Key Takeaways
Behavioral health practice management EHR systems combine clinical documentation, scheduling, billing, and compliance into one integrated platform built for mental health workflows.
42 CFR Part 2 and HIPAA impose stricter confidentiality rules on substance use disorder records than standard healthcare data, requiring purpose-built EHR architecture.
Purpose-built behavioral health EHRs include validated outcome measures (PHQ-9, GAD-7) and specialty note formats (DAP, SOAP, BIRP) out-of-the-box, unlike general-purpose EHRs.
Pabau supports behavioral health clinics with customizable clinical forms, integrated telehealth, automated scheduling, and AI-assisted documentation through Echo AI.
Behavioral Health Practice Management EHR: What Makes It Different
A behavioral health practice management EHR is not just a general electronic health record with a mental health label applied. Practices running on general-purpose EHRs consistently report the same problem: the platform handles primary care workflows well but creates friction the moment a clinician needs to document a DAP note, track a PHQ-9 score over time, or apply 42 CFR Part 2 protections to a substance use disorder record.
This guide is for clinic owners, practice managers, and clinicians evaluating whether their current system is fit for purpose, or researching options for the first time. It covers what a behavioral health practice management EHR actually does, which features matter most, the compliance requirements that shape software architecture, and how to evaluate platforms against your practice’s specific operational model.
The market is crowded with options ranging from solo-therapist tools to enterprise platforms serving multi-location agencies. The right choice depends on practice size, payer mix, regulatory exposure, and workflow complexity, not on which platform has the most favorable review count.
Core Features Every Behavioral Health EHR Should Include
Most behavioral health EHR evaluations start and end with “does it have therapy notes?” That question is necessary but nowhere near sufficient. A mental health EMR that only handles documentation leaves practices managing scheduling in one system, billing in another, and outcomes measurement in a spreadsheet. That fragmentation adds administrative hours every week.
These are the core feature areas to evaluate, with the specific capabilities each one requires:
Clinical Documentation
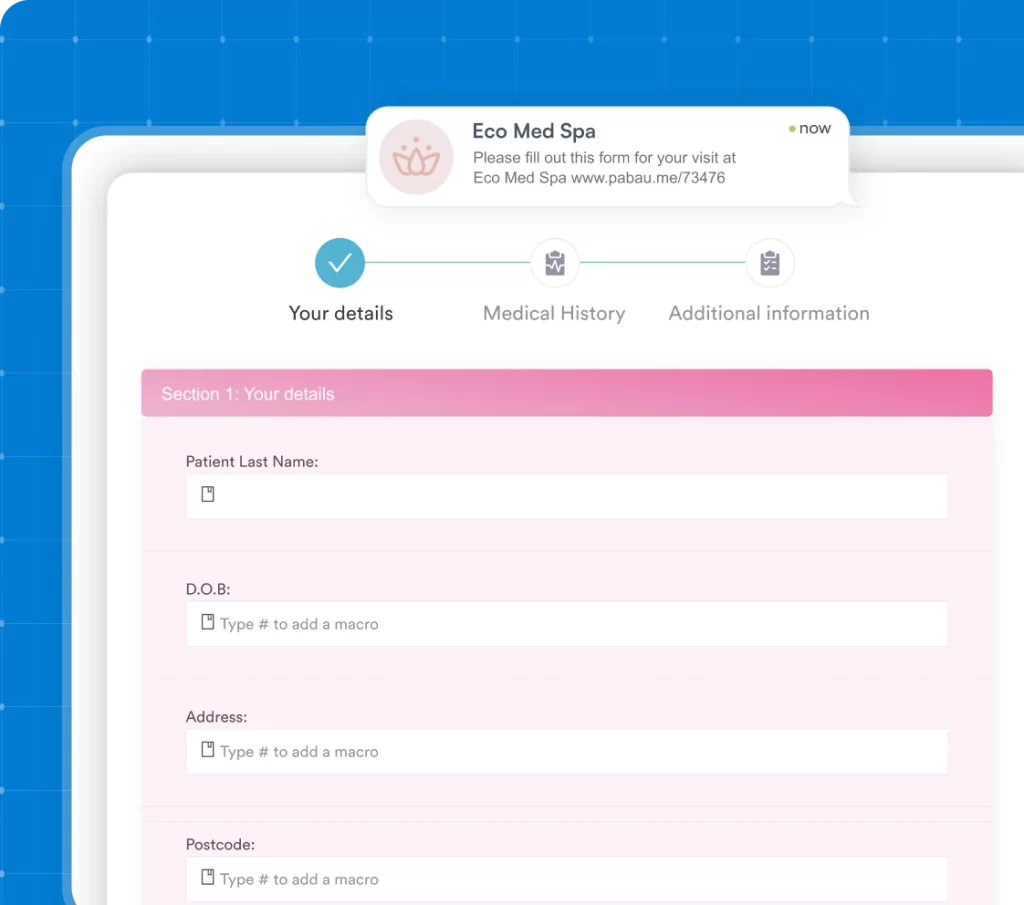
The documentation layer is where behavioral health EHRs earn their specialty label. General EHRs offer SOAP notes. Purpose-built behavioral health systems add DAP (Data, Assessment, Plan), BIRP (Behavior, Intervention, Response, Plan), and GIRP formats because different therapy modalities require different note structures. Beyond format variety, these systems should include pre-built digital intake forms incorporating validated outcome measures: the PHQ-9 for depression and GAD-7 for anxiety, both of which are public-domain instruments widely incorporated into behavioral health EHRs. Licensed instruments such as the BDI-II are also used in clinical practice but typically require separate Pearson licensing rather than out-of-the-box EHR inclusion.
Treatment plan templates, group therapy documentation, and risk assessment tools round out the clinical documentation picture. A platform that requires clinicians to build these from scratch is not purpose-built, regardless of how it markets itself.
Scheduling and Caseload Management
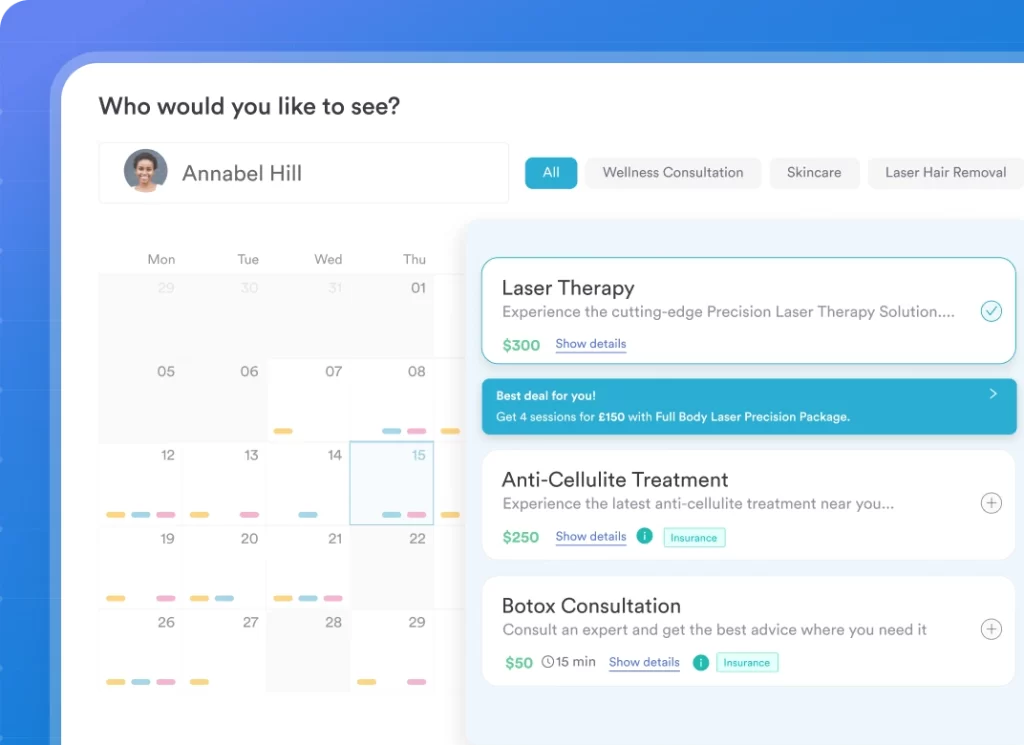
Behavioral health scheduling has specific demands: recurring weekly appointments, group session coordination, cancellation management across multiple therapists, and waitlist handling for high-demand practitioners. Solo practitioners have different needs than multi-location agencies running 15 clinicians across three sites.
Caseload management, the ability to see a clinician’s full client list with session frequency, outstanding notes, and care plan status, is a feature often missing from general scheduling tools. For psychiatry practice management, this visibility also covers medication review schedules and risk flag tracking per client.
Patient Portal and Communication
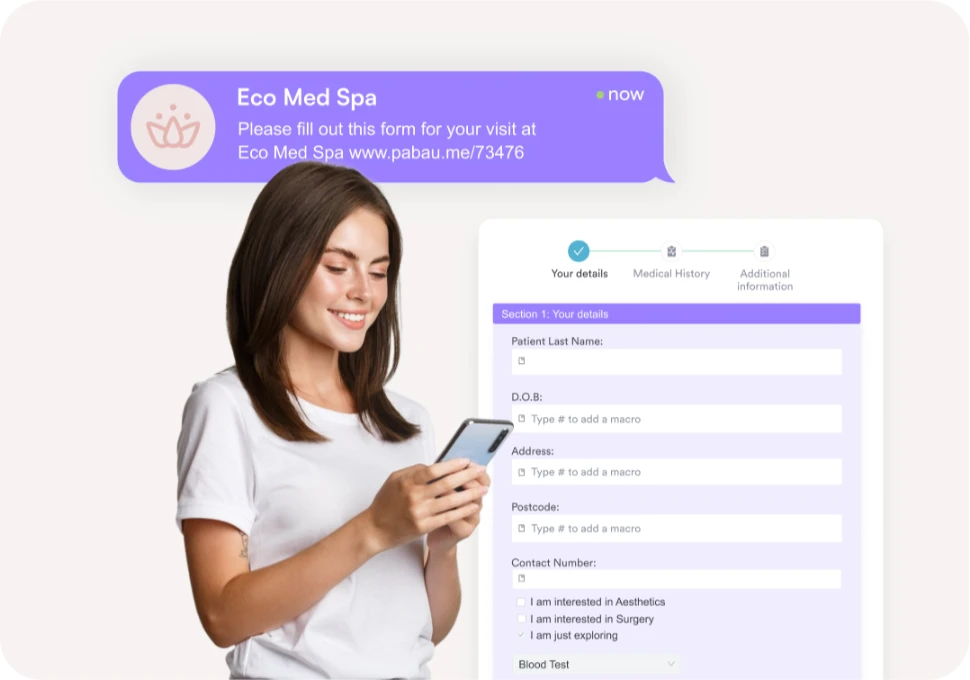
A client-facing portal is not optional in modern behavioral health. Clients complete intake forms before the first appointment, access their care documents, and receive session reminders through the portal. For practices running telehealth, the portal often serves as the entry point for virtual visits.
Secure messaging between clients and practitioners, handled within the EHR rather than through external email, supports both HIPAA requirements and therapeutic continuity between sessions. This matters especially for therapy practice management workflows where between-session communication is part of care delivery.
| Feature Area | Basic Requirement | Advanced Capability |
|---|---|---|
| Clinical Notes | SOAP templates | DAP, BIRP, GIRP + outcome measures (PHQ-9, GAD-7) |
| Scheduling | Single-provider calendar | Multi-provider, group sessions, waitlist, recurring appointments |
| Billing | Invoice generation | Insurance claims, ERA processing, prior authorization tracking |
| Compliance | HIPAA data encryption | 42 CFR Part 2 access controls, audit trails, BAA management |
| Telehealth | Third-party video link | Native HIPAA-compliant video embedded in patient portal |
| Outcomes | Manual score entry | Built-in validated tools with trend tracking over time |
HIPAA and 42 CFR Part 2: The Compliance Foundation
Every healthcare EHR must meet HIPAA requirements. Behavioral health adds a second compliance layer that many general EHRs are not architected to handle: 42 CFR Part 2, the federal regulation governing confidentiality of substance use disorder patient records. According to SAMHSA, 42 CFR Part 2 imposes strict rules on how substance use disorder information is recorded, stored, and shared, going significantly beyond standard HIPAA protections.
The practical difference matters. Under HIPAA, a treating provider can share records within a care team with implied consent. Under 42 CFR Part 2, substance use disorder records require explicit written patient consent before being shared, even with another treating provider. An EHR without 42 CFR Part 2 access controls built into its architecture forces manual workflows to enforce those protections, creating both compliance risk and administrative burden.
For practices serving clients with co-occurring disorders, where mental health and substance use treatment overlap, this distinction shapes EHR selection. The system must be able to apply different consent and disclosure rules to different record types within the same client file. Review HIPAA compliance requirements for clinic software to understand the broader framework before evaluating specific platform certifications.
Additional compliance considerations for behavioral health EHRs include:
- Business Associate Agreements (BAAs): Every vendor handling protected health information must execute a BAA. Verify this is standard practice before signing any contract.
- Audit trails: HIPAA requires logged access to all PHI. Behavioral health systems with 42 CFR Part 2 exposure need granular, query-level audit trails.
- ONC certification: The Office of the National Coordinator for Health Information Technology (ONC) certifies EHR modules for specific clinical functions. Not all behavioral health EHRs carry ONC certification, which affects interoperability and federal program eligibility.
- CCBHC compliance: Certified Community Behavioral Health Clinics (CCBHCs) require additional reporting and data submission capabilities per SAMHSA standards. If your organization operates under the CCBHC model, confirm the EHR supports those specific workflows before purchasing.
Pro Tip
Run a 42 CFR Part 2 scenario test during any EHR demo: create a mock client with both a mental health diagnosis and a substance use disorder record, then attempt to share only the mental health record with an external provider. If the system cannot selectively redact the SUD record, it lacks the access control architecture for compliant 42 CFR Part 2 workflows.
Billing and Revenue Cycle Management in Behavioral Health
Behavioral health billing operates on different CPT code sets than primary care. Psychotherapy codes (90832-90838), evaluation and management codes for psychiatric visits, and group therapy codes each carry specific documentation requirements, modifier rules, and payer policies. A billing module that works well for a general practice often creates denials when applied to behavioral health claims because it lacks the code-specific logic those services require.
Revenue cycle management in behavioral health involves several stages where errors accumulate:
- Eligibility verification: Mental health benefits often have separate deductibles and visit limits from medical benefits. Real-time eligibility checks before each session prevent billing surprises after service delivery.
- Prior authorization tracking: Many payers require authorization for ongoing therapy. An EHR that tracks authorization numbers, approved visit counts, and expiration dates within the scheduling workflow prevents over-service claims.
- Claims submission and ERA processing: Electronic remittance advice (ERA) processing automatically posts payments and identifies denial codes. Manual posting is the primary driver of revenue cycle delays in practices without integrated billing.
- Superbill generation: Practices billing clients directly need accurate superbills including diagnosis codes, CPT codes, and provider NPI numbers for insurance reimbursement. This should generate automatically at encounter close.
Pabau’s claims management software handles integrated billing and payment processing within the same platform as clinical records, reducing the need for separate billing tools. For practices with complex US insurance workflows, dedicated behavioral health billing platforms offer deeper payer-specific claim logic. The right choice depends on your payer mix and whether US insurance claims processing or private-pay efficiency is the priority.
Telehealth and AI Documentation in Modern Behavioral Health EHR Systems
Telehealth is now a permanent fixture in behavioral health delivery, not a pandemic accommodation. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), telehealth has significantly expanded access to behavioral health services, particularly in rural and underserved areas. The implication for EHR selection is direct: a platform with bolted-on third-party video creates workflow friction. Native integrated telehealth embedded in the EHR means the session, the note, and the billing record are created in the same environment without switching between applications.
Key telehealth requirements for behavioral health EHRs:
- HIPAA-compliant video that does not require clients to download separate applications
- Session notes that open automatically at appointment start time
- Client portal access for joining sessions without separate login credentials
- Telehealth-specific documentation indicating the modality and client location, required for many payers
AI-assisted clinical documentation is the emerging differentiator in the behavioral health EHR market. Clinicians using session transcription and note-generation tools report meaningfully less time on documentation after each session. Pabau’s Echo AI handles AI-assisted documentation, supporting note generation and clinical scribe workflows for practices that want to reduce the administrative burden of session notes. As with any AI documentation tool, clinical review and sign-off remain the practitioner’s responsibility. The AI handles the structural heavy lifting; the clinician validates clinical accuracy.
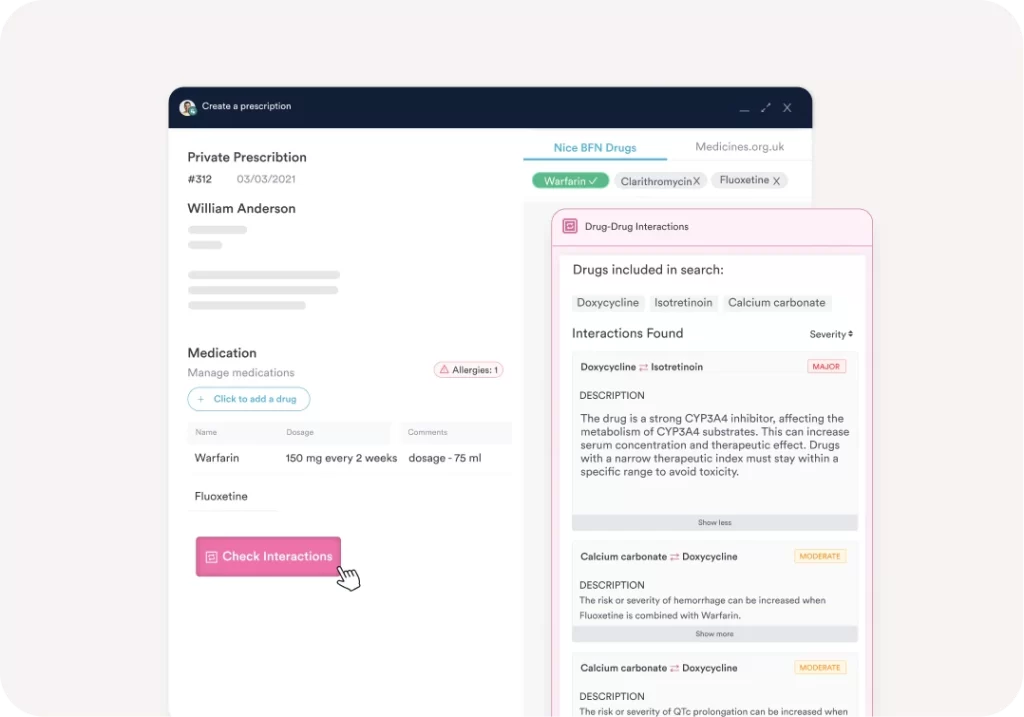
Outcomes measurement is another area where purpose-built behavioral health EHRs separate from general platforms. Administering the PHQ-9, GAD-7, or BDI electronically through the patient portal before each session, with automatic score trending visible in the clinical record, gives practitioners objective data to anchor treatment decisions. Practices using manual paper-based outcomes measurement typically administer these tools inconsistently. Built-in automated workflows can trigger outcome measure delivery before scheduled sessions without any manual action from administrative staff.
See How Pabau Supports Behavioral Health Practices
Pabau combines clinical documentation, scheduling, telehealth, billing, and AI-assisted notes in one platform. Built for multi-practitioner clinics running complex workflows.

How to Choose the Right Behavioral Health Practice Management EHR
The behavioral health EHR market divides roughly into three categories. Solo and small-group platforms are optimized for therapist-centric workflows, individual scheduling, and basic insurance billing. Mid-market platforms add multi-provider scheduling, group therapy management, and deeper payer integrations. Enterprise platforms serve large agencies and CCBHCs with multi-location reporting, complex access controls, and interoperability requirements.
Most practices buy the wrong category because they evaluate based on current size rather than 12-24 month trajectory. Migrating between EHR platforms is a significant operational project. Choose a system that fits where your practice is going, not just where it is today.
Evaluate these five decision criteria before selecting a behavioral health practice management EHR:
- Practice type and size: Solo practitioners with straightforward private-pay models have different requirements than multi-location groups running psychiatric services alongside therapy. A platform optimized for solo therapists will create friction at 10 clinicians. Confirm the platform you evaluate has documented deployments at your practice size and complexity.
- Payer mix: If your revenue is primarily insurance-based, deep CPT code libraries, ERA processing, and prior authorization tracking are non-negotiable. Private-pay practices can accept simpler billing tools. International or private-pay clinics, where Pabau has particular strength, may find purpose-built US insurance billing platforms unnecessarily complex.
- Regulatory exposure: Substance use disorder services require 42 CFR Part 2 compliance. CCBHC-certified organizations need reporting modules meeting SAMHSA standards. Confirm compliance architecture before signing.
- Integration requirements: Does your practice connect to a health system or ACO? HL7 FHIR interoperability may be required. Check whether the EHR carries ONC certification for the specific modules you need, as certification status affects both interoperability and federal program eligibility.
- Implementation timeline and support: EHR migrations carry real risk of workflow disruption and data loss. Evaluate vendor implementation support, training resources, and data migration capabilities explicitly. The content gap in current SERP results is notable here: almost no published guides address staff training and change management during a behavioral health EHR transition, yet this is frequently where implementations fail.
For practices exploring platform options, psychology practice software built on a multi-disciplinary clinical foundation offers flexibility as service offerings expand. Practices that start with individual therapy and later add psychiatry, group programs, or medication management need a platform that can grow with that clinical scope rather than requiring another migration.
Pro Tip
Request a live demo using your actual note template, your CPT codes, and a simulated insurance claim. Most EHR demos use vendor-prepared data that hides friction. Your own clinical workflow data reveals whether the system actually fits your practice, or whether you will be spending hours on workarounds every week.
Continue your research
Managing a multi-practitioner behavioral health clinic? Mental Health EMR covers the platform capabilities that support complex multi-provider clinical environments.
Need psychiatric-specific workflows? Psychiatry EMR Software outlines the documentation, prescribing, and risk management tools that psychiatric practices require.
Evaluating therapy practice platforms? Therapy Practice Management explains how integrated scheduling and clinical documentation reduce administrative overhead for therapy groups.
Conclusion
The gap between a general EHR and a purpose-built behavioral health practice management EHR is not cosmetic. It shows up in compliance architecture, specialty documentation formats, payer-specific billing logic, and the operational workflows that determine whether a practice runs efficiently or burns through clinical staff on administrative tasks.
Pabau supports behavioral health practices with customizable clinical forms, integrated telehealth, automated scheduling across multi-provider teams, and AI-assisted note documentation through Echo AI. For practices evaluating an integrated practice management platform that scales beyond individual therapy to multi-disciplinary clinical environments, book a demo to see how Pabau handles your specific workflow requirements.
Frequently Asked Questions
Purpose-built behavioral health EHRs include treatment plan templates that link presenting problems to measurable goals, intervention strategies, and review timelines. Clinicians complete an initial treatment plan at intake, update it at defined review intervals, and attach session notes to treatment plan goals. Some platforms trigger automatic review reminders based on the plan’s review schedule. The treatment plan, session notes, and outcome scores should all exist in the same client record for auditable continuity of care.
At minimum: specialty note formats (DAP, BIRP, SOAP), validated outcome measures (PHQ-9, GAD-7), treatment plan templates, HIPAA-compliant scheduling and telehealth, insurance billing with behavioral health CPT codes, 42 CFR Part 2 access controls for practices treating substance use disorders, a client portal for intake forms and secure messaging, and caseload management for multi-provider practices. E-prescribing and group therapy scheduling are additional requirements for psychiatric and group treatment settings.
An EHR covers clinical functions: notes, treatment plans, assessments, and the medical record. Practice management software covers operational functions: scheduling, billing, insurance claims, and reporting. Historically these were separate systems requiring integration. Modern behavioral health platforms combine both into one environment. Integrated systems reduce data entry duplication, eliminate the latency between clinical and billing records, and give administrators real-time visibility into both clinical caseload and financial performance without switching between applications.
Reputable behavioral health EHRs are designed with HIPAA compliance requirements built into their architecture, including data encryption at rest and in transit, role-based access controls, audit logging, and Business Associate Agreement execution. However, HIPAA compliance is not a one-time certification; it requires ongoing operational practices including staff training, risk assessments, and breach response procedures. Practices treating substance use disorder patients must also verify 42 CFR Part 2 compliance, which imposes additional consent and disclosure controls beyond standard HIPAA requirements.










