Key Takeaways
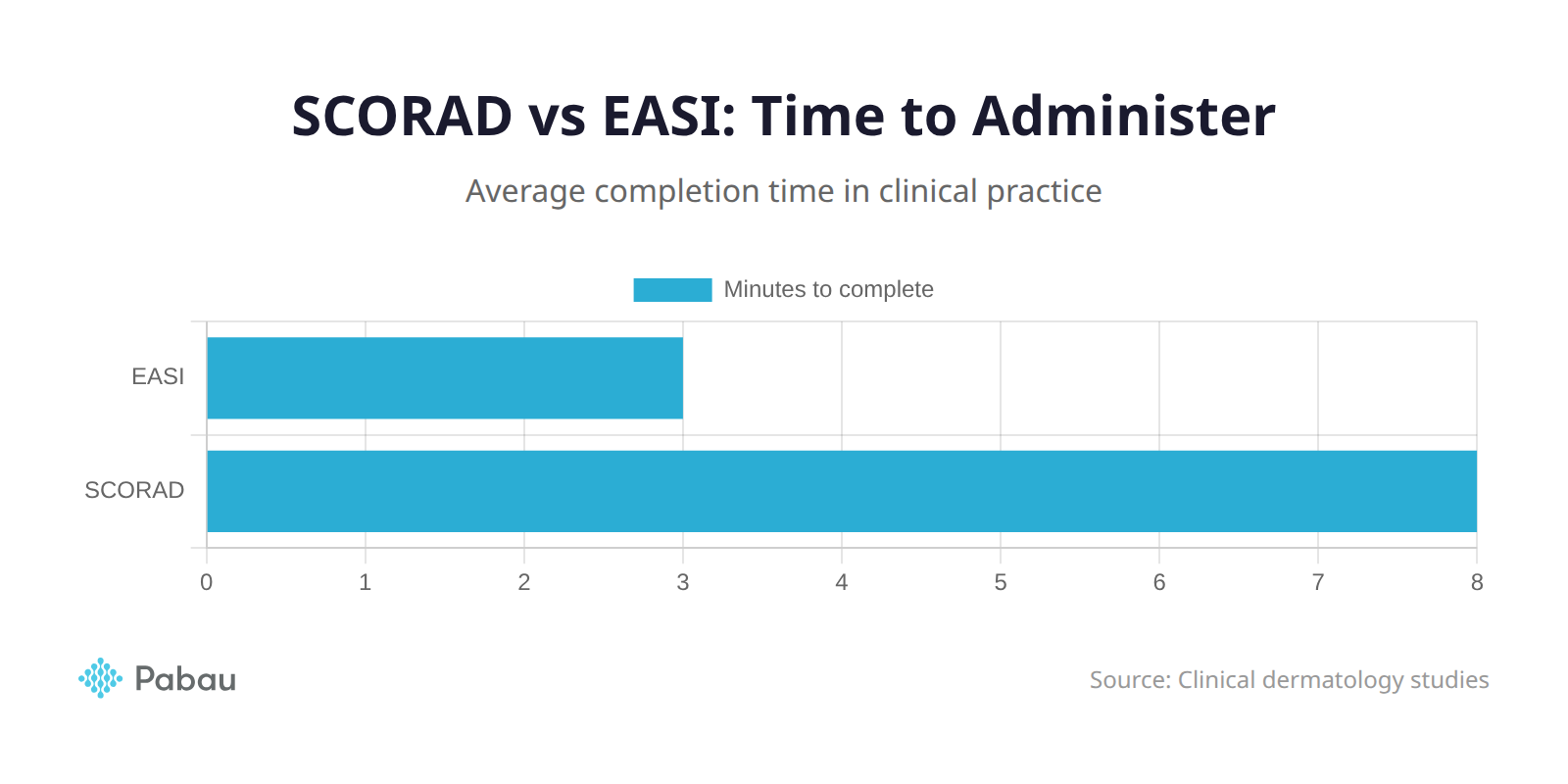
EASI takes 3-5 minutes to complete while SCORAD requires 8-10 minutes per assessment
EASI is the HOME initiative’s recommended core outcome measure for clinical trials
SCORAD captures patient-reported symptoms (itch and sleep loss) that EASI does not
Both tools correlate strongly (r > 0.8) but differ in scoring range and structure
Choose based on your workflow: EASI for speed and objectivity, SCORAD for a fuller clinical picture
Clinicians who manage atopic dermatitis need scoring tools they can trust. Consistent severity measurement drives better treatment decisions, supports insurance documentation, and tracks patient progress over time. However, choosing between the two most widely used instruments can feel overwhelming. This is where the SCORAD vs EASI debate becomes relevant for every dermatology practice.
SCORing Atopic Dermatitis (SCORAD) and the Eczema Area and Severity Index (EASI) both measure disease severity, yet they differ in structure, administration time, and what they capture. SCORAD includes patient-reported symptoms like itch and sleep disturbance. In contrast, EASI focuses purely on clinician-assessed signs. Each tool has strengths that suit different clinical scenarios.
In this guide, you will learn how each scoring system works, where they differ, and which one fits your practice best. We also cover reliability data, clinical trial preferences, and practical tips for integrating these atopic dermatitis scoring tools into your electronic medical records.
What Is SCORAD?
The European Task Force on Atopic Dermatitis developed SCORAD in 1993 as a comprehensive eczema severity assessment tool. It remains one of the most widely used dermatology assessment tools globally, combining clinician observations with patient-reported outcomes in a single composite score.
How SCORAD Works
SCORAD uses a three-part formula: A/5 + 7B/2 + C.
- Part A (Extent): Clinicians map affected skin across eight anatomical regions using the rule of nines. This measures the percentage of body surface area involved (0-100).
- Part B (Intensity): Six clinical signs receive a score from 0 to 3 each. These signs include erythema, oedema/papulation, excoriation, lichenification, oozing/crusting, and dryness. The maximum intensity score is 18.
- Part C (Subjective symptoms): Patients rate their itch and sleep disturbance on visual analogue scales (0-10 each). This section accounts for up to 20 points.
The total SCORAD score ranges from 0 to 103. Severity bands break down as follows: 0-9.9 (clear), 10-28.9 (mild), 29-48.9 (moderate), and 49-103 (severe).
Administration Time and Variants
A full SCORAD assessment typically takes 8-10 minutes. This includes time for patient questionnaires on itch and sleep quality. For settings where patient input is unavailable or unreliable, clinicians can use the objective SCORAD (oSCORAD) variant. The oSCORAD removes Part C entirely, capping the maximum score at 83. As a result, it relies solely on clinician-assessed data while retaining the same extent and intensity measurements.
Furthermore, SCORAD's inclusion of subjective symptoms makes it particularly valuable for chronic disease monitoring. Patients often report symptoms that clinical examination alone cannot capture. For example, nocturnal itch significantly affects quality of life but leaves minimal visible signs during daytime consultations.
What Is EASI?
The Eczema Area and Severity Index was developed by Hanifin et al. (2001) and has since become the preferred EASI score calculator for clinical trials worldwide. The Harmonising Outcome Measures for Eczema (HOME) initiative formally endorsed EASI as the core outcome instrument for atopic dermatitis research.
How EASI Works
EASI evaluates four clinical signs across four body regions. The clinical signs are erythema, oedema/papulation, excoriation, and lichenification. Each sign receives a severity score from 0 (absent) to 3 (severe) in each body region.
The four body regions and their area weightings are:
- Head and neck (10% of body surface area, multiplier 0.1)
- Trunk (30%, multiplier 0.3)
- Upper limbs (20%, multiplier 0.2)
- Lower limbs (40%, multiplier 0.4)
The total EASI score ranges from 0 to 72. Severity bands offer more granularity than SCORAD: 0 (clear), 0.1-1.0 (almost clear), 1.1-7.0 (mild), 7.1-21.0 (moderate), 21.1-50.0 (severe), and 50.1-72.0 (very severe).
Key Characteristics
EASI is purely objective. It does not include patient-reported outcomes such as itch or sleep disturbance. This design choice makes it faster to administer, typically taking just 3-5 minutes per assessment. Similarly, the absence of subjective components eliminates variability introduced by patient mood, recall bias, or language barriers.
The HOME initiative's endorsement of EASI as a core outcome measure has driven widespread adoption in clinical trials since the 2010s. In addition, regulatory bodies including the FDA and EMA accept EASI-based endpoints for drug approval submissions. This makes EASI familiarity essential for practices involved in dermatology research.
Pro Tip
Train your team on EASI first if your clinic participates in clinical trials. Most trial protocols now require EASI as a primary endpoint, and consistent scoring across staff members reduces data variability.
SCORAD vs EASI: Key Differences
Understanding the differences between these atopic dermatitis scoring tools helps you choose the right one for your workflow. The table below summarises the core distinctions.
| Feature | SCORAD | EASI |
|---|---|---|
| Year developed | 1993 | 2001 |
| Score range | 0-103 | 0-72 |
| Clinical signs assessed | 6 | 4 |
| Body regions | 8 (rule of nines) | 4 |
| Patient-reported symptoms | Yes (itch + sleep loss) | No |
| Administration time | 8-10 minutes | 3-5 minutes |
| Objective variant | oSCORAD (score 0-83) | Inherently objective |
| HOME endorsed | No | Yes (core outcome) |
| Severity bands | 4 (clear to severe) | 6 (clear to very severe) |
Narrative Comparison
When comparing SCORAD vs EASI, the most significant difference lies in subjectivity. SCORAD's Part C captures what patients feel, not just what clinicians see. This gives a more holistic view of disease burden. On the other hand, EASI's purely objective approach reduces scorer bias and speeds up the assessment process.
Administration time is another practical consideration. In a busy dermatology clinic seeing 20-30 patients per day, saving 5 minutes per assessment adds up quickly. EASI's streamlined four-region, four-sign approach makes it ideal for high-volume settings.
Additionally, SCORAD assesses two signs that EASI does not: oozing/crusting and dryness. These signs can be clinically relevant in certain presentations. Therefore, SCORAD may provide a more complete picture of acute flares where oozing is prominent.
The severity band structure also differs. EASI's six-level classification offers finer discrimination at the lower end of the scale. This is particularly useful for tracking patients who are approaching clearance, where distinguishing "almost clear" from "mild" informs treatment tapering decisions.
Reliability and Validity: Which Score Is More Accurate?
The SCORAD vs EASI debate extends to reliability data. Both scoring systems demonstrate strong psychometric properties. However, their reliability profiles differ depending on the measurement context. Understanding these differences helps you pick the right tool for your specific use case.
Inter-Rater Reliability
Inter-rater reliability measures how consistently different clinicians score the same patient. Studies show that oSCORAD achieves slightly higher inter-rater reliability than standard SCORAD. This makes sense because removing subjective symptoms eliminates a source of variability. EASI also performs well in inter-rater studies, though oSCORAD edges ahead in most head-to-head comparisons.
For practices where multiple clinicians assess the same patient across visits, oSCORAD offers the most consistent results. Consequently, multi-provider dermatology clinics may prefer oSCORAD for longitudinal tracking.
Intra-Rater Reliability
Intra-rater reliability measures how consistently a single clinician scores the same patient over time. EASI consistently achieves the highest intra-rater reliability scores across published studies. This makes EASI the stronger choice when the same dermatologist follows a patient through their treatment journey.
Minimal Clinically Important Difference
The minimal clinically important difference (MCID) represents the smallest score change that patients perceive as meaningful. For SCORAD, the MCID is 8.7 points. For EASI, it is 6.6 points. These thresholds help clinicians determine whether a treatment is genuinely working rather than producing statistically significant but clinically meaningless improvements.
Correlation Between Tools
Research consistently shows a strong correlation between SCORAD and EASI scores (r > 0.8). This means both tools generally agree on disease severity. Nevertheless, they are not interchangeable because their scales, ranges, and components differ significantly. You cannot simply convert one score to the other using a formula.
“Since switching to Pabau, we have streamlined our clinical documentation and patient tracking. The digital forms and measurements tools save us significant time during consultations, allowing us to focus on what matters most: patient care.”
Clinical Trial Use: Which Tool Do Researchers Prefer?
When examining SCORAD vs EASI in research settings, the landscape has shifted significantly in favour of EASI over the past decade. Understanding these clinical trial scoring methods helps practices that participate in or reference trial data.
HOME Initiative Recommendation
The Harmonising Outcome Measures for Eczema (HOME) initiative conducted a rigorous consensus process to standardise outcome reporting in atopic dermatitis research. In 2014, HOME recommended EASI as the core outcome instrument for measuring clinical signs in trials. This recommendation carried significant weight because HOME involved patients, clinicians, researchers, and regulators from over 40 countries.
As a result, most major clinical trials launched after 2015 use EASI as their primary or co-primary endpoint. The EASI-75 response rate (the percentage of patients achieving at least 75% improvement) has become the standard efficacy benchmark for new biologics and JAK inhibitors.
Regulatory Acceptance
Both the FDA and EMA accept SCORAD and EASI as valid endpoints in regulatory submissions. However, EASI's HOME endorsement gives it a practical advantage. Sponsors designing pivotal trials increasingly default to EASI to align with international consensus. Furthermore, using EASI simplifies cross-trial comparisons, which regulators value when assessing relative efficacy.
Trends in Published Research
A review of published atopic dermatitis trials shows a clear trend. Before 2010, SCORAD appeared more frequently in European studies while EASI dominated North American and Asian research. Since the HOME recommendation, EASI has become the dominant tool globally. Studies published by Schmitt et al. (2014) in the British Journal of Dermatology were instrumental in building the evidence base for this shift.
Pro Tip
When reviewing trial results for treatment decisions, check whether the study used EASI-50, EASI-75, or EASI-90 as endpoints. Higher thresholds indicate more stringent efficacy criteria and help you set realistic expectations with patients.
Which Tool Should You Use in Clinical Practice?
The best scoring tool depends on your clinical context, patient volume, and workflow needs. Here is a practical framework for deciding between SCORAD vs EASI in everyday practice.
When to Use SCORAD
Choose SCORAD when patient-reported symptoms are central to your treatment decisions. Itch severity and sleep disturbance directly influence quality of life and often guide therapeutic escalation. For chronic cases requiring long-term monitoring, the subjective component provides insights that clinical examination alone may miss.
SCORAD also fits practices where 8-10 minutes per assessment is feasible. Smaller dermatology clinics with longer appointment slots can leverage the richer data SCORAD provides. Additionally, if your electronic medical records system already integrates SCORAD templates, switching tools may introduce unnecessary disruption.
When to Use EASI
EASI excels in high-volume settings where efficiency matters. A 3-5 minute assessment time means your team can score more patients without extending clinic hours. For practices involved in clinical trials, EASI is essentially mandatory given the HOME recommendation.
Choose EASI when you need purely objective tracking. This is particularly valuable when multiple clinicians assess the same patients, as EASI reduces inter-rater variability. In addition, EASI's finer severity bands help track incremental improvement in patients responding to treatment.
Using Both Tools
Some research-oriented practices use both tools simultaneously. SCORAD captures the patient perspective while EASI provides the objective benchmark. This dual approach adds assessment time but generates the most comprehensive dataset. For most clinical settings, however, one tool is sufficient.
EMR Integration
Whichever tool you select, building it into your digital forms and workflows saves time and reduces errors. Pabau's custom form builder lets you create SCORAD or EASI scoring templates that auto-calculate totals. Combined with measurements tracking, you can graph severity scores over time and share visual progress reports with patients.
How Pabau Supports Atopic Dermatitis Management
Managing atopic dermatitis effectively requires more than a scoring tool. You need a system that connects assessments to treatment plans, tracks progress, and keeps documentation audit-ready.
Pabau's digital forms let you build custom SCORAD and EASI calculators that match your clinical workflow. Score fields auto-populate severity bands, reducing manual calculation errors. These forms integrate directly with each patient's client record, creating a unified longitudinal profile.
For visual tracking, measurements tracking plots severity scores on graphs over weeks and months. This makes treatment response immediately visible during consultations. Patients respond well to seeing their progress charted, which supports compliance documentation and shared decision-making.
Before and after photos add another dimension to atopic dermatitis documentation. Clinical photographs taken at each visit provide objective visual evidence that complements numerical scores. Similarly, automated workflows can trigger follow-up assessments at set intervals, so no patient falls through the cracks.
For practices capturing patient-reported outcomes alongside SCORAD, Pabau's forms can collect itch and sleep data digitally before the consultation starts. This saves chair time and ensures subjective data is recorded consistently. Your clinic dashboard then provides a real-time overview of patient severity distribution across your caseload.
Expert Picks
Need better clinical documentation workflows? Learn how writing faster, safer clinical notes improves patient outcomes and reduces admin time.
Want to track patient progress visually? See how skin assessment tools integrate with your clinical workflow for better dermatology outcomes.
Looking to streamline your consultation process? Discover tips for performing consultations that convert while maintaining clinical rigour.
FAQs
No direct conversion formula exists between SCORAD and EASI. Although the two scores correlate strongly (r > 0.8), they measure different components and use different scales. SCORAD includes patient-reported symptoms that EASI does not capture, making mathematical conversion unreliable.
Neither tool is inherently more accurate. EASI achieves higher intra-rater reliability, meaning a single clinician scores more consistently over time. However, oSCORAD shows slightly better inter-rater reliability across different assessors. Your choice depends on whether consistency within one rater or across multiple raters matters more.
Most clinicians can learn EASI in a single training session of 30-60 minutes. SCORAD takes slightly longer because it involves more clinical signs, the rule of nines for body surface area, and patient-reported symptom scales. Both tools have freely available training resources online from their respective development groups.
Both SCORAD and EASI are validated for paediatric use. However, SCORAD’s patient-reported symptom component may need parent proxy reporting for young children, which can introduce bias. EASI’s purely objective approach avoids this issue, making it slightly more practical for paediatric assessments.
No universal requirement exists. Both the FDA and EMA accept SCORAD and EASI in regulatory submissions. Some biologic prescribing criteria reference specific EASI or SCORAD thresholds for treatment eligibility. Check your local formulary guidelines, as requirements vary by region and insurer.
Both tools track treatment response effectively but do not predict it in advance. Baseline severity scores help set expectations, and serial measurements show whether a treatment is working. The MCID values (SCORAD 8.7, EASI 6.6) help determine whether observed improvements are clinically meaningful.