Key Takeaways
An EHR for multi-franchise mental health practice needs centralized admin controls with location-level autonomy, not just a shared login.
Consolidated billing across sites is the #1 operational challenge franchise owners report when scaling past three locations.
42 CFR Part 2 compliance for substance use disorder records requires data segregation that many standard EHRs cannot enforce at the franchise level.
Pabau’s multi-location dashboard and unified client records support behavioral health franchises scaling across sites without separate software instances.
Most behavioral health franchise owners discover the limits of their EHR around location number three. Claims start routing to the wrong provider. Therapists at different sites can’t access shared client histories. Compliance documentation that works fine for one state creates problems in another. The software that served a single location well becomes an operational liability at scale.
Choosing an EHR for multi-franchise mental health practice is not the same decision as choosing an EHR for a solo therapist or even a single group practice. This guide covers what franchise owners and administrators need to evaluate: centralized oversight, location-level autonomy, multi-provider scheduling, consolidated billing, and compliance architecture that works across sites.
What the Software Must Actually Do
The term “multi-location support” appears in nearly every EHR marketing page. What it actually means varies enormously. For a franchise owner overseeing five or more behavioral health sites, the practical requirements are specific.
You need a single login that gives you visibility across all locations without exposing location-specific clinical data to the wrong providers. You need billing that aggregates across sites for ownership reporting while still generating location-level invoices for payers. You need scheduling that accounts for therapists who work across multiple locations in the same week. And you need clinical documentation templates that are standardized at the franchise level but editable at the location level for state-specific requirements.
According to the American Psychiatric Association’s EHR guidance, much of healthcare policy surrounding electronic records is concerned with connecting multiple providers across practices to share patient health information. For franchise models, this interoperability requirement is not optional. It is the architecture on which every other operational decision rests.
- Centralized admin dashboard: Franchise owners need performance data across all sites from a single interface, not separate logins per location.
- Role-based access control: Clinicians at Location A should not have default access to client records at Location B. Permissions must be granular.
- Unified client records: A client who receives services at multiple franchise locations needs a single longitudinal record, not duplicate charts.
- Location-specific settings: Fee schedules, intake forms, and compliance workflows may differ by state. The EHR must accommodate this without requiring a separate software instance.
- Multi-provider scheduling: Therapists, psychiatrists, and support staff across sites need calendar visibility that respects location-specific booking rules.
Where Most Multi-Location Mental Health Platforms Fall Short
The operational challenges of multi-location practice management follow a predictable pattern. The EHR was built for solo or small-group practices and stretched to accommodate expansion. The result is usually one of three failure modes.
Siloed billing: Each location bills as a separate entity within the software, preventing franchise-wide revenue reporting. Owners can’t see aggregate claim status, denial rates by location, or cross-site payer performance without manually exporting and combining data.
Flat permission structures: The EHR offers two roles: admin and clinician. A franchise model requires at minimum four levels: franchise owner, location manager, licensed clinician, and support staff. Without this hierarchy, either privacy is compromised or administrative access is unnecessarily restricted.
Template rigidity: Documentation templates are set at the system level with no location-specific overrides. A franchise operating in both California and Texas, for example, may need different intake disclosures, different informed consent language, and different progress note requirements. A rigid template system forces manual workarounds that increase documentation errors.
These are not minor inconveniences. They represent material compliance and revenue risks for practices with three or more locations.
The Five Capabilities That Separate Enterprise-Ready EHRs
When evaluating a behavioral health EHR for franchise use, move past feature checklists and test these five capabilities in a demo environment with your actual multi-site workflows.
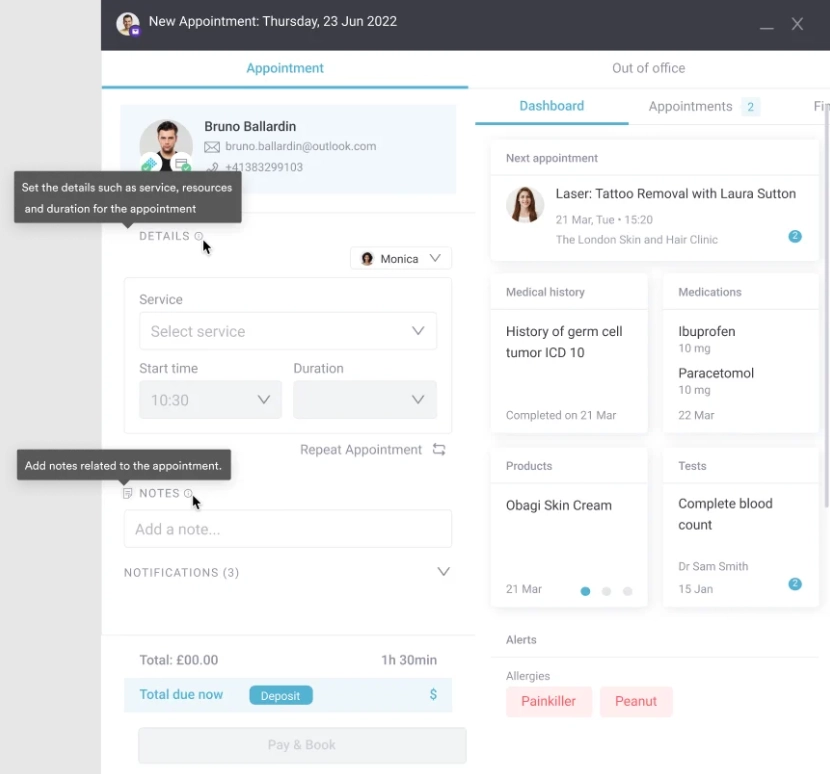
1. Multi-location scheduling with provider visibility across sites. A therapist who splits their week between two locations needs a calendar that reflects availability at both sites without double-booking. The EHR should support cross-location calendar management for individual providers, not just per-location appointment books. Pabau’s appointment scheduling supports multi-provider, multi-location calendar management within a single practice instance.
2. Outcome measurement tool integration. PHQ-9, GAD-7, and similar validated screening instruments should be administered digitally, scored automatically, and stored in the client record. For franchises, these tools need to be deployable at the location level while feeding into franchise-wide outcome reporting. This capability is often listed but rarely implemented cleanly in general-purpose EHRs. Digital forms with automated scoring are what separates this from a paper process pasted into a PDF upload.
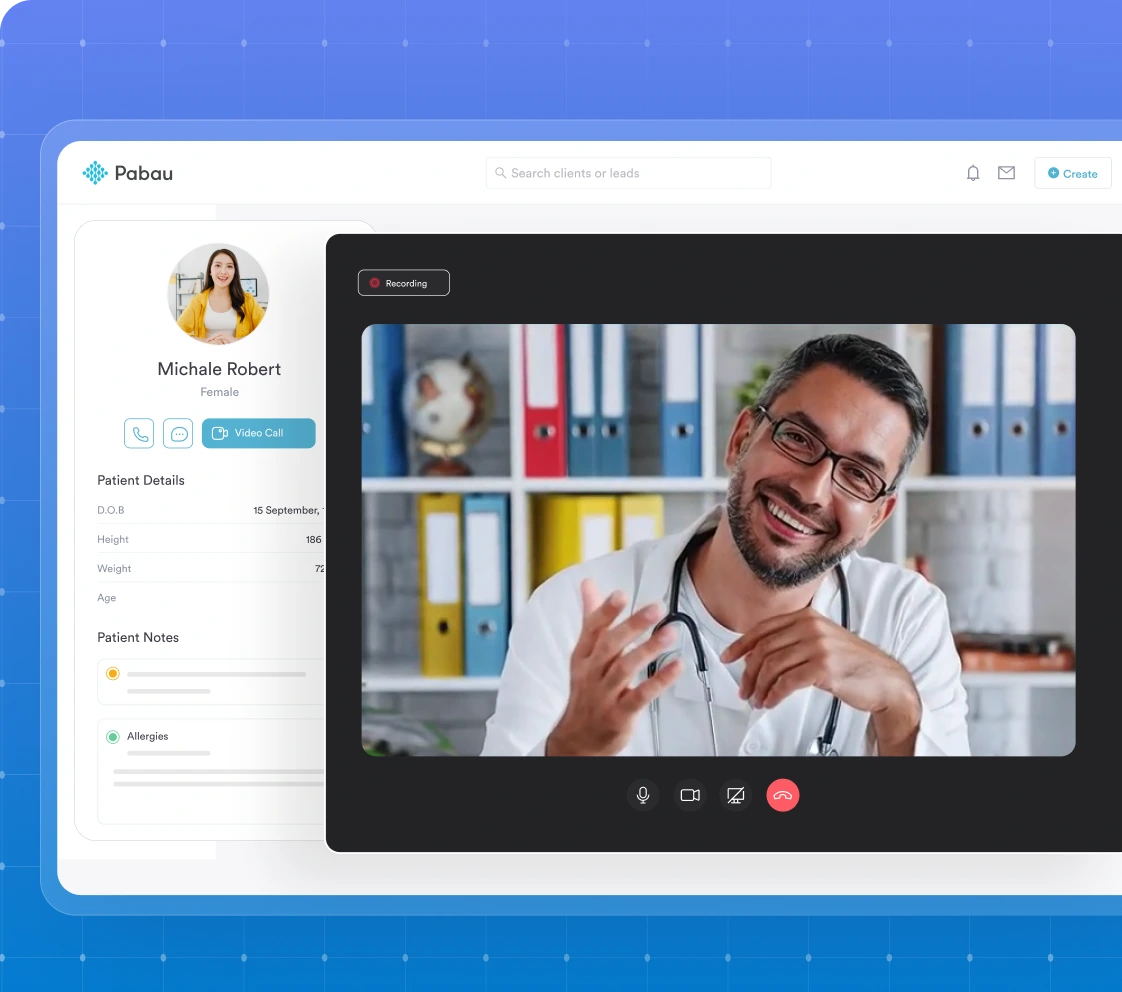
3. Telehealth integration without a third-party add-on. For franchises operating across state lines, telehealth is not optional. Requiring therapists to use a separate video platform that doesn’t connect to the scheduling system or clinical record creates documentation gaps. The EHR should handle telehealth scheduling, session delivery, and note completion in one workflow.
4. Franchise-wide reporting and KPI dashboards. Owners need to benchmark location performance against each other. Appointment capacity utilization, no-show rates, average sessions per client, and revenue per provider are the metrics that drive operational decisions. The clinic dashboard must support this level of aggregation, not just location-level snapshots.
5. Onboarding architecture for new locations. Adding a fourth or fifth franchise location should not require rebuilding the EHR configuration from scratch. Templates, workflows, permission structures, and payer setups should be cloneable from an existing location with only the state-specific adjustments needed.
| Capability | What to Test in Demo | Common Gap |
|---|---|---|
| Multi-site scheduling | Can a single provider appear in calendars at two locations without duplicate setup? | Separate calendar instances per location |
| Outcome tool integration | Does PHQ-9 auto-score and attach to the session note? | Manual scoring, separate PDF upload |
| Telehealth workflow | Does scheduling a telehealth session auto-generate a video link and attach to the note? | Third-party video platform, manual link sharing |
| Franchise reporting | Can you see revenue and utilization across all locations in one dashboard view? | Export-and-combine manual reporting |
| Location onboarding | Can you clone a location template for a new site? | Full reconfiguration required for each new location |
Consolidated Billing Across Multiple Locations
Billing is where multi-franchise EHR limitations become revenue problems. A franchise with five locations and 40 providers may submit several hundred claims per week. Without consolidated billing architecture, each location operates as a standalone billing entity. Owners can’t see which locations have claim backlogs, which payers are generating the most denials, or whether specific procedure codes are being underbilled.
The claims management workflow in an enterprise-ready EHR needs to support multi-location aggregation while maintaining location-specific billing profiles. Each location may have different tax IDs, different credentialed providers, and different in-network payer agreements. The system must track this without collapsing everything into a single undifferentiated billing queue.
For franchises with mixed revenue models, including private-pay, insurance billing, and employee assistance program (EAP) contracts, the billing layer needs to handle each payment type at the location level while rolling up to franchise-wide financial reporting. This is where many behavioral health EHRs designed for small practices reach their architectural limits.
Reviewing financial management practices for multi-location franchises consistently highlights one theme: the cost of billing fragmentation compounds as you scale. A denial rate of 8% on 200 weekly claims becomes materially different from the same denial rate on 800 weekly claims across four locations.
See how Pabau supports multi-franchise behavioral health billing
Pabau's multi-location platform gives franchise owners consolidated financial reporting, location-specific billing profiles, and integrated claims management across all sites from one dashboard.

Multi-State Compliance and HIPAA Data Architecture
A franchise operating across state lines faces a compliance layer that single-location practices never encounter. Telehealth regulations vary significantly by state. Clinician licensing requirements differ. And for franchises that treat substance use disorders, 42 CFR Part 2 confidentiality requirements impose data segregation rules that go beyond standard HIPAA protections. SAMHSA’s Final Rule effective April 2024 aligned 42 CFR Part 2 more closely with HIPAA – particularly by allowing a single patient consent to cover treatment, payment, and healthcare operations (TPO) disclosures, rather than the previous per-disclosure consent model – but Part 2 still imposes stricter requirements than HIPAA for disclosures outside TPO and for use of records in civil, criminal, or administrative proceedings, and the EHR must enforce those distinctions at the technical level.
HIPAA Business Associate Agreements (BAAs) for multi-entity franchise structures are more complex than single-location BAAs. Each franchise entity may need its own BAA with the EHR vendor. The software must be able to enforce data access controls that reflect these legal structures, not just treat all locations as branches of a single entity.
Compliance management workflows in a multi-site EHR should include: location-specific consent form versioning, audit trails that track who accessed which client records across which locations, automated HIPAA-required notification workflows, and configurable data retention policies by location or by state requirement. Reviewing HIPAA compliance requirements for clinic software makes clear that the technical safeguards required under HIPAA’s Security Rule apply at the covered entity level. A franchise is not a single covered entity simply because it uses the same EHR.
For franchises considering expansion into states with stronger medical privacy or mental health statutes – such as California’s Confidentiality of Medical Information Act (CMIA), which applies broader protections to medical information than HIPAA, or jurisdictions with mental health-specific confidentiality protections including New York’s Mental Hygiene Law and similar statutes in other states – the EHR’s data architecture needs to support state-specific data handling without requiring a separate software instance for each jurisdiction.
Pro Tip
Audit your EHR’s BAA before signing. Ask the vendor specifically whether the BAA covers all franchise entities or only the primary contracting entity. Many standard BAAs are written for single-location practices and require amendment for multi-entity franchise structures. Get the amended language in writing before onboarding.
How to Evaluate an EHR for Multi-Franchise Mental Health Practice
The evaluation process for an ehr for multi-franchise mental health practice should mirror the operational structure you are building, not the one you currently have. Practices that select an EHR based on their current two locations and then try to adapt it for their fifth location pay for that decision in implementation costs and lost productivity.
Run your RFP process using these four evaluation phases:
- Architecture review: Ask how the software handles multi-entity BAAs, role-based access hierarchies, and location-specific configuration. Request a demo with your actual org structure (franchise owner, location managers, clinicians, admin staff) configured in the system.
- Billing stress test: Submit test claims for two different locations with different tax IDs and different payer agreements. Verify the system routes each correctly and generates separate EOBs while also producing a consolidated financial report.
- Compliance scenario walkthrough: Walk through a 42 CFR Part 2 scenario if your franchise treats any substance use disorders. Ask specifically how the system segregates these records and what prevents unauthorized cross-location access.
- Scalability simulation: Ask the vendor to add a third demo location to your test environment and document how long it takes and what configuration is required. This predicts your real onboarding cost for each new franchise location.
Pabau’s multi-location feature set supports centralized admin controls, location-specific settings, and a unified dashboard for owners overseeing multiple sites. For franchises that also need to standardize clinical documentation across locations, the franchise management solutions framework applies directly to behavioral health multi-site operations.
The key software features for multi-location practice management consistently point to the same priority: a single source of truth for clinical and financial data that can be viewed at any level of the org chart without losing location-specific context.
Expert Picks
Need a structured psychiatric documentation framework? Psychiatric Evaluation Template provides a step-by-step guide for comprehensive mental health assessments compatible with multi-site documentation standards.
Managing a multi-location behavioral health practice? Mental Health EMR Software covers Pabau’s purpose-built features for mental health and behavioral health practices at any scale.
Concerned about clinical note quality across franchise locations? Safer Clinical Notes outlines documentation practices that reduce liability and support audit readiness for multi-site practices.
Conclusion
The EHR that works for a single behavioral health location rarely survives contact with a franchise model. Billing fragmentation, permission gaps, and documentation rigidity compound at every new site you add. The operational cost of the wrong platform grows faster than the revenue from the new locations.
Pabau’s multi-location architecture supports behavioral health franchises with consolidated reporting, location-specific configuration, and integrated billing across sites from a single platform instance. If you are evaluating an ehr for multi-franchise mental health practice, see how Pabau handles the specific workflows your org structure requires: book a demo and walk through your actual multi-site setup.
Frequently Asked Questions
No single EHR is best for every franchise structure. The evaluation should focus on whether the system supports multi-entity BAAs, role-based permission hierarchies with at least four levels, consolidated billing with location-specific profiles, and configurable clinical templates by location. Pabau, Valant, and a small number of other platforms are built to handle these requirements at scale.
Most group practice EHRs aggregate data at the provider level, not the organizational level. Franchise-level reporting requires an additional aggregation layer that rolls up location performance into ownership-level dashboards. If the EHR does not natively support this, franchise owners typically build manual reports in spreadsheets, which introduces error and delay.
42 CFR Part 2 imposes consent and disclosure requirements for substance use disorder records that, in several areas, are stricter than standard HIPAA. SAMHSA’s Final Rule effective April 2024 brought Part 2 into closer alignment with HIPAA – most notably by allowing a single patient consent to authorize treatment, payment, and healthcare operations (TPO) disclosures – but Part 2 still imposes stricter requirements than HIPAA for disclosures outside TPO and for use of SUD records in civil, criminal, or administrative proceedings. For franchises, the practical implication is that the EHR must support data segregation that prevents SUD records from appearing in cross-location clinical summaries without the appropriate patient consent, and must reflect the post-2024 consent model in its consent-management workflows. Not all EHRs enforce this at the technical level – confirm this capability directly with the vendor before signing.
Ask whether the system flags state-specific telehealth restrictions when a provider is licensed in one state and attempting to schedule a session with a patient located in another. Ask how the system handles licensure verification for providers working across state lines and whether the platform integrates with interstate telehealth compact registries. These workflows are manual in most general-purpose EHRs.
SimplePractice serves over 250,000 practitioners according to its website and works well for solo and small group practices. Its customization for complex multi-location scenarios is limited, and pricing increases significantly at higher provider counts. Franchise owners with five or more locations and 20-plus providers typically find that platforms designed for enterprise or multi-site use cases offer better operational fit.