Key Takeaways
Package pricing creates predictable revenue and improves treatment compliance rates
Per-session billing offers flexibility but requires stronger collections management
Hybrid models balance insurance requirements with cash-pay incentives
Software automation reduces administrative burden for both pricing structures
Pelvic floor therapy pricing shapes more than how much patients pay per visit. It determines treatment compliance, revenue predictability, and operational complexity for physical therapy practices. Most clinics choose between two fundamental models: per-session billing tied to insurance reimbursement, or package-based pricing that bundles multiple sessions upfront. Each creates different financial outcomes, patient behaviors, and administrative workflows.
According to the American Physical Therapy Association, pelvic floor therapy typically requires 6-12 sessions over several months. Individual session costs range from $100 to $250, with geographic location and provider expertise driving variation. Insurance coverage complicates the picture: copays average $20-$60 per session, deductibles apply, and out-of-network rates push costs higher. The pricing model you select influences whether patients complete recommended treatment protocols and how predictably revenue flows into your practice.
Understanding Pelvic Floor Therapy Pricing Models
Physical therapy practices operate under constraints most other healthcare providers avoid. Insurance reimbursement rates rarely cover full clinical costs. Administrative overhead for claims management consumes staff time. Patients face out-of-pocket expenses that influence whether they return for follow-up sessions. Pelvic health clinics must balance clinical best practices against financial sustainability.
Per-session billing aligns with traditional insurance workflows. Each visit generates a separate claim using CPT codes like 97110 (therapeutic exercise) or 97530 (therapeutic activities). Patients pay their copay or coinsurance at checkout. Practices submit claims to insurers and wait 30-90 days for reimbursement. Cash flow depends on payer processing timelines and denial management efficiency.
Package pricing inverts this relationship. Patients prepay for a series of sessions-typically 6, 10, or 12 visits-at a discounted rate compared to individual session pricing. The practice receives full payment upfront. Revenue becomes predictable. Patients commit psychologically to completing treatment because they’ve already paid. But insurance complications arise: most payers don’t reimburse package purchases, forcing practices to operate outside insurance networks for package clients.
How Insurance Coverage Affects Pelvic Floor Therapy Pricing
In-network practices accept contracted reimbursement rates from insurance companies. These rates typically fall between $75 and $150 per session depending on CPT codes billed and regional fee schedules. Patient responsibility varies based on plan design: some pay flat copays of $20-$40, others pay percentage-based coinsurance of 10%-30% after meeting their deductible. High-deductible health plans can leave patients responsible for the full session cost until they hit $3,000-$5,000 in annual expenses.
Out-of-network billing gives practices more pricing control but shifts financial burden to patients. Many clinics charge $150-$250 per session when operating out-of-network. Patients submit superbills to their insurance company for potential partial reimbursement, but they pay the full session fee upfront. This model supports package pricing: since patients already bear most costs, prepaying for a series at a discount becomes attractive.
Package Pricing vs. Per-Session Billing: Financial Impact Analysis
A clinic seeing 120 pelvic floor therapy visits monthly faces different revenue patterns under each model. Per-session billing at $150 per visit generates $18,000 in gross charges. Insurance reimbursement averages 65%-75% of billed charges after contractual adjustments, yielding $11,700-$13,500 in actual collections. Collections occur 45-60 days post-service. Monthly revenue fluctuates based on payer processing delays and seasonal patient volume changes.
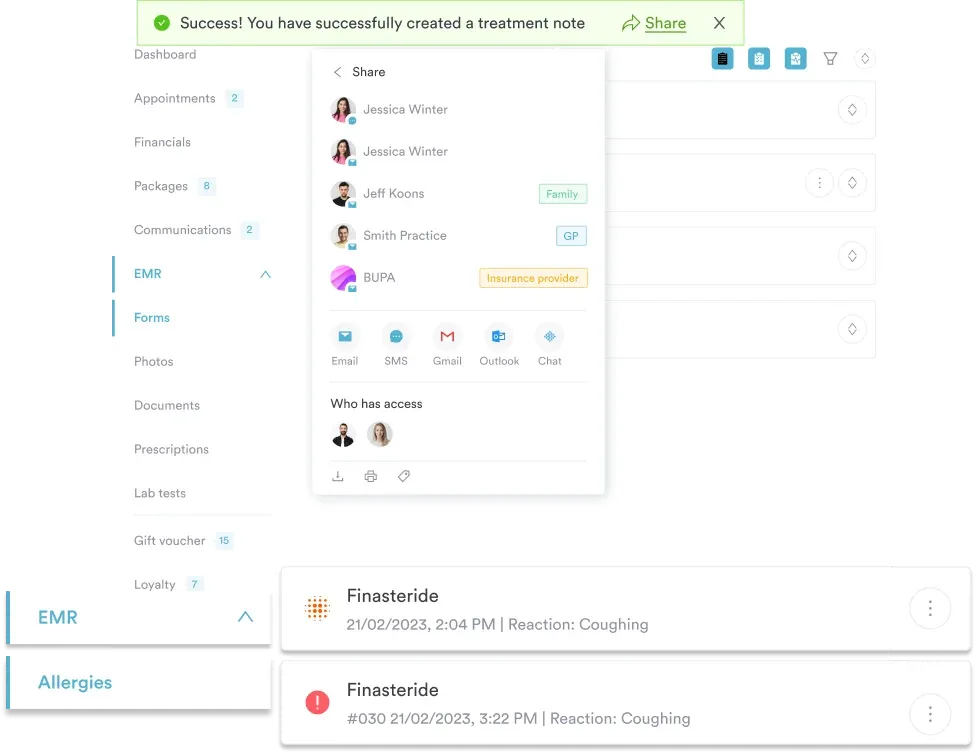
Package pricing with 20 clients purchasing 6-session bundles at $800 each produces $16,000 in immediate cash. No claims processing delays. No denial management overhead. Revenue certainty exists on day one. The practice sacrifices some per-visit revenue ($133 per session in packages vs. $150 per session individually) but gains operational simplicity and cash flow predictability.
Treatment Compliance Rates Under Different Pricing Models
Patients who prepay for therapy packages complete treatment at significantly higher rates than per-session payers. Financial commitment creates psychological momentum. A patient who bought a 10-session package but only attended 6 visits lost $320 of prepaid value. Loss aversion drives attendance. Per-session patients face no such barrier: skipping a visit costs nothing beyond the copay they would have paid anyway.
Clinical outcomes depend on completed treatment protocols. Pelvic floor dysfunction resolves through progressive neuromuscular re-education over multiple sessions. Patients who stop after 3-4 visits rarely achieve functional improvement. Package pricing aligns financial incentives with clinical best practices. Practices see fewer dropouts, better outcomes, and stronger referral generation from satisfied patients who completed care.
Automate Package Management and Revenue Tracking
Pabau tracks package session depletion, automates balance alerts, and provides revenue recognition reporting that distinguishes prepaid income from per-session billing. See how our system handles both pricing models seamlessly.

Financial Impact on Practice Revenue and Cash Flow
Revenue recognition rules differ sharply between models. Per-session billing records revenue when services are rendered and claims are submitted. Accounting systems recognize income in the month care was delivered, even though cash arrives 30-90 days later. This creates timing mismatches: payroll happens now, revenue arrives later. Practices need working capital reserves or credit lines to cover operational gaps.
Package sales generate deferred revenue liabilities. When a patient prepays $900 for 9 sessions, the practice receives cash immediately but can only recognize revenue as sessions are delivered. Month one might see $300 in earned revenue (3 sessions delivered) while $600 remains as a liability on the balance sheet. Payment processing systems must track remaining balances and automate session depletion to maintain accurate books.
Break-even analysis reveals when each model becomes profitable. A per-session practice with $8,000 monthly overhead needs 60-65 sessions at $130 average reimbursement to cover costs. A package-focused practice with the same overhead reaches break-even at 55 sessions because average revenue per session increases to $145 after accounting for package discounts and improved attendance rates. Fewer sessions required for profitability creates capacity for growth or allows practitioners to see fewer patients while maintaining income.
Managing Insurance Billing Alongside Package Pricing
Hybrid models combine both approaches. Practices bill insurance for initial evaluations and covered sessions while offering cash-pay packages for sessions beyond insurance limits. Many pelvic floor therapy plans cover only 6-12 visits annually. Patients needing ongoing care face full out-of-pocket costs after benefits exhaust. A package offer at this transition point captures revenue that would otherwise be lost to patient dropout.
Claims management software tracks both billing streams without confusion. Pabau’s system flags when patients approach their insurance visit caps, triggering automatic package offers. Staff see remaining covered sessions alongside package balances in a unified patient record. This prevents double-billing errors and ensures accurate revenue allocation across payment types.
Pro Tip
Track insurance authorization limits in your practice management system and set automated alerts when patients have 2-3 covered visits remaining. Present package options proactively before benefits exhaust rather than reactively after patients face unexpected out-of-pocket bills. Conversion rates on pre-emptive package offers run 40-60% higher than post-exhaustion offers.
Operational Considerations for Implementation
Staff training requirements differ between pricing models. Per-session billing demands insurance verification expertise: staff must check coverage, understand authorization requirements, calculate patient responsibility, and submit clean claims. Package sales require consultative selling skills: explaining value propositions, overcoming price objections, and structuring payment plans. Most practices need different team members handling each function.
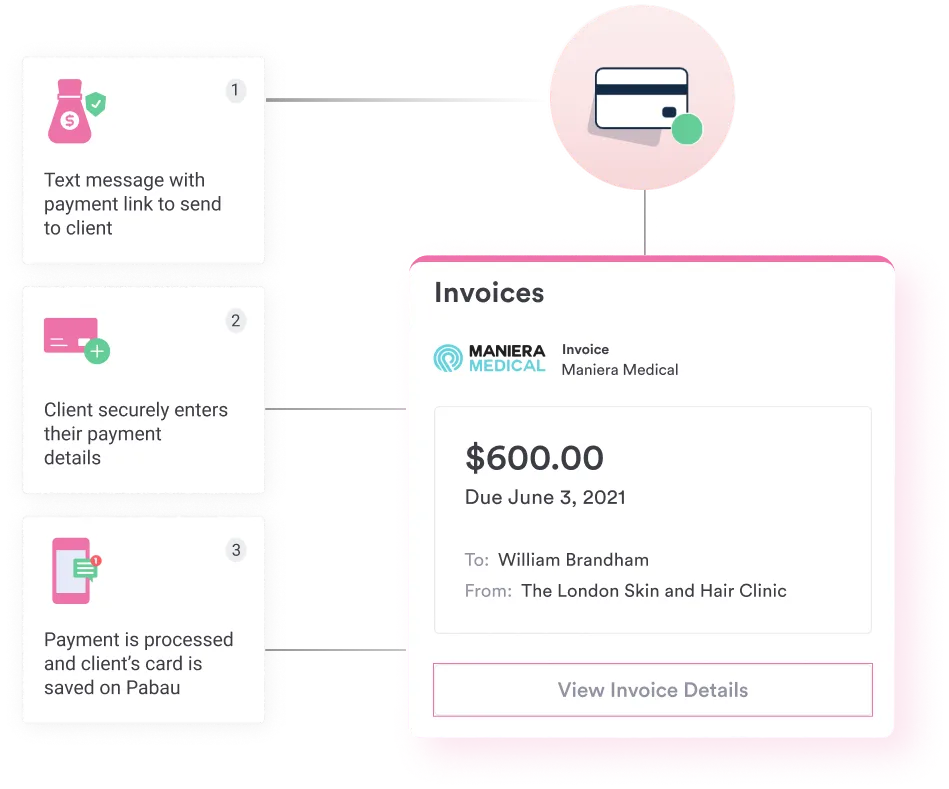
Technology infrastructure shapes operational success. Practices operating per-session billing need robust clearinghouse integrations, denial management workflows, and aging accounts receivable tracking. Package-based operations require prepayment processing, automated session counting, and prorated refund calculations for unused services. Physical therapy EMR systems like Pabau support both models within the same platform, eliminating the need to maintain separate systems for different revenue streams.
Compliance considerations vary by state. Some jurisdictions regulate prepaid service agreements for healthcare providers. California requires written contracts exceeding $500 to include cancellation rights and refund terms. Texas mandates surety bonds for certain prepaid healthcare arrangements. Practices must consult local regulations before implementing package pricing to ensure legal compliance and consumer protection requirements are met.
Setting Package Pricing That Drives Adoption
Discount structures influence purchase decisions without sacrificing profitability. A 15%-20% discount on package purchases compared to per-session rates creates enough incentive for uptake while maintaining healthy margins. For example, if individual sessions cost $175, a 10-session package priced at $1,500 ($150 per session) offers 14% savings. Patients perceive value. The practice gains $1,500 in immediate cash flow rather than waiting months for insurance reimbursement on 10 separate claims.
Session count options matter. Offering 6-session, 10-session, and 12-session packages accommodates different patient needs and budgets. New patients uncertain about commitment choose smaller packages. Returning patients with established relationships select larger bundles. Flexibility increases overall package adoption rates by removing barriers to entry.
Expert Picks
Need structured pricing guidance for specialty services? How to Choose Med Spa Pricing Strategy covers package design principles that apply across clinical specialties.
Evaluating practice management systems that support both models? Practice Management Software: Complete Guide breaks down automation capabilities for revenue cycle management.
Planning operational workflows for hybrid billing? Patient Scheduling and Appointment Management explains how integrated systems prevent scheduling conflicts between insurance and package clients.
Conclusion
Pelvic floor therapy pricing models create fundamentally different practice operations. Per-session billing aligns with insurance workflows but introduces cash flow unpredictability and administrative complexity. Package pricing generates immediate revenue and improves treatment compliance but operates primarily outside insurance networks. Most successful practices run hybrid models: billing insurance when coverage exists, offering packages when benefits exhaust or patients prefer cash-pay simplicity.
Financial outcomes depend on implementation quality. Practices need staff trained in both insurance verification and consultative sales. Technology must automate session tracking, revenue recognition, and balance management across payment types. Compliance with state regulations governing prepaid services protects both practice and patients. The pricing model that works best depends on your patient population, insurance mix, and operational capacity-but understanding the mechanics of each ensures you make informed decisions that support sustainable growth.
Frequently Asked Questions
Individual session costs range from $100 to $250 depending on geographic location, provider expertise, and clinic setting. In-network insurance reimbursement typically falls between $75 and $150 per session. Out-of-network cash-pay rates average $150-$250. Patient responsibility varies based on insurance plan design, with copays ranging from $20 to $60 per visit.
Package pricing bundles multiple sessions at a discounted rate, typically 15%-20% below individual session costs. Patients prepay upfront, creating immediate cash flow for practices. Per-session billing processes each visit separately through insurance, resulting in 30-90 day payment delays. Package pricing improves treatment completion rates but operates outside most insurance networks. Per-session billing integrates with insurance workflows but requires stronger collections management.
Yes, hybrid models bill insurance for covered sessions while offering cash-pay packages when benefits exhaust. Most insurance plans cover 6-12 pelvic floor therapy visits annually. Patients needing additional care face full out-of-pocket costs after authorization limits. Practices present package options at this transition point, capturing revenue that would otherwise be lost to patient dropout. Practice management software must track both payment streams to prevent billing errors.
Discounts of 15%-20% off per-session rates create sufficient incentive for package adoption without sacrificing profitability. If individual sessions cost $175, a 10-session package at $1,500 ($150 per session) offers 14% savings. Patients perceive value while practices gain immediate cash flow. Larger packages typically justify slightly higher discount percentages to encourage upfront commitment.
When patients prepay for multiple sessions, practices receive cash immediately but can only recognize revenue as services are delivered. A $900 prepayment for 9 sessions creates a liability on the balance sheet. Revenue recognition occurs session by session: 3 sessions delivered equals $300 in earned revenue and $600 in remaining liability. Practice management systems must automate session depletion tracking to maintain accurate financial records.