Key Takeaways
Functional medicine practitioners must hold an active healthcare license; IFM’s certifications require completion of IFM’s accredited coursework, a written case report, and a written exam.
Your business structure (LLC vs. PLLC vs. PC) must comply with state corporate practice of medicine laws, which vary significantly by license type.
Most functional medicine practices operate on a cash-pay or hybrid model, requiring clear fee transparency and a written financial policy from day one.
Pabau’s functional medicine software handles long intake forms, complex patient timelines, lab tracking, and automated follow-ups in a single platform.
Most practitioners who launch functional medicine clinics underestimate one thing: the administrative load. A conventional 15-minute visit generates a short SOAP note. A functional medicine new-patient encounter generates a 90-minute intake, a 10-page health history, timeline mapping, lab requisitions, and a multi-page treatment protocol. Do that for 20 patients a week without the right systems and the clinical work suffers. This guide covers how to start a functional medicine practice with the credentials, legal structure, technology, and operations in place before you see your first patient.
This guide is written for licensed clinicians: physicians (MD/DO), nurse practitioners, physician assistants, naturopathic doctors, and other credentialed providers considering an independent or group functional medicine practice. It covers the full launch sequence, from certification through your first 90 days of operations.
How to Start a Functional Medicine Practice: Credentials and Scope
Functional medicine is not a separate licensure category. According to the Institute for Functional Medicine (IFM), this approach can be incorporated into nearly every business model, including health systems, institutional settings, and independent practices. What governs your scope is your underlying professional license, not a credential alone.
For prescribers (MD, DO, NP, PA), that means your state medical or advanced practice board defines what you can order, prescribe, and bill. For non-prescribers (registered dietitians, health coaches, chiropractors, naturopathic physicians), scope is narrower and varies considerably by state. Understanding this before you design your service menu prevents a compliance problem later.
IFM Certification (IFMCP)
The IFMCP (Institute for Functional Medicine Certified Practitioner) has historically been the most recognized credential in the field. It is earned by completing IFM’s Applying Functional Medicine in Clinical Practice (AFMCP) course plus all six Advanced Practice Modules (Bioenergetics, Cardiometabolic, Environmental Health, GI, Hormone, and Immune), submitting and passing a written case report, and passing a written exam – a pathway that typically spans 2 to 4 years.
In 2026, IFM launched a new Functional Medicine Certification Program under its International Board of Functional Medicine Certification (IBFMC), offering two newer credentials: the FMCP (Functional Medicine Certified Professional), for licensed health practitioners whose scope of practice is more focused, and the FMCP-M (Functional Medicine Certified Professional – Medical), for physicians, nurse practitioners, physician assistants, and naturopathic doctors whose scopes include diagnosing, prescribing, and ordering labs. Candidates pursuing these competency-based credentials may accumulate 100 or more hours of accredited functional medicine training to meet the requirements. All IFM certifications require an active, permanent professional healthcare license; student, residency, and temporary licenses do not qualify. Naturopathic physicians in non-licensing states must present licensure from a state that does recognize the ND degree.
Additional training programs include the Kalish Institute (clinical systems and lab interpretation) and the Kresser Institute (ADAPT framework). None of these replace your professional license. They supplement clinical knowledge and signal to patients that you have completed structured functional medicine training beyond your core degree.
Practitioners running an integrative medicine practice alongside functional services should note that the American Board of Integrative Medicine (ABOIM) offers a separate board certification for physicians looking to formalize integrative medicine credentials.
Legal Structure and Business Setup
Corporate practice of medicine (CPOM) laws exist in most states and restrict who can own a medical practice. Physicians can generally form a Professional Corporation (PC) or Professional Limited Liability Company (PLLC). Non-physician providers face stricter constraints. In Texas, for example, a physician assistant cannot be a majority owner of a medical business, meaning a PA-led practice requires a physician co-owner to satisfy state law. Verify current requirements with a healthcare attorney in your state before filing anything.
- LLC: Most common for non-clinical businesses. May not be available to physicians practicing medicine in CPOM states.
- PLLC (Professional LLC): Available to licensed professionals in many states. Provides liability protection while satisfying professional licensing requirements.
- PC (Professional Corporation): Required in some states for physician-owned practices. More rigid governance structure than an LLC.
- Solo DBA: Sole proprietorship operating under a business name. Simplest setup, zero liability protection. Only appropriate for very low-risk service models.
Beyond entity type, you will need: a National Provider Identifier (NPI) number from CMS (free at NPPES), a DEA number if you will prescribe controlled substances, state business registration, a federal EIN from the IRS, and a HIPAA-compliant business infrastructure before you see your first patient. The guide to starting a medical practice covers the full compliance checklist in detail.
Building Your Business Plan
A functional medicine business plan differs from a conventional practice plan in one critical way: revenue projections cannot rely on insurance reimbursement rates. Extended lab consultations, root-cause workups, and long-form intake visits are not fully reimbursable under standard payer contracts. The financial model must account for this from day one.
Your medical practice business plan should address four core financial areas:
- Revenue model: Cash-pay, hybrid (some insurance + cash-pay for extended services), membership/retainer, or direct primary care. Most functional medicine practices use cash-pay or hybrid.
- Startup costs: Licensing and certification fees, malpractice insurance, office lease or virtual platform costs, EHR/practice management software, lab account setup, initial marketing. Startup costs for a lean virtual practice can be under $15,000; a physical clinic typically requires $40,000-$100,000 or more depending on build-out and equipment.
- Fee structure: New patient initial consultation (commonly $300-$600), follow-up visits ($150-$350), lab review consultations, and supplement dispensing revenue if applicable. These figures vary by market, specialty mix, and practitioner experience.
- Break-even analysis: Calculate the minimum patient volume at your average revenue per visit to cover fixed monthly costs. For a solo practitioner seeing 15 patients per week, this is usually achievable within 6-12 months of launch.
Malpractice insurance is a non-negotiable line item. Work with a carrier familiar with integrative and functional medicine scope, as standard policies sometimes exclude certain testing or prescribing patterns common in this specialty. Expect premiums between $2,000-$8,000 annually for a solo practice, depending on state, specialty, and coverage limits.
Pro Tip
Run your break-even calculation before signing a lease or hiring staff. Divide your total fixed monthly costs by your average revenue per patient visit. That number is the minimum patients per month you need to cover overhead. Add 20% as a buffer. If the number is unrealistic for your market or patient base, adjust your fee structure or reduce fixed costs before committing to a physical location.
Choosing Your Practice Model and Clinical Offerings
The direct primary care model and functional medicine overlap considerably: both prioritize longer visits, care continuity, and a patient-provider relationship not constrained by per-visit insurance billing. But they are not identical, and your choice of model determines your pricing, patient volume, staffing, and technology requirements.
| Practice Model | Visit Structure | Billing Approach | Best For |
|---|---|---|---|
| Cash-pay only | 60-90 min new patient, 30-45 min follow-up | Patient pays directly at time of service | Practitioners exiting insurance entirely |
| Hybrid (insurance + cash) | Standard visits billed to insurance; extended services cash-pay | Mixed; CPT codes for covered services | Practitioners maintaining some insurance relationships |
| Membership/retainer | Monthly or annual fee covers defined visit access and services | Flat monthly/annual fee; not insurance-billable | Practices emphasizing care continuity and chronic disease management |
| Virtual only | All appointments via telehealth | Cash-pay or hybrid; state telehealth laws apply | Practitioners targeting broad geographic reach |
Virtual practices have grown significantly, particularly for functional medicine where lab interpretation, dietary counseling, and supplement protocols can be delivered effectively via video. A telehealth-only setup eliminates lease costs and expands your potential patient base across state lines, provided you hold licensure in each state where patients are located. Pabau’s telehealth software integrates video consultations directly with patient records and automated follow-up workflows.
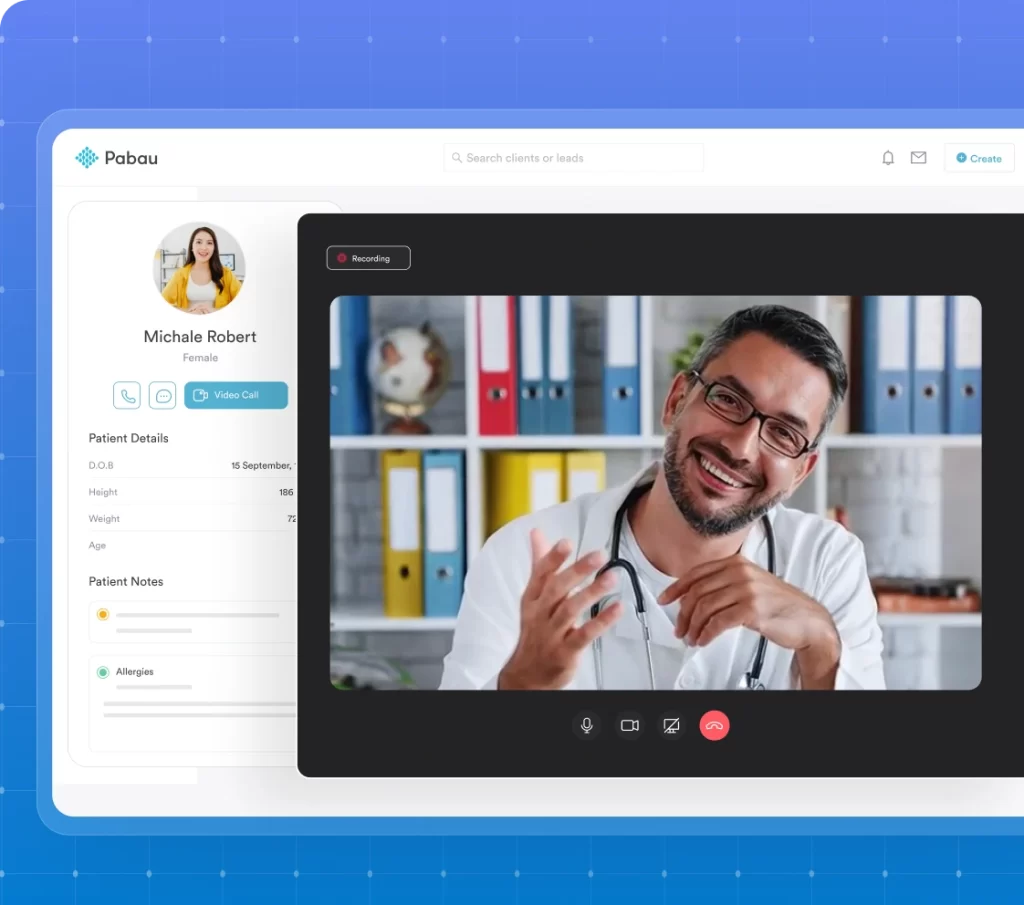
When designing your clinical menu, begin with your professional training and legal scope of practice, as IFM recommends. A common mistake is building a service menu around certifications rather than around what your license permits. An NP in a restricted practice state cannot offer the same menu as an MD in a full practice authority state, regardless of shared IFMCP credentials.
Run Your Functional Medicine Practice Without the Admin Overload
Pabau handles your long intake forms, lab tracking, treatment protocols, automated recalls, and telehealth in one platform built for complex clinical workflows. See how it works.

Technology Stack: EHR and Practice Management
Conventional EHR systems are built around 15-minute encounter notes and ICD-10 coding. Functional medicine documentation looks nothing like that. New patient intakes run 10-20 pages. Timeline reviews require structured fields for medical history across decades. Lab panels involve dozens of biomarkers with reference ranges that differ from conventional lab normals. A generic EHR forces practitioners to work around the system constantly.
Functional medicine software built for this workflow handles several requirements that conventional systems miss:
- Long-form intake and health history forms: Patients complete detailed questionnaires before their first visit. Digital intake forms sent automatically after booking eliminate manual data entry and reduce the pre-appointment workload significantly.
- Lab tracking and trend analysis: Functional labs involve dozens of markers across multiple panels. Software that stores lab results in structured fields and tracks trends over time is essential for the root-cause analysis approach.
- Treatment protocol templates: Structured note templates for functional medicine encounter types save documentation time without sacrificing clinical detail.
- Automated follow-up workflows: Recall reminders, pre-appointment preparation instructions, post-visit supplement protocols, and lab result notifications can all be automated, reducing staff time on outbound communication.
- HIPAA compliance infrastructure: All patient data, messaging, and telehealth sessions must meet HIPAA standards. Read the detailed guide to HIPAA compliance for medical offices before selecting any software.
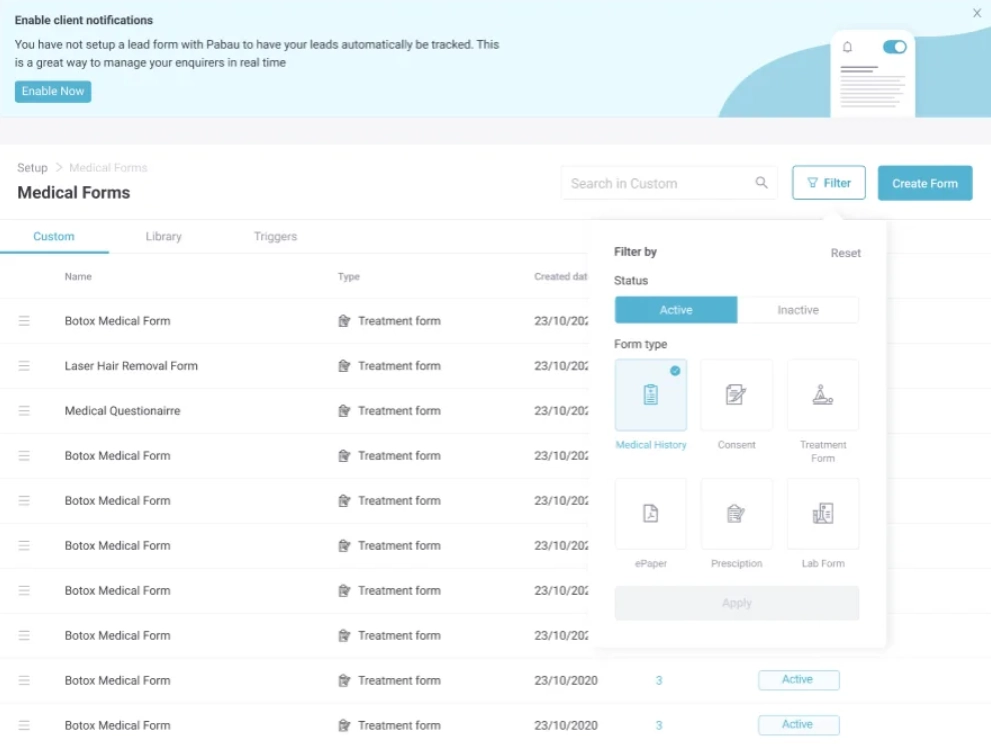
For clinical documentation specifically, AI-assisted clinical documentation tools can reduce the time spent on encounter notes by transcribing and structuring the clinical encounter in real time. For providers seeing complex patients with lengthy visit histories, this can recover 30-60 minutes per day in documentation time.
Marketing the Practice on a Lean Budget
These patients are typically self-referred, health-literate adults with chronic conditions who have not found answers in the conventional system. Their searches are specific: “functional medicine doctor near me,” “root cause thyroid doctor,” “integrative care for autoimmune conditions.” Your marketing should be built around how they search, not around broad brand awareness.
Four channels produce the highest return for a new practice in this specialty:
- Google Business Profile: Claim and fully optimize your profile before you see your first patient. Category selection matters: use “Functional Medicine Practitioner” or “Integrative Medicine” rather than generic “Medical Clinic.” Request reviews from early patients systematically.
- Content marketing: Long-form educational content targeting condition-specific searches (e.g., “functional medicine approach to Hashimoto’s,” “root cause treatment for IBS”) builds organic traffic from patients actively searching for your approach. This compounds over 12-24 months.
- IFM and ABOIM provider directories: Both organizations maintain searchable practitioner directories that drive qualified patient referrals. Completing your profile fully with conditions treated and geographic coverage improves visibility.
- Referral relationships: Conventional physicians who encounter patients with complex chronic conditions and limited treatment options often refer out. Building three to five referral relationships with primary care physicians or specialists in your area generates consistent patient flow.
Detailed guides on clinic marketing and strategies to grow your practice cover digital marketing, patient acquisition funnels, and reputation management in more depth. In this specialty, patient education content tied to your clinical approach consistently outperforms generic brand advertising.
Expert Picks
Need a complete software platform built for functional medicine? Functional Medicine Software covers intake forms, lab tracking, telehealth, and automated workflows in one system.
Planning your clinic’s financial model before launch? Medical Practice Business Plan walks through revenue projections, startup cost planning, and break-even analysis for independent practices.
Want to understand how AI documentation tools fit into a complex clinical workflow? Echo AI transcribes and structures clinical encounters in real time, recovering significant documentation time for high-volume practices.
Considering a direct primary care or membership model? Direct Primary Care Software explains the operational differences and technology requirements between DPC, membership, and cash-pay functional medicine models.
Conclusion
The administrative complexity of functional medicine, not the clinical complexity, stops most practitioners from launching. Long intakes, lab-heavy protocols, cash-pay billing, and patient education demands overwhelm practices that try to run them on systems designed for 15-minute appointments.
Pabau’s functional medicine software handles the operational layer: digital intake forms sent automatically after booking, structured lab tracking, automated recall workflows, and HIPAA-compliant telehealth, all in one platform. The benefits of private practice only materialize when your systems can keep pace with your clinical model. Book a demo to see how Pabau supports functional medicine workflows end to end.
Frequently Asked Questions
Any licensed healthcare provider can practice functional medicine, including MDs, DOs, NPs, PAs, naturopathic physicians, and registered dietitians, provided the services offered fall within their state-defined scope of practice. The functional medicine approach is a clinical framework, not a separate license category. Non-prescribers can offer nutrition counseling, lifestyle interventions, and health coaching within their scope, but cannot prescribe medications or order labs without appropriate licensure.
Coverage is highly variable. Standard office visits billed under CPT codes (e.g., 99213-99215) may be reimbursable if the provider is in-network. However, extended consultations, comprehensive lab panels, and many functional medicine-specific services are typically not covered by standard insurance plans. Most functional medicine practitioners operate on a cash-pay or hybrid model. Some practices use Health Savings Account (HSA) or Flexible Spending Account (FSA) eligibility to help patients offset out-of-pocket costs.
A lean virtual practice can launch for under $15,000, covering licensing, malpractice insurance, EHR software, and basic marketing. A physical clinic with build-out, equipment, and staffing typically requires $40,000-$100,000 or more depending on location and service mix. The largest variable cost is usually the physical space. Practitioners who start virtually and transition to in-person once patient volume justifies the overhead tend to reach profitability faster.
No specific functional medicine certification is legally required to practice. Historically, the IFMCP (Institute for Functional Medicine Certified Practitioner) has been the most widely recognized credential, earned by completing IFM’s AFMCP course, all six Advanced Practice Modules, a written case report, and a written exam alongside an active healthcare license. In 2026, IFM launched a new Functional Medicine Certification Program offering the FMCP (for licensed health practitioners) and the FMCP-M (for physicians, NPs, PAs, and NDs with broader scopes), each with its own competency-based requirements. The Kalish Institute and Kresser Institute also offer recognized training programs. Board certification through the American Board of Integrative Medicine (ABOIM) is available to physicians seeking a formal integrative medicine credential.
From an existing healthcare license, completing IFM’s required education and certification process typically takes 12-24 months of part-time study alongside clinical practice. Practitioners who complete accelerated programs may finish in 9-12 months, though applying functional medicine principles in complex patient cases takes considerably longer to develop. Building a functional medicine practice from licensure through consistent patient volume generally takes 18-36 months.