Key Takeaways
A structured return to running protocol physical therapy programme reduces re-injury rates by up to 50%
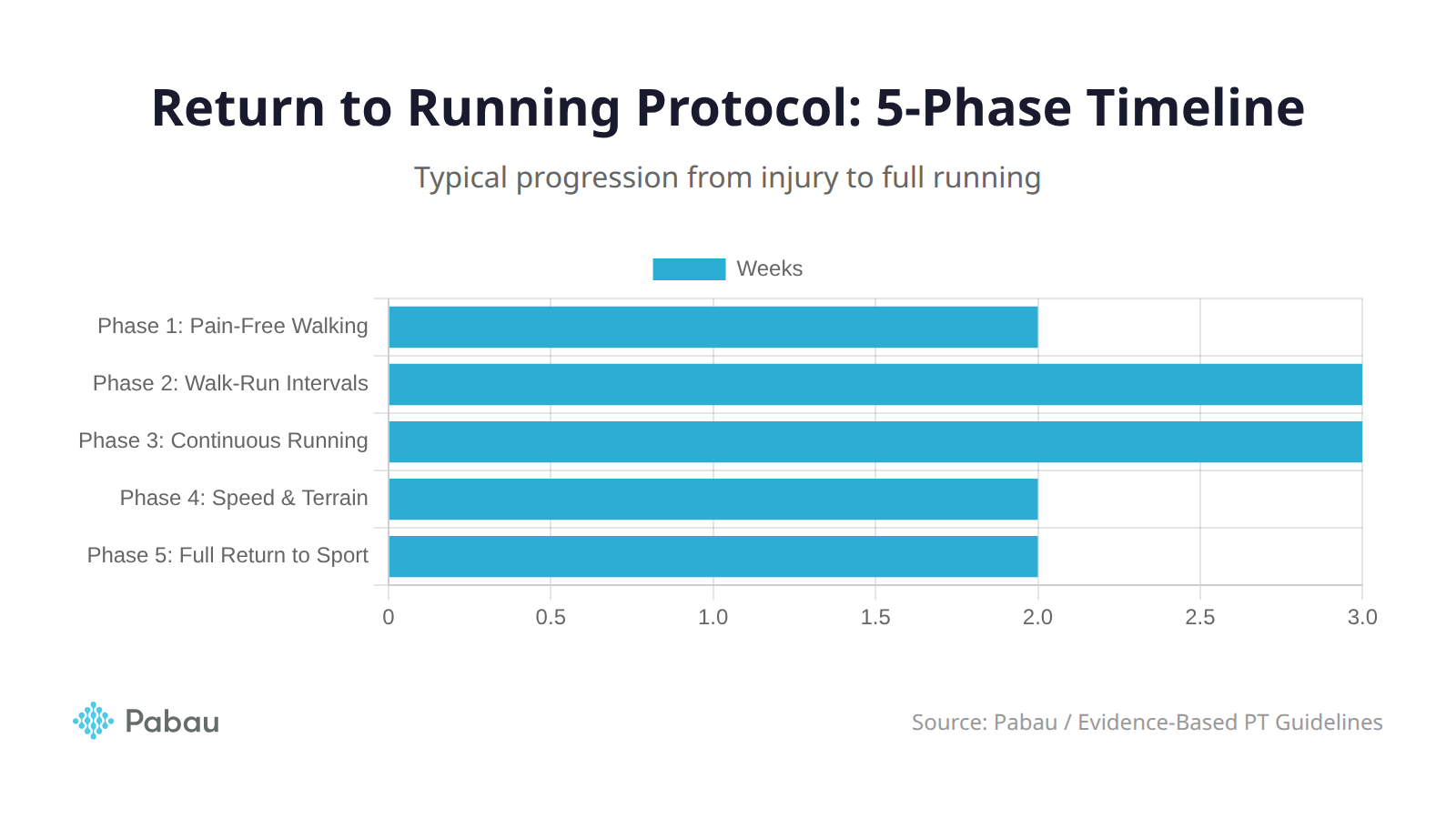
Five progressive phases move patients from pain-free walking through walk-run intervals to full sport return
Objective criteria such as single-leg hop symmetry and pain-free gait must be met before advancing each phase
Run-walk intervals are the safest bridge between rehabilitation exercises and continuous running
Tracking session data and pain scores in clinic software keeps the protocol accountable and measurable
Every year, roughly 50% of recreational runners experience an injury that forces them to stop training. For physical therapists, the challenge is not just healing the injury but getting that runner back on the road safely. A return to running protocol physical therapy programme provides the structured, criteria-driven framework clinicians need to bridge the gap between rehabilitation and full activity.
In this guide, you will learn exactly how to design, implement, and progress a return to running protocol in your physical therapy practice. From readiness screening to the final phase of unrestricted training, each step is backed by current evidence and practical clinical insight.
Why a Return to Running Protocol Physical Therapy Programme Matters
Returning to running too early is one of the most common mistakes in musculoskeletal rehabilitation. Without a structured protocol, patients often resume training based on how they feel rather than objective clinical markers. This leads to re-injury rates as high as 30% in some lower-limb conditions, according to research published in the British Journal of Sports Medicine.
A return to running protocol physical therapy approach replaces guesswork with measurable milestones. It gives both the clinician and the patient a clear roadmap, reduces anxiety around returning to sport, and provides documentation that supports clinical decision-making.
For clinics using practice management software, these protocols can be templated, tracked, and adjusted within the patient record, improving consistency across your team.
Benefits for Clinicians and Patients
Structured protocols benefit both sides of the therapeutic relationship. Clinicians gain objective progression criteria they can defend in documentation. Patients gain confidence because they understand what comes next and why.
Additionally, a phased approach reduces the psychological burden of returning to sport. Runners who follow a graduated return to running protocol report lower fear-avoidance scores and higher satisfaction with their rehabilitation outcomes.
Pre-Running Readiness Criteria
Before any running begins, the patient must meet baseline readiness criteria. Skipping this step is the most frequent protocol failure in clinical practice.

Minimum Requirements Before Phase 1
The following criteria should be met before a patient enters the walk-run phase:
- Pain-free walking for 30 minutes at a brisk pace without a limp
- Full, pain-free range of motion at the injured joint
- Single-leg balance held for 30 seconds with eyes closed
- At least 80% strength symmetry on manual muscle testing or dynamometry
- No effusion or swelling after 30 minutes of continuous walking
These benchmarks align with guidelines from the American Physical Therapy Association (APTA) and represent the minimum threshold for safe progression.
Pro Tip
Use a simple traffic-light system in your clinic notes: red (not ready), amber (close but needs 1-2 more sessions), green (cleared for Phase 1). It speeds up team communication and keeps everyone aligned.
Phase 1: Pain-Free Walking and Baseline Conditioning
Phase 1 is not about running at all. It focuses on building the aerobic base and tissue tolerance needed to handle the impact forces of running, which can reach 2.5 times body weight per stride.
During this phase, patients perform 20 to 30 minutes of brisk walking three to four times per week. Alongside walking, the programme includes targeted strengthening for the gluteals, quadriceps, and calf complex, as well as neuromuscular control exercises.
Key Exercises in Phase 1
- Bodyweight squats and single-leg squats progressing to weighted variations
- Calf raises (bilateral progressing to single-leg, flat surface to step)
- Side-lying hip abduction and clamshells with resistance bands
- Single-leg Romanian deadlifts for posterior chain activation
- Balance board or wobble cushion drills for proprioception
Progression criteria to Phase 2: the patient must walk briskly for 30 minutes on consecutive days with zero pain and zero swelling.
Phase 2: Walk-Run Intervals in Your Return to Running Protocol
This is the critical transition phase in any return to running protocol physical therapy programme. Walk-run intervals introduce controlled impact loading while allowing recovery between bouts.
A typical starting point is one minute of running followed by four minutes of walking, repeated for 20 to 30 minutes. Over the course of two to three weeks, the ratio shifts gradually until the patient reaches five minutes of running with one minute of walking rest.
Sample Week-by-Week Progression
| Week | Run | Walk | Total Time | Sessions per Week |
|---|---|---|---|---|
| 1 | 1 min | 4 min | 20 min | 3 |
| 2 | 2 min | 3 min | 25 min | 3 |
| 3 | 3 min | 2 min | 25 min | 3-4 |
| 4 | 5 min | 1 min | 30 min | 3-4 |
Each session should be performed on flat, even surfaces. The patient must have at least one rest day between running sessions.
Monitoring Symptoms During Walk-Run Intervals
Patients should rate their pain on a 0 to 10 visual analogue scale (VAS) before, during, and 24 hours after each session. The acceptable threshold is a maximum pain score of 2 out of 10 during the run that returns to baseline within 24 hours. Any score above 3 during running or persistent next-day symptoms means the patient should repeat the previous week's protocol.
Pro Tip
Have patients log each session in a shared digital form. Tracking run duration, pain scores, and perceived exertion in your clinic software creates an objective record you can review at each appointment.
Phase 3: Continuous Running
Once the patient completes 30 minutes of five-minutes-on, one-minute-off intervals without symptoms, they are ready for continuous running. However, this does not mean returning to pre-injury distances overnight.
Start with 15 to 20 minutes of continuous easy-pace running. Increase by no more than 10% per week, following the well-established 10% rule for mileage progression. In most cases, patients reach 30 minutes of continuous running within two to three weeks of entering this phase.
Common Mistakes in Phase 3
Several errors commonly derail progress during this phase. Running too fast is the most frequent problem, as patients confuse feeling good with being ready for tempo runs. Similarly, adding hills or trails before the protocol permits introduces biomechanical stress the tissues may not yet tolerate.
Furthermore, skipping the strengthening programme is a risk. The Journal of Orthopaedic and Sports Physical Therapy (JOSPT) consistently highlights that concurrent strength training reduces running-related injury recurrence by 30 to 50%.
Phase 4: Speed, Terrain, and Sport-Specific Drills
Phase 4 is where the return to running protocol physical therapy programme begins to look like actual training again. This phase introduces tempo runs, hill repeats, and sport-specific agility drills.
Progression in Phase 4
- Week 1-2: Add gentle inclines and declines to the route
- Week 3-4: Introduce tempo intervals (80% perceived effort for 2 to 5 minutes)
- Week 5-6: Include lateral movement drills, cutting, and change-of-direction work if the patient's sport requires it
For distance runners, this phase also includes longer runs at conversational pace, building toward 75% of pre-injury weekly mileage. For field sport athletes, agility ladders, shuttle runs, and sport-specific movement patterns are integrated.
Objective Benchmarks for Phase 4 Clearance
Before advancing to Phase 5, the patient should demonstrate:
- Single-leg hop for distance within 90% of the uninjured side
- Y-balance test composite score within 4 cm of the uninjured limb
- Ability to complete 30 minutes of continuous running at moderate intensity without symptoms
- Completion of three consecutive sport-specific training sessions with no pain or swelling
“Since implementing structured rehabilitation protocols in Pabau, our physiotherapy team has cut re-injury rates significantly. The ability to template treatment plans and track patient progress digitally means every clinician follows the same evidence-based pathway.”

Phase 5: Full Return to Running and Maintenance
The final phase of a return to running protocol physical therapy programme is unrestricted return to training. At this point, the patient has met all objective benchmarks, completed graduated loading, and demonstrated consistent symptom-free performance across multiple sessions.
However, the work does not stop here. A maintenance programme should continue for at least eight weeks after full clearance to consolidate tissue adaptation and prevent deconditioning of the stabilising muscles.
Maintenance Programme Essentials
- Continue strength training two to three times per week (hip, knee, and ankle focused)
- Perform single-leg balance and proprioception drills before each run as a warm-up
- Follow the 10% weekly mileage increase rule for at least the first two months
- Schedule a follow-up appointment at four and eight weeks post-clearance
Clinics that use automated workflows can set reminders for these follow-ups, ensuring patients do not fall through the gaps during the critical maintenance window.
How to Document a Return to Running Protocol in Your Clinic
Clear documentation protects both the clinician and the patient. Each session should record the phase, the specific walk-run or run parameters used, pain scores, and any deviations from the protocol.
Building a Protocol Template
For practices using electronic health records, building a digital form template for the return to running protocol saves time and standardises data collection. Key fields to include are:
- Current phase and week number
- Session parameters (duration, run-walk ratio, pace)
- Pre-session and post-session VAS pain score
- Functional test results (hop test, Y-balance)
- Clinician notes and next-session plan
This level of documentation also supports measurements tracking over time, giving you a visual record of each patient's recovery trajectory.
Keeping Patients on Schedule
Appointment scheduling workflows matter for protocol success. Return to running progressions require regular check-ins at phase transitions. Automated reminders reduce no-shows and keep patients engaged throughout their rehabilitation journey.
For clinics managing large patient volumes, going paperless with digital assessment forms eliminates manual filing whilst ensuring instant access to historical data during patient encounters.
Adapting the Protocol for Different Injuries
Not every patient follows the same timeline. The return to running protocol physical therapy approach should be adapted based on the specific injury, surgical history, and individual patient factors.
Injury-Specific Considerations
Achilles tendinopathy: Progress more slowly through Phase 2, adding eccentric calf loading exercises. Allow up to four weeks in the walk-run phase.
ACL reconstruction: Typically, running is not introduced until at least four to five months post-surgery, pending surgeon clearance and quadriceps strength index above 80%.
Stress fractures: Require complete bony healing (confirmed via imaging) before entering Phase 1. Bone stress injuries have the highest re-injury risk when protocols are rushed.
Patellofemoral pain syndrome: Focus heavily on hip and quadriceps strengthening in Phase 1. Many patients with this condition can enter walk-run intervals earlier but need more time in Phase 4 due to hill and stair sensitivity.
For clinics managing multiple injury types, storing these adaptations in a client record system ensures continuity of care across therapists.
Common Reasons Return to Running Protocols Fail
Even well-designed protocols can break down in practice. Understanding the common pitfalls helps you avoid them.
Insufficient patient education: Patients who do not understand why each phase matters are more likely to skip steps. Take two minutes at the first session to explain the rationale behind graduated loading.
Lack of objective criteria: Advancing phases based on time alone ignores individual variation. Always use measurable benchmarks rather than calendar dates.
Poor compliance tracking: If you cannot see whether a patient completed their home sessions, you cannot make informed progression decisions. A patient portal where patients log their sessions between appointments solves this problem.
Ignoring psychosocial factors: Fear of re-injury is a significant barrier to returning to sport. Screen for kinesiophobia using the Tampa Scale and address it through graded exposure and education.
Pro Tip
Schedule a 15-minute ‘running readiness review’ before Phase 2 begins. Use it to reassess strength, review home exercise compliance, and address any psychological barriers. This single checkpoint prevents most protocol failures.
Using Technology to Manage Return to Running Protocols
Modern physiotherapy clinic management software makes it significantly easier to implement structured protocols across a multi-therapist clinic.
With the right system, you can template the five-phase protocol, assign it to a patient at intake, and track progress automatically. Shared digital records ensure any therapist in the clinic can pick up where the last session left off.
For clinics that offer online booking, patients can self-schedule their Phase 2 to 5 follow-ups based on the intervals the protocol requires, reducing administrative burden on reception staff.
Expert Picks
Setting up a physiotherapy clinic? Read our guide on how to open a physiotherapy clinic covering licensing, equipment, and software.
Need to ensure regulatory compliance? Our breakdown of mandatory compliance for physiotherapy clinics covers everything from GDPR to clinical governance.
Looking for clinic requirements in the US? Check our guide to physical therapy clinic requirements in Arizona for state-specific regulations.
Frequently Asked Questions
A return to running protocol physical therapy programme is a structured, phased plan that guides patients from injury recovery through graduated walking, walk-run intervals, and continuous running back to full sport participation. Each phase has objective criteria that must be met before progression.
Patients can begin walk-run intervals once they can walk briskly for 30 minutes without pain, limping, or swelling. They should also have at least 80% strength symmetry and full range of motion at the affected joint. Your physical therapist will confirm readiness using objective clinical tests.
Most return to running protocols take 8 to 12 weeks from the start of Phase 1 walking to full unrestricted running. However, the timeline varies significantly based on injury type, surgical history, and individual healing rates. ACL reconstruction protocols may take 4 to 6 months before running begins.
The 10% rule states that weekly running mileage should increase by no more than 10% from one week to the next. This guideline helps prevent overloading healing tissues and is widely recommended by sports medicine professionals as a safe progression strategy during return to running programmes.
Yes, return to running protocols are essential after ACL reconstruction. However, running typically does not begin until 4 to 5 months post-surgery, pending surgeon clearance and quadriceps strength index above 80%. The walk-run phase may also be extended to allow additional tissue adaptation.
Physical therapists track progress using pain scores (VAS), functional tests like the single-leg hop test and Y-balance test, and session logs recording run duration and walk-run ratios. Many clinics now use digital clinical forms and practice management software to automate tracking and ensure consistency across the care team.
Take the Next Step
A well-structured return to running protocol physical therapy programme transforms how your clinic manages running injuries. By following evidence-based phases, tracking objective criteria, and using digital tools to maintain consistency, you give every patient the best possible chance of returning to sport safely.









