes restarting feel harder than stopping. Understanding which factors are within your control is the first step.
- Perceived recovery: Patients feel “good enough” after 2-3 sessions and stop attending. This is the most common reason cited across PT literature – and it is addressable through better outcome tracking and patient education at the initial evaluation. Pabau’s patient compliance tools help clinics document and communicate progress milestones that show patients how far they have come and how far they have left to go.
- Scheduling friction: Difficulty booking follow-up appointments, long wait times, or inconvenient slots create an easy off-ramp. Appointment scheduling that allows online self-booking removes this barrier entirely.
- Cost and insurance barriers: Co-pay accumulation becomes a real obstacle for patients on high-deductible plans, particularly after 4-6 visits. Transparent cost communication at intake prevents surprise-driven dropout.
- Lack of therapist-patient rapport: The therapeutic alliance – the working relationship between clinician and patient – is one of the strongest predictors of treatment adherence in rehabilitation research. Practices that rotate patients between therapists without notice consistently see lower retention.
- Poor communication between visits: Patients who receive no contact between appointments feel forgotten. A single automated check-in message 48 hours after a visit can significantly change perceived care continuity.
The American Physical Therapy Association (APTA) emphasises patient education as a core component of evidence-based PT practice – not just about exercises, but about the full recovery timeline and what to expect at each stage. Clinics that build this education into their intake workflow reduce the “I feel better, so I’m done” dropout pattern measurably.
Five Strategies to Improve Patient Retention in Physical Therapy Clinics
Improving patient retention in physical therapy does not require a complete operational overhaul. The highest-impact changes target the moments where dropout risk is highest: the first visit, the gap between sessions, and the point where perceived recovery plateaus.
1. Book the Next Appointment Before the Patient Leaves
This is the single highest-leverage action in any retention strategy. A patient who leaves their first session without a scheduled follow-up is statistically more likely to disengage. The next appointment should be booked before the patient reaches the reception desk – ideally confirmed by the treating therapist during the session debrief. Pabau’s automated workflows can trigger a booking reminder automatically if a follow-up has not been scheduled within 24 hours of a completed visit.
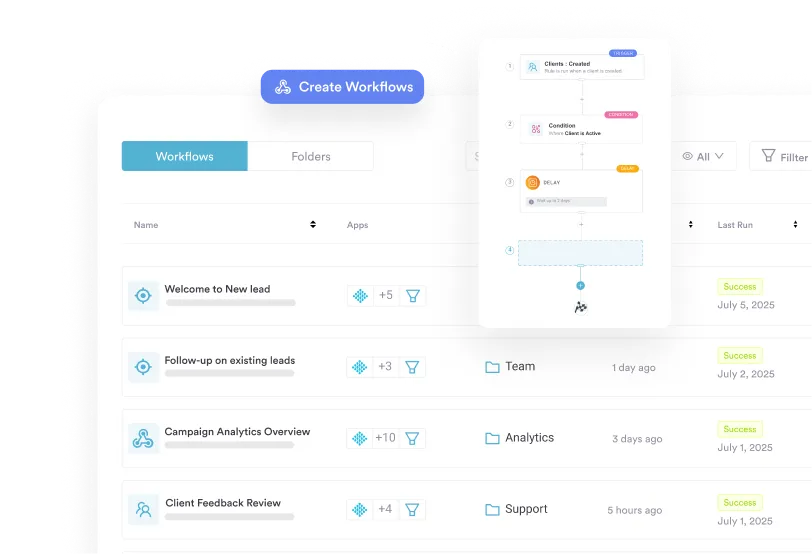
2. Use Automated Reminders to Close the Gap Between Visits
The period between appointments is where motivation erodes. Patients complete their home exercise programme (HEP) for two days, get busy, skip a few sessions, and then feel too embarrassed to return. A structured communication cadence – reminder 48 hours before the appointment, check-in 24 hours after, and a progress prompt mid-week – keeps the therapeutic relationship active without requiring staff time. Using SMS and email campaigns built into your practice management system ensures this happens consistently for every patient, not just the ones staff remember to call. Research consistently shows that automated appointment reminders reduce no-show rates – and a patient who shows up consistently is a patient who completes their plan of care.
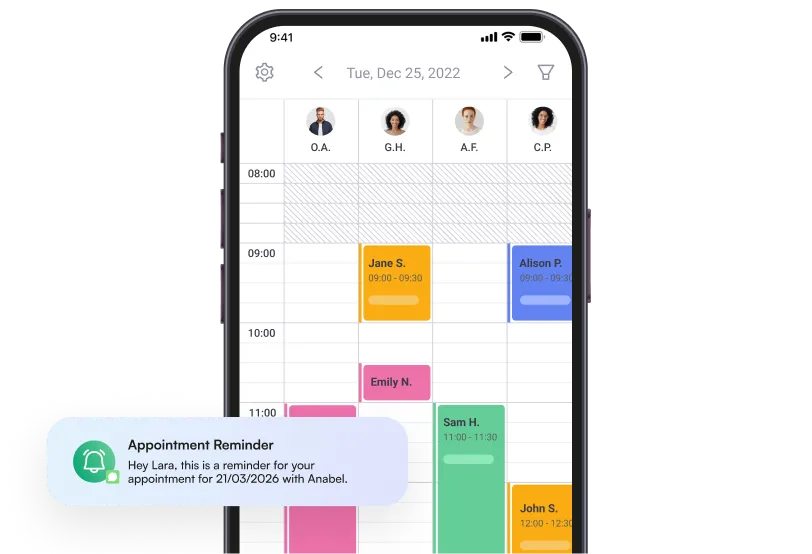
3. Make Progress Visible at Every Session
Patients who cannot see their own progress have no rational reason to continue attending. Functional outcome measures – range of motion improvements, pain scores, strength benchmarks – need to be documented and shared with the patient in plain language at each visit. Patient Reported Outcome Measures (PROMs) and Patient Reported Experience Measures (PREMs) give clinics structured data on both clinical progress and patient experience, which can surface dropout risk before a patient actually disengages.
Practices that track these metrics and share them with patients during sessions report stronger therapeutic alliance scores – the very factor that predicts treatment completion most reliably. A client portal that lets patients view their own records, progress notes, and exercise library between visits reinforces this transparency and keeps engagement high between appointments.
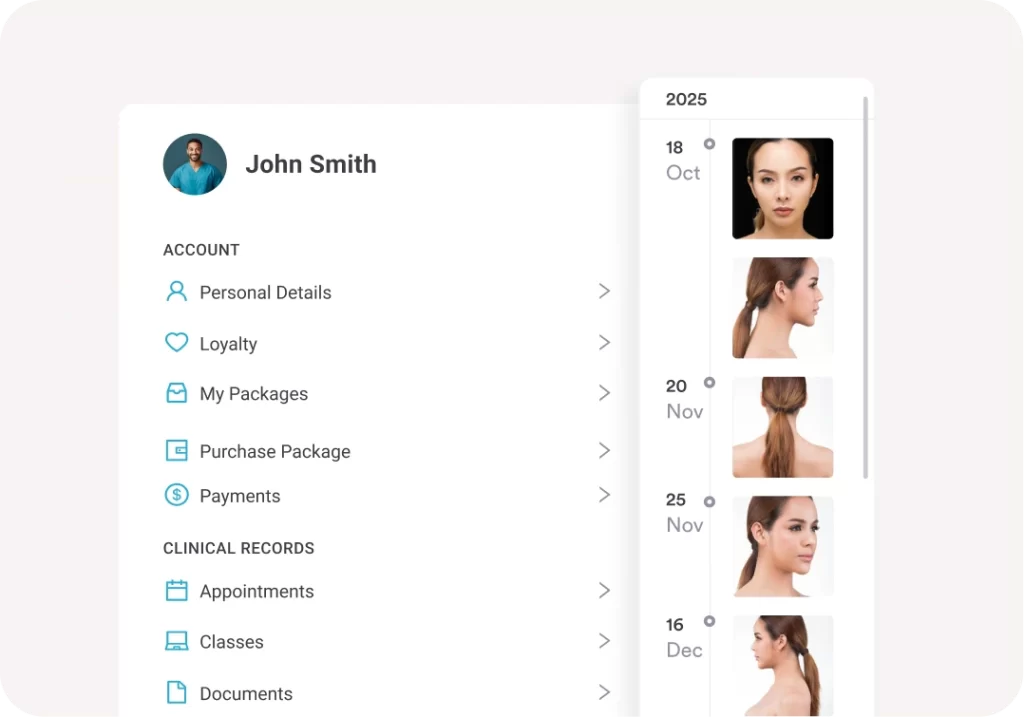
4. Address Scheduling and Access Barriers Proactively
A patient who misses one appointment due to a scheduling conflict is at moderate risk of dropout. A patient who misses two in a row is at high risk. Practices that monitor attendance gaps in real time and trigger outreach after a single missed visit recover far more patients than those who wait for the patient to reschedule themselves.
Telehealth physical therapy is not a replacement for hands-on treatment, but it is a proven tool for maintaining care continuity when a patient cannot attend in person. Regulatory acceptance varies by payer and jurisdiction – CMS has specific coverage rules for telehealth PT in the US, and the Chartered Society of Physiotherapy (CSP) provides guidance for UK practitioners. Using a system that supports patient engagement across both in-person and virtual touchpoints gives clinics the flexibility to adapt when patient circumstances change.
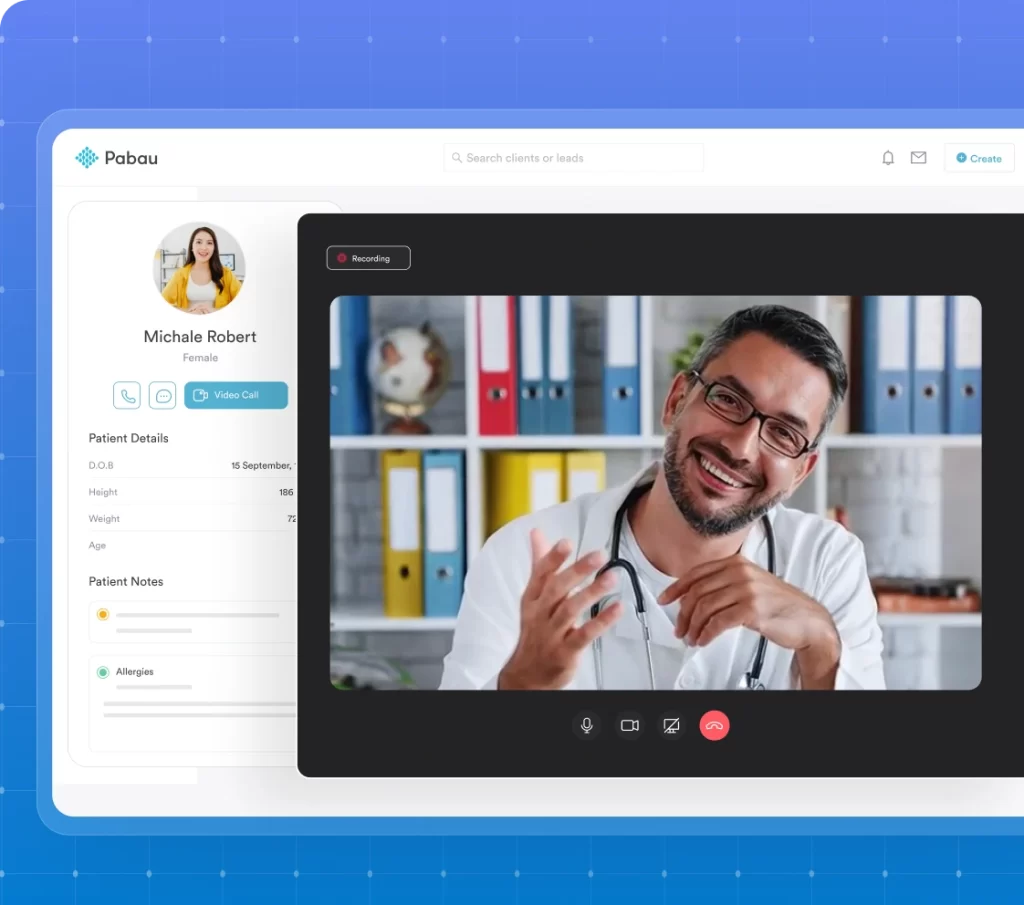
5. Build a Reactivation Workflow for Discharged Patients
Patient retention in physical therapy extends beyond the active plan of care. Former patients are your highest-converting acquisition channel – they already trust the clinic and have experienced results. A structured reactivation programme that contacts discharged patients at 30, 60, and 90 days after discharge (with outcome check-ins and relevant health tips) keeps the relationship warm and generates a predictable stream of returning patients without additional marketing spend. This same logic applies to physiotherapy clinic management software that tracks discharged patients and automates these touchpoints based on discharge date.
Pro Tip
Run a monthly PRR report segmented by therapist. If one clinician consistently shows lower retention rates than peers, the issue is almost always communication style or care planning depth at the first visit – not clinical competence. Targeted coaching at that specific touchpoint produces faster improvement than practice-wide protocol changes.
See How Pabau Reduces PT Patient Dropout
Pabau's automated recall workflows, appointment reminders, and client portal keep physical therapy patients engaged through every stage of their plan of care – without adding administrative work for your team.

The Role of Technology in Improving Patient Retention in Physical Therapy
Practice management software does not retain patients by itself. But it removes the operational friction that causes avoidable dropout. The highest-value technology features for PT retention are not the most complex ones – they are the ones that run automatically in the background while clinical staff focus on treatment.
- Automated appointment reminders: SMS and email reminders sent 48-72 hours before each appointment are the most straightforward dropout prevention tool available. Clinics using automated reminders consistently report lower no-show rates than those relying on manual calls alone.
- Online booking and self-scheduling: Patients who can book their next appointment at 9pm from their phone are significantly less likely to let a gap form. Removing the “I’ll call tomorrow” friction point matters.
- Digital forms and intake workflows: Streamlined intake reduces first-visit friction and gives clinicians the information they need to create a meaningful plan of care from session one – which directly affects the therapeutic alliance that drives retention.
- Patient portal access: Giving patients visibility into their own records, HEP instructions, and progress notes between visits keeps them invested in their recovery. Passive patients drop out; engaged patients complete their plans of care.
- Outcome tracking and reporting: A dashboard that surfaces patients with declining attendance or incomplete plans of care lets clinic managers intervene before a patient officially disengages. Early intervention is far more effective than reactivation.
For practices evaluating their current systems, it is worth asking whether your existing software makes these workflows easy or whether staff are working around limitations. The administrative burden of manual reminder calls, paper-based intake, and spreadsheet outcome tracking adds up – and the cost of opening and sustaining a physiotherapy clinic makes operational efficiency a direct financial priority, not just a convenience.
How to Track Patient Retention Metrics Across Your Practice
Improving retention requires measuring it consistently. Many PT practices calculate PRR at discharge – too late to intervene. The practices with the highest retention rates monitor attendance in real time and use attendance patterns as early warning signals.
A practical reporting structure for most outpatient PT clinics looks like this:
- Weekly: Flag any patient who has missed two consecutive appointments without rescheduling. Trigger a personal outreach call within 48 hours.
- Monthly: Calculate practice-wide PRR and segment by therapist, condition type, and payer. Patterns by payer often reveal insurance-related dropout that can be addressed through cost transparency conversations at intake.
- Quarterly: Review plan of care completion rates and compare against your baseline. Set a specific improvement target (for example, moving from 40% to 55% plan completion within two quarters).
- At discharge: Send a structured patient satisfaction survey. The data informs both clinical quality improvement and retention strategy refinement.
Practices using integrated reporting – where appointment data, billing data, and clinical notes live in the same system – can generate these reports without manual data pulling. If your current workflow requires exporting from three different systems to produce a retention report, that friction is itself a barrier to using the data.
Tools like clinic reporting and analytics built into your practice management platform can surface PRR trends, attendance gaps, and discharge rates without requiring a dedicated analyst. For multi-location practices, cross-site reporting is particularly valuable for identifying which locations need operational support.
Expert Picks
Running a physiotherapy clinic and want a compliance and operations overview? Mandatory Compliance for Physiotherapy Clinics covers the regulatory requirements that affect day-to-day operations in UK and international physiotherapy settings.
Looking to understand what patient engagement tools actually do? Improve Patient Engagement breaks down the specific features and workflows that keep patients active between visits across different clinic types.
Want to benchmark your clinic against physical therapy software options? Physical Therapy EMR outlines the practice management features built specifically for PT workflows, from documentation to recall automation.
Conclusion
Patient retention in physical therapy is not a clinical problem – it is an operational one. The treatments work. The dropout happens because of scheduling gaps, poor communication between visits, and patients who cannot see their own progress clearly enough to stay motivated. Each of these is solvable with the right workflows in place.
Pabau’s automated recall system, built-in patient communication tools, and real-time attendance reporting give PT clinics the infrastructure to catch dropout risk early and act on it before a patient disengages. If you are ready to see how this works in practice, book a demo and we will walk through the specific workflows relevant to your clinic size and patient mix.
Frequently Asked Questions
Industry benchmarks suggest that PT clinics with strong retention systems achieve PRR scores of 70-85% or higher. The State of Rehab Therapy survey indicates the average is far lower – often 7-25% of patients complete their full plan of care. If your practice-wide PRR is below 60%, that is a meaningful signal that operational changes are needed.
Divide the number of visits a patient attended by the number of visits prescribed in their plan of care, then multiply by 100. A patient prescribed 12 visits who attends 9 has a PRR of 75%. Track this per patient and aggregate it practice-wide monthly to identify trends.
The most common reasons are perceived recovery (feeling better and assuming treatment is complete), scheduling friction, cost accumulation from co-pays, and limited communication between visits. Practices that address all four through structured protocols – not just one or two – see the most significant improvement in plan completion rates.
Automated reminders reduce no-shows by keeping the upcoming appointment top of mind and removing the friction of manual rescheduling. Practices that send SMS or email reminders 48-72 hours before each visit consistently report fewer missed appointments than those relying on manual reminder calls. The effect compounds across a full plan of care.
The first visit establishes the therapeutic alliance, sets expectations for the recovery timeline, and – critically – should end with the next appointment already scheduled. Patients who leave the initial evaluation without a follow-up booking are significantly more likely to disengage. Many experienced PT clinics treat first-visit booking conversion as a primary performance metric for their clinical team.










